Mouth Sores
Reader-supported. We may earn a commission from links on this page. Advertising disclosure.
In this article
Mouth sores are painful ailments that appear on the soft tissues of your mouth. They affect your ability to eat, drink, practice dental hygiene, and talk.
But you might be wondering if mouth sores are serious or contagious. Below we break down everything you need to know about mouth sores, including at-home remedies.
What Do Mouth Sores Look Like?
While mouth sores look different depending on the cause, they are typically a different color from surrounding tissue and can appear red, purple, yellow, or white.
They may develop on any of your mouth’s soft tissues, including your:
- Lips
- Cheeks
- Gums
- Tongue
- Floor of the mouth
- Roof of the mouth (soft palate)
You may also have sores and inflammation in your esophagus, the tube that connects your throat to your stomach. A tingling or burning sensation may occur a day or two before the sores develop.
Different Types of Mouth Sores And Their Causes
Mouth sores include various conditions that are often mistakenly lumped together. However, these sores differ in cause, appearance, and treatment.
These include:
1. Canker Sores
Canker sores (aphthous ulcers) develop within the oral cavity. They appear as small ulcers with a white, yellow, or gray center and a flat red border.
Canker sores typically appear as small ulcers with a white, yellow, or gray center and a red border. Before additional symptoms emerge, a canker sore may cause a tingling or burning sensation.
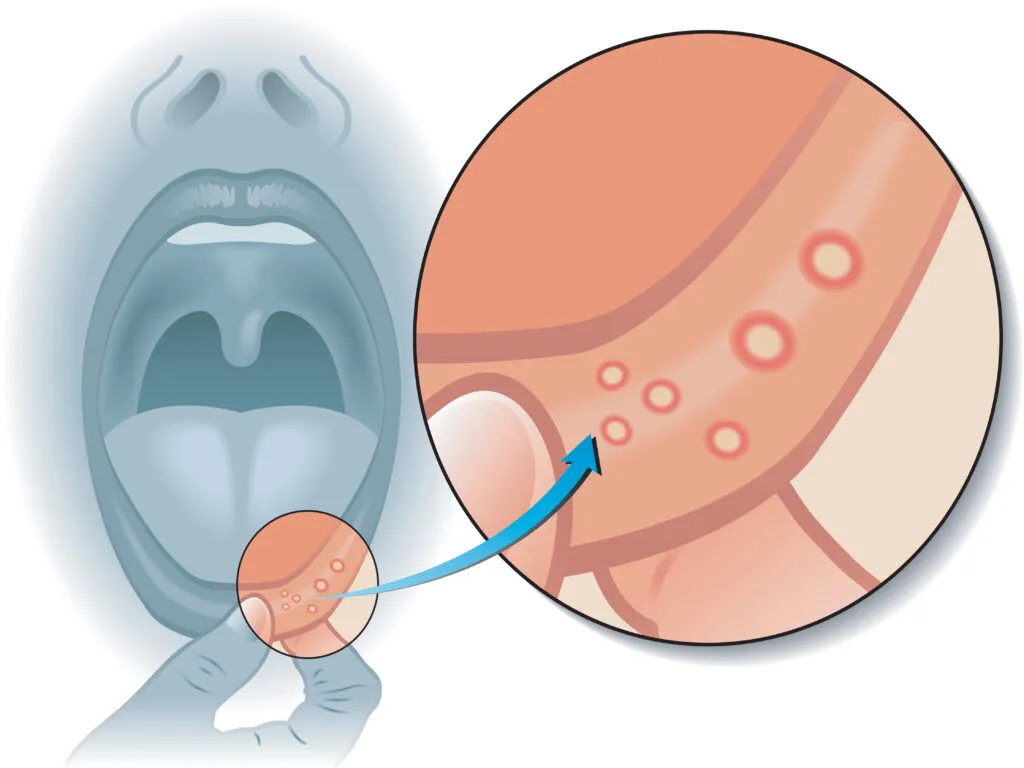
Severe canker sores may sometimes have a large diameter and a raised edge. Fortunately, most heal on their own within 7 to 10 days.
