What is Gum Disease: How To Prevent and Treat It
Reader-supported. We may earn a commission from links on this page. Advertising disclosure.
In this article
Gum disease, also known as periodontal disease, is an infection and inflammation of the gums and the structures supporting the teeth. It is a widespread issue, affecting nearly half of adults over 30 in the United States alone, with severe cases impacting around 9% of the population.
Understanding gum disease is crucial for maintaining oral health, as it can lead to severe complications such as tooth loss and can worsen other chronic conditions like diabetes.
Here we share information about gum disease, its causes, how to prevent it, and its treatment options.
What Are the Causes of Gum Disease?
Gum disease is an inflammatory condition affecting the gums and bones supporting the teeth. It ranges from mild inflammation (gingivitis) to severe damage to the soft tissue and bone (periodontitis).
The most common cause of gum disease is plaque and tartar. Plaque is a sticky film of bacteria that forms on teeth.
If not removed through regular brushing and flossing, it hardens into tartar, which can only be removed by a dental professional. The bacteria in plaque and tartar cause inflammation and infection of the gums.
Risk Factors of Gum Disease
Several factors increase the risk of developing gum disease, such as:
- Smoking — One of the most significant risk factors, smoking impairs the immune system, making it harder to fight off gum infections.
- Poor oral hygiene — Inadequate brushing and flossing allow plaque to build up and harden into tartar.
- Genetics — Some people are genetically predisposed to gum disease, even with good oral care.
- Age — Older adults have higher rates of gum disease, with over 70% of those aged 65 and older affected.
- Hormonal changes — Pregnancy, menopause, and other hormonal changes can make gums more sensitive and susceptible to gum disease.
- Illnesses — Conditions like diabetes, cancer, and HIV/AIDS can affect the gums and increase the risk of infections.
- Medications — Certain medications can reduce saliva flow, leading to dry mouth and an increased risk of gum disease.
- Stress — It can weaken the immune system and increase inflammation, contributing to gum disease.
How Can You Prevent Gum Disease?
Visiting your dentist twice a year is a proven method to prevent gum disease. Routine check-ups allow for early detection of gum disease and other oral health issues, and professional cleanings can remove plaque and tartar missed by regular brushing and flossing.
If you can’t see your dentist regularly, practice proper toothbrushing to ensure plaque is effectively removed from all surfaces of the teeth.
Here are our tips for proper brushing techniques:
- Use fluoride toothpaste
- Angle the bristles of your toothbrush toward the gum line
- Brush gently using small, circular motions for at least two minutes twice a day
- Floss between the teeth to remove plaque biofilm trapped where your toothbrush can’t reach
- Rinse with an antiseptic mouthwash after brushing and flossing
What is the Proper Flossing Technique?
The correct flossing technique involves using a string of floss about two feet long, wrapping it around the middle fingers, and gripping it between the thumb and index fingers.
Gently ease it between the teeth until it reaches the gumline. The floss should be curved like the letter ‘C’ around each tooth and slid up and down under the gum.
Can Better Lifestyle Choices Prevent Gum Disease?
A healthy diet plays a significant role in promoting healthy gums. Foods rich in vitamins and minerals, such as fruits, vegetables, and dairy products, support good oral hygiene and help prevent gum disease.
You can also quit smoking to greatly reduce the risk of developing gingivitis and periodontitis. Smoking impairs blood flow to the gums and can affect the immune response.
We also recommend incorporating stress-reducing activities such as exercise, meditation, and adequate sleep into your routine to support overall health, including oral health.
How is Gum Disease Diagnosed?
Finding gum problems early is very important to prevent their worsening. By checking your mouth yourself for signs and seeing a dentist, you can keep your mouth healthy and avoid serious problems.
Self-Examination for Gum Disease
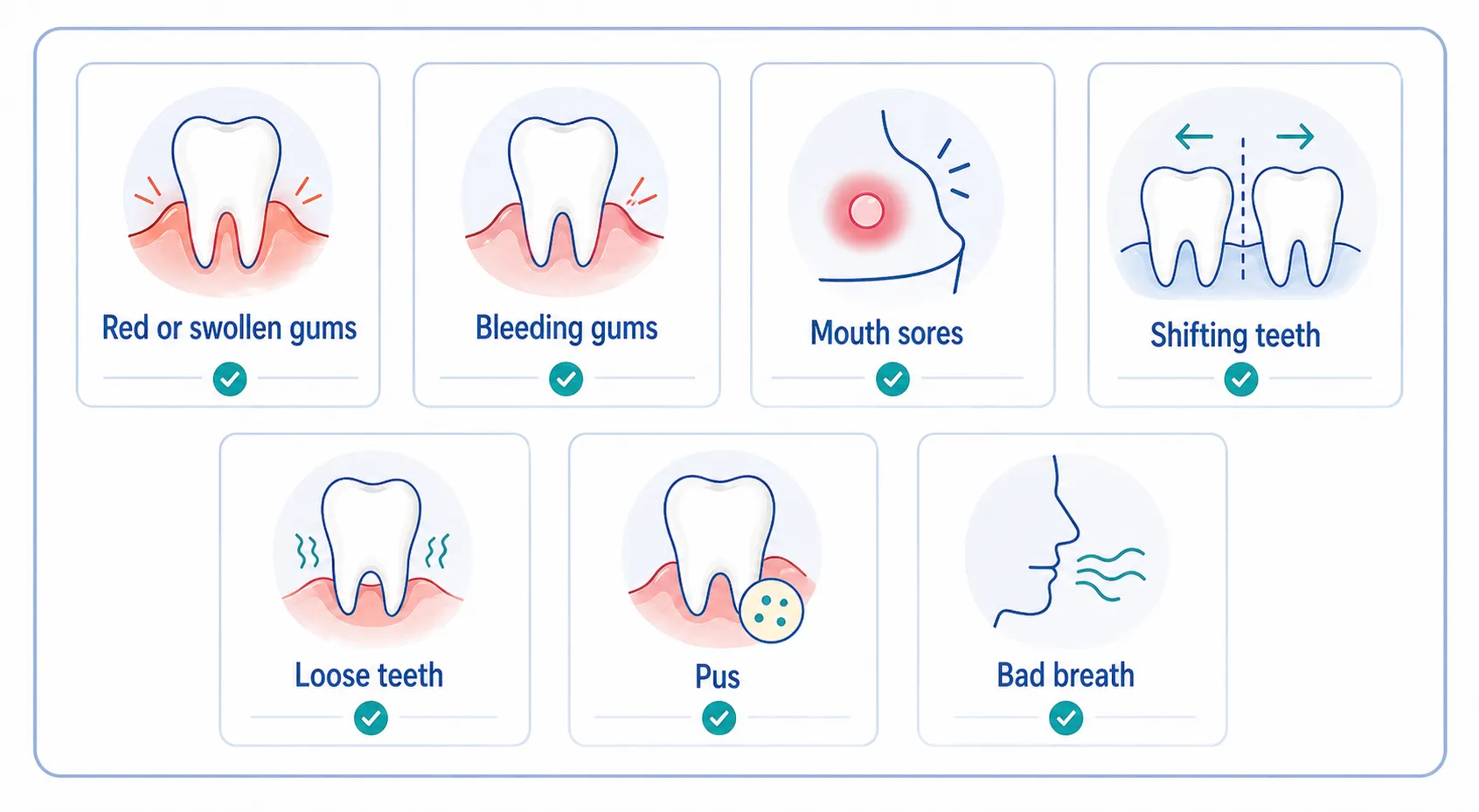
Here are some signs to look for when doing self-examination:
- Red, swollen, or tender gums — Healthy gums should be a comfortable pink color. Redness and swelling can indicate inflammation and early gum disease.
- Bleeding gums — Gums that bleed during brushing or flossing are not normal and may be a sign of gingivitis, the early stage of gum disease.
- Mouth sores — Sores in the mouth can be a symptom of periodontal disease and should be evaluated by a dentist.
- Shifting teeth — If your teeth seem to have shifted or fit together differently when you bite, it could be a sign of periodontitis.
- Loose teeth — Advanced gum disease can cause teeth to become loose due to the destruction of the supporting bone and tissue.
- Pus — The presence of pus between the teeth and gums is a clear sign of infection and advanced gum disease.
- Bad breath — Persistent bad breath or a bad taste in the mouth can be indicative of gum disease.