There is limited research on the exact cause of canker sores. However, scientists have linked the condition to genetics. Other triggers include fatigue, stress, physical trauma, and citrus or acidic foods.
2. Cold Sores
Cold sores are painful, fluid-filled blisters that form in clusters (fever blisters) caused by the herpes simplex virus (HSV). These sores typically appear on the border of the lips, called the vermilion border.
HSV can spread through nonsexual contact, such as kissing, touching an infected person’s skin, or sharing infected objects like lip balm. Once infected with herpes, the virus remains dormant in the body. ese sores typically appear on the border of the lips, called the vermilion border.
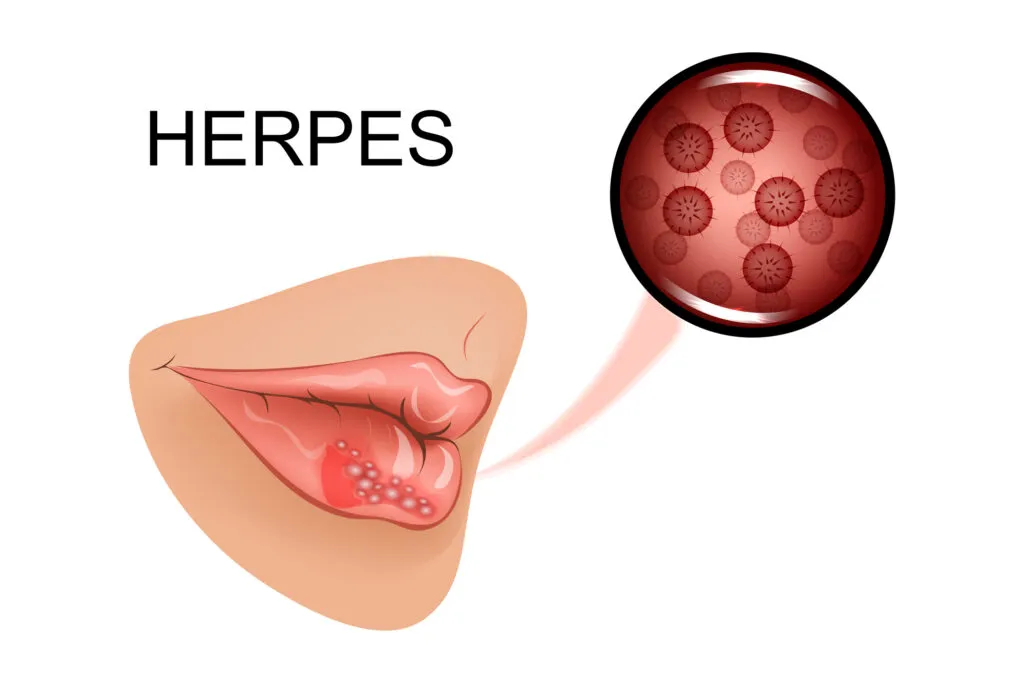
Sores may appear when the virus reactivates and typically heal within 1 to 2 weeks (often 5 to 15 days). Additionally, several factors, including wind, sun, fever, or stress, can trigger a ‘flare-up.‘
3. Candida
Candida, also called oral thrush or moniliasis, is a yeast infection that causes creamy white and red spots on the mouth’s surfaces. An overgrowth of Candida fungus often causes it.
It’s most common among the very young, the elderly, and people with a weakened immune system, such as patients with diabetes or AIDS. It is also common among denture wearers.
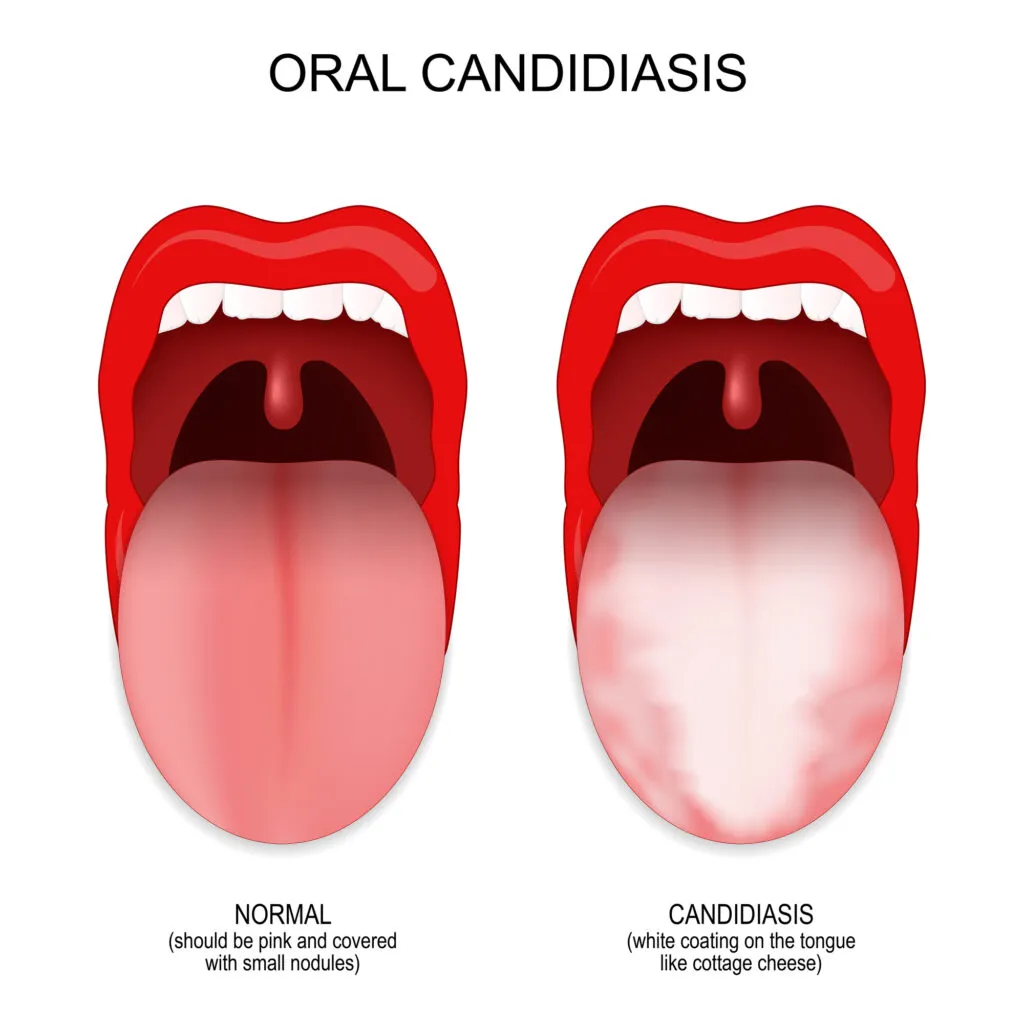
This condition may be painful. It can also cause foul breath and trouble eating and swallowing.
4. Leukoplakia
Leukoplakia is when a white or gray patch develops inside the mouth, typically under the tongue or on the inside of your cheeks. It’s caused by abnormal cell growth in the mouth lining.
Patches of leukoplakia appear gradually and may regress if the source of irritation (e.g., tobacco) is removed, but many persist and require monitoring or surgical removal.