Professional Diagnosis
At your dental check-up, your dentist will learn more about your overall health to see if anything might be affecting your gums. Then, they’ll take a close look at your mouth to check for any swelling, redness, or sores.
They’ll also measure the space between your teeth and gums—deeper spaces can be a sign of gum disease. Finally, they might take X-rays to check for damage to the bone underneath your gums, which can happen with advanced gum disease.
Gum Disease Diagnostic Tools
Modern dental practices use various diagnostic tools to detect gum disease:
- Digital imaging — X-rays and other imaging technologies help visualize the extent of bone loss and other issues not visible to the naked eye.
- Periodontal probes — These tools measure the depth of gum pockets to assess the severity of gum disease.
- Biomarker analysis — Saliva and gingival crevicular fluid can be tested for biomarkers that indicate the presence and severity of periodontal disease.
Treatment Options for Gum Disease
Fortunately, different treatment options for gum disease are available. Non-surgical treatment options include scaling and root planing.
Your dentist will remove plaque and tartar from the surface of the teeth and below the gumline. The procedure may require local anesthesia to minimize discomfort and can take multiple.
Antibiotics are particularly effective in reducing bacterial load and inflammation, which helps in the healing process. They can be administered orally or applied directly to the gums, depending on the severity of the condition.
Surgical treatment options for gum disease include:
- Flap surgery — It involves making small incisions in the gum to lift it away from the teeth, followed by thorough cleaning and then suturing the gum back in place.
- Bone and tissue grafts — These are procedures used to replace lost bone and gum tissue. They help restore the structural integrity of the teeth and gums, promoting stability and health.
Guided tissue regeneration—This procedure involves placing a special membrane between the bone and gum tissue, allowing the bone and connective tissue to regenerate. It’s useful in treating advanced cases of periodontitis where significant bone loss has occurred.
What is Gum Disease: How To Prevent and Treat It
NewMouth PodcastSources
- AlJehani, Y. A. “ Risk Factors of Periodontal Disease: Review of the Literature.” International Journal of Dentistry, 2014.
- “Gum Disease Risk Factors.” American Academy of Periodontology.
- Van Dyke, T. E., & Dave, S. “Risk Factors for Periodontitis.” Journal of the International Academy of Periodontology, 2004.
- “Why Your Gums Are so Important to Your Health?” Harvard Health, 2023.
- Nazir, M. A. “Prevalence of Periodontal Disease, Its Association With Systemic Diseases and Prevention.” International Journal of Health Sciences, 2017.
- Chapple, I. L. “Time to Take Gum Disease Seriously.” British Dental Journal, 2022.
- “The Importance of Flossing.” National Dental Care.
- “Gingivitis and Periodontitis: What Are the Advantages and Disadvantages of Professional Teeth-Cleaning?” Institute for Quality and Efficiency in Health Care (IQWiG), 2006.
- Ko, J., et al. “The Chairside Periodontal Diagnostic Toolkit: Past, Present, and Future.” Diagnostics, 2021.
- Ramenzoni, L. L., et al. “Oral Diagnostic Methods for the Detection of Periodontal Disease.” Diagnostics, 2021.

UCLA-trained dentist practicing in public health. Focuses on whole-body approach to dental care.
Related Articles
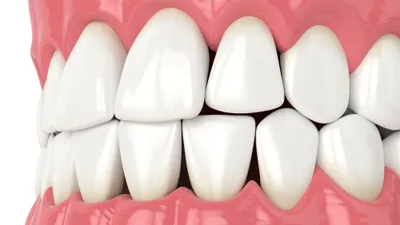
Black Triangles Between Your Teeth
When you look in the mirror, you may notice small black triangles between your teeth. These are gaps that your gum tissu...

Tight Jaw Causes, Tips for Relief, and Prevention
Why Does My Jaw Feel Tight? There are many potential causes of a tight jaw. Your lifestyle, jaw disorders, and certain i...

What are the Underlying Causes of Strawberry Tongue?
Key Takeaways Strawberry tongue is a type of tongue inflammation. It causes a swollen, red, bumpy appearance, similar to...

What are Mamelons on Teeth?
You might wonder, "What are those little bumps on my child's new adult teeth?" They're called mamelons and are a normal...