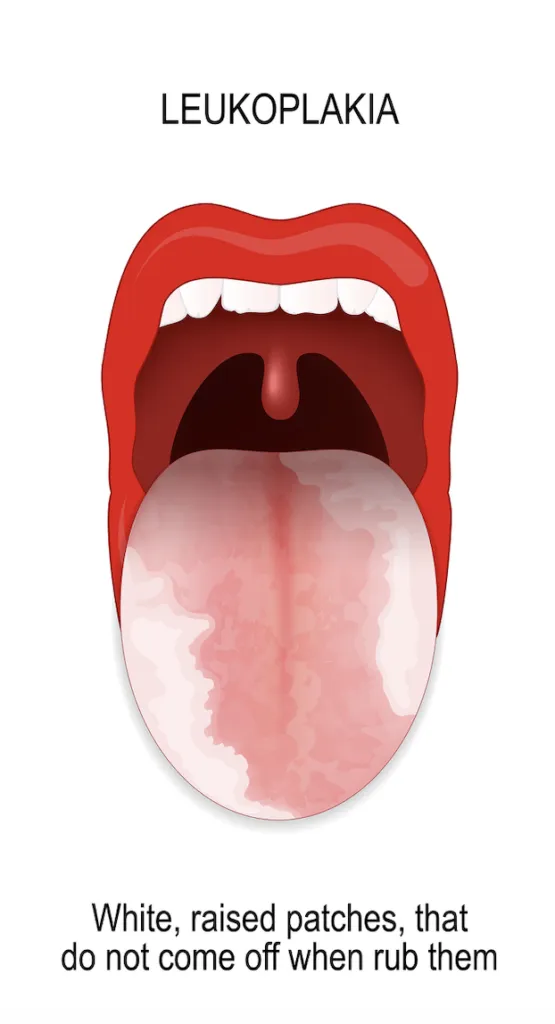
Leukoplakia differs from other causes of white spots as it can progress to oral cancer. Common causes of these mouth sores include:
- Smoking or chewing tobacco
- Certain foods
- Cheek biting
- Irregular dental restorations
- Damaged teeth
5. Erythroplakia
Erythroplakia is a red, velvety lesion that may appear anywhere in the mouth. It is most often found on the gum tissue behind the back teeth or the floor of the mouth.
The cause of erythroplakia is unclear, although it is most often linked to alcohol and tobacco consumption. Chronic inflammation and poor diet can also play a role.
Erythroplakia is less common than leukoplakia. However, biopsies reveal that some of these sores are precancerous or malignant.
6. Oral Cancer
White or red lesions, lumps, or ulcers in the mouth may all be signs of mouth cancer. Mouth cancer often starts small and painless, but rapidly grows and spreads.
Most oral cancers are detected during routine medical checkups. The sores from oral cancer may appear on the lips, tongue, gums, or the roof of your mouth.
Contributing factors to oral cancer include smoking cigarettes, using smokeless tobacco, and consuming alcoholic beverages. According to experts, tobacco use accounts for an estimated 75 to 90% of oral cancer cases, varying by population and study.
7. Celiac Disease
Celiac disease is an autoimmune disease where the consumption of gluten, a protein found in wheat and other grains, damages the lining of your small intestine.
People with celiac disease often experience outbreaks of canker sores or aphthous ulcers. The symptoms can improve by adopting a gluten-free diet.
8. Hand, Foot, and Mouth Disease
Hand, foot, and mouth disease (HFMD) is a viral illness common in children under five. It usually starts with a fever and rashes on the hands and feet.
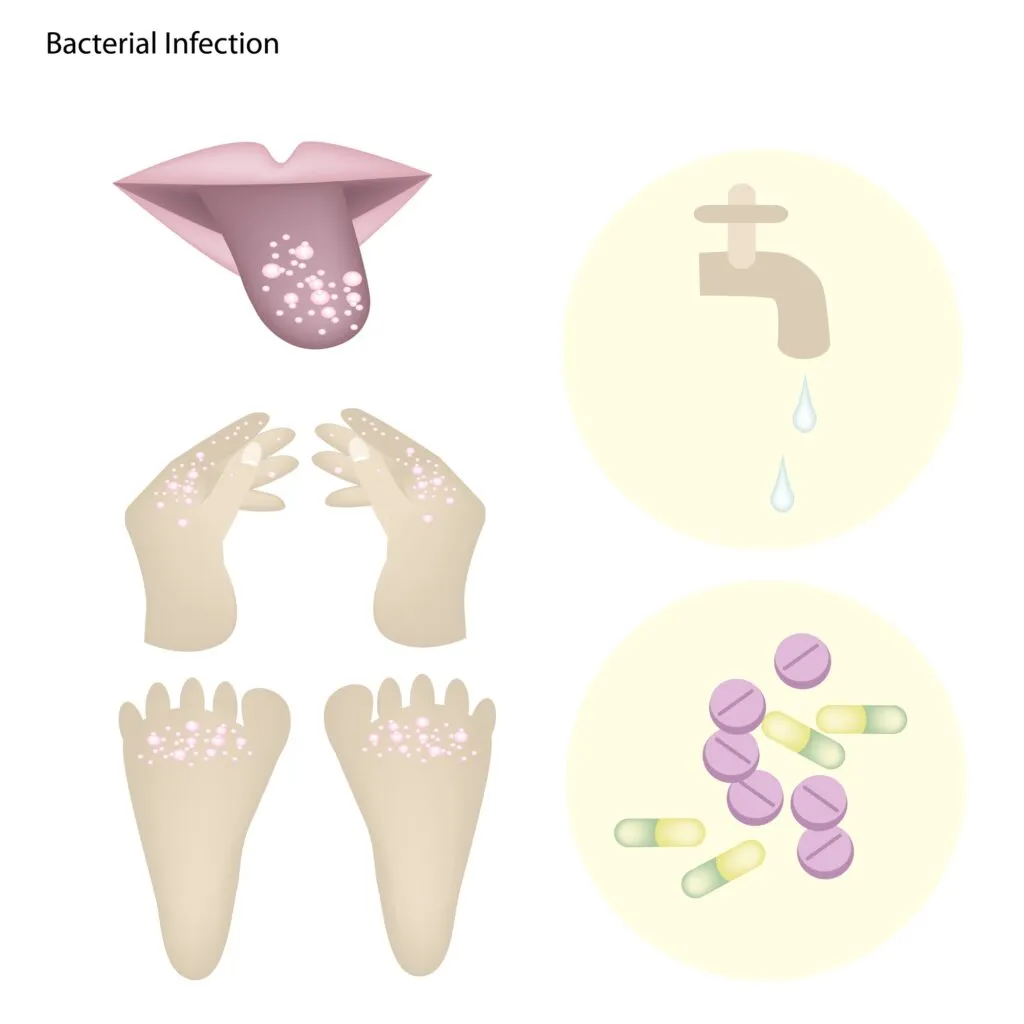
HFMD can also affect the mouth and tongue, causing mouth sores. The viruses that cause HFMD spread quickly between people who come into close contact with each other. These viruses include:
- Coxsackievirus A16
- Coxsackievirus A6
- Enterovirus 71 (EV-A71)
Mild symptoms of HFMD usually resolve within 7 to 10 days.
Are Mouth Sores Serious?
Mouth sores, including canker sores (aphthous ulcers), are typically harmless and last just a week or two. However, mouth sores may indicate oral cancer or a viral infection, such as herpes simplex virus (HSV), and in some cases, require professional care.
According to Dr. Nandita Lilly, one of NewMouth’s in-house dentists, “Mouth sores are a fairly common ailment among the population, and fortunately, your dentist may be able to help reduce pain, control the outbreaks, and even diagnose early signs of oral cancer.”
How Are Mouth Sores Treated?
Most mouth ulcers will heal without treatment. However, if your mouth ulcers are frequent and painful, going to a healthcare provider or dentist is the best way to rule out any underlying issues.
Treatment options include:
- Over-the-counter (OTC) anesthetics — Topical anesthetic benzocaine gels can relieve pain, while prescription corticosteroid fluocinonide gels reduce inflammation.
- Protective patches — Protective patches create a barrier, allowing ulcers to heal faster by minimizing irritation during eating.
- Prescription antivirals — Antiviral medications (like acyclovir) effectively shorten cold sore outbreaks if applied during the early signs of tingling.
- Corticosteroids — Topical corticosteroids reduce inflammation significantly, ideal for persistent or very painful aphthous ulcers.
- Low-level laser therapy (LLLT) — This provides instant pain relief and shortens healing time.
- Chemical cautery — This procedure cauterizes the sore with a tiny stick coated in silver nitrate, which may similarly alleviate pain, though it is less effective than a laser.
Your doctor will order a biopsy for further examination if mouth cancer is suspected. If oral cancer is detected, your doctor will prepare a treatment plan, including surgery or chemotherapy.
Home Remedies for Mouth Sores
Mouth sores don’t always require a visit to your doctor, and if you’re dealing with minor pain, you can likely treat the ailment at home.
The most effective home remedies for mouth sores include the following:
- A saltwater mixture can help dry out a mouth sore for quicker healing. Mix one teaspoon (tsp) of salt with ½ cup of water, gargle, and rinse. Don’t swallow it.
- Baking soda can minimize the bacteria in the mouth, while a salt mixture can help dry out a mouth sore for quicker healing. Mix one part baking soda with one part water, gargle, and rinse. Do not swallow the mixture.
- Milk of magnesia can help to dry out the sores. Apply a small amount to the lesion several times a day. The medication will coat the mouth sore, relieving irritation and pain.
- Placing a cold compress over the sore can temporarily relieve any painful sensation caused by the sore. Never put ice directly on the sore.
- For a severe mouth sore, a steroid mouthwash containing the ingredient dexamethasone can assist with healing and prevent a mouth sore from worsening.
- Mouth sores are often found in people with nutritional deficiencies. Frequent mouth sores can indicate low zinc, folic acid, iron, and vitamin B12 levels. A blood test can rule out or confirm nutritional deficiencies.
When Should You Call a Dentist or Doctor?
If your mouth sores occur frequently, it may be time to see a doctor. Seek immediate medical attention if you notice any of the following:
- Sores lasting longer than two weeks
- Non-painful sores in one or more areas of the mouth
- Ulcers larger than one centimeter or clusters that bleed
- Rapidly spreading sores
- Mouth sores developing after starting a new medication
- Systemic symptoms, such as fever, weight loss, or swollen lymph nodes
- Difficulties with eating or breathing
Expect your dentist or oral medicine specialist to consider biopsies or blood tests to rule out serious conditions, including oral cancer or autoimmune diseases.
How To Prevent Mouth Sores
The best way to prevent mouth sores is by practicing good oral hygiene, by brushing and flossing regularly. Use a toothbrush with soft bristles to prevent irritation, and visit your dentist regularly for checkups.
You can also prevent mouth sores through lifestyle changes, including:
- Improving iron, folate, vitamin B12, and zinc levels.
- Avoid using irritating toothpaste containing sodium lauryl sulfate (SLS).
- Avoid alcohol consumption and tobacco use.
Talk to your healthcare provider to find out if you have nutrient deficiencies that cause mouth sores.
Mouth Sores
NewMouth PodcastSources
- López‑García et al. “Treatment of Recurrent Aphthous Stomatitis: A Systematic Review.” Medicina Oral, Patología Oral y Cirugía Bucal, 2023.
- Jian et al. “Thalidomide for Recurrent Aphthous Stomatitis: A Systematic Review and Meta‑Analysis of Randomized Controlled Trials.” BMC Oral Health, 2024.
- Panel on Opportunistic Infections in Adults and Adolescents with HIV. “Guidelines for the Prevention and Treatment of Opportunistic Infections in Adults and Adolescents with HIV: Candidiasis (Mucocutaneous).” National Institutes of Health, 2024.
- Plewa M.C., & Chatterjee K. “Recurrent Aphthous Stomatitis.” Treasure Island (FL): StatPearls Publishing, 2023.
- Al‑Maweri et al. “Efficacy of Hyaluronic Acid for Recurrent Aphthous Stomatitis: A Systematic Review.” BMC Oral Health, 2022.

Certified physician assistant with 20 years experience. Owns virtual care practice and advocates for patients.
Related Articles

Best Natural Remedies for Treating Gum Disease
Having a good oral care routine is a great way to prevent gum disease and build the foundation for healthy gums. But the...

Best Foods for Healthy Teeth and Gums
What you eat plays a crucial role in maintaining a healthy mouth, and below we cover the best foods to incorporate into...
Dental Abscess: Identifying and Treating It at Home
Although minor infections may heal on their own, neglecting dental abscesses can put you at risk of short and long-term...
What Food Should You Avoid To Maintain Good Oral Health?
When it comes to teeth, sometimes the tastiest foods can be the biggest culprits in creating problems. Bacteria in your...
