Sleep Apnea - Symptoms, Causes, and Treatment Options
Reader-supported. We may earn a commission from links on this page. Advertising disclosure.
In this article
Sleep apnea is a condition that causes short interruptions in breathing while sleeping. It affects around 936 million adults worldwide.
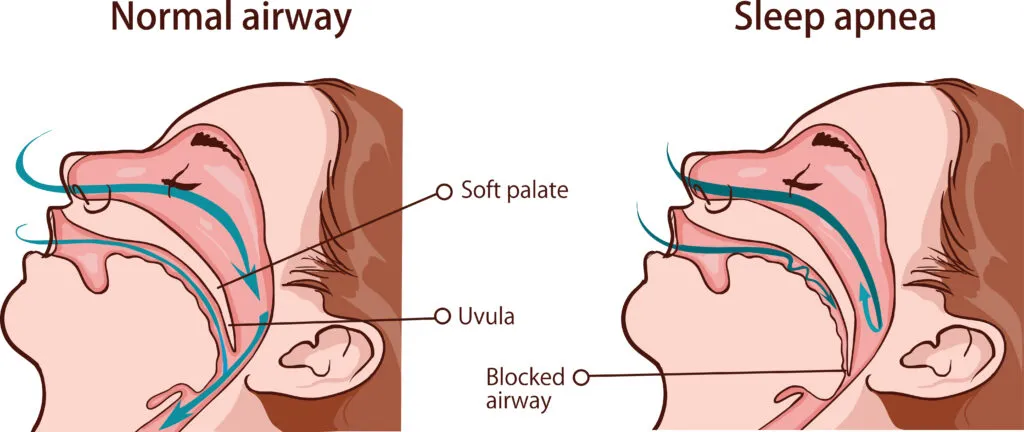
Leaving sleep apnea untreated can be dangerous. Because it starves the body of oxygen, the condition can lead to severe health problems, including high blood pressure, heart disease, and stroke.
Here we cover the different types of sleep apnea, its causes, and possible treatment options.
What Are the Symptoms of Sleep Apnea?
The three most common sleep apnea symptoms are:
- Abrupt awakenings accompanied by choking or gasping for air
- Breathing that starts and stops suddenly
- Frequent, loud snoring
These 3 symptoms aren’t the only effects you may notice. Some people also experience:
- Excessive daytime sleepiness
- Restless sleep
- Trouble falling asleep
- Dry mouth
- Morning headaches
- Sexual dysfunction
- Waking during the night to urinate
- Mood changes
Children with sleep apnea may have trouble concentrating in school, experience bedwetting, or have worsening asthma symptoms.
What Are the Causes of Sleep Apnea?
The cause of sleep apnea depends on the type a person has. For example, the causes of OSA and CSA will vary. Additionally, not every instance of sleep apnea stems from the same root cause.
Causes of OSA include:
- Relaxation of muscles in the throat
- The tongue falling backward to block the airway
- Accumulation of fat around the upper airway
- Enlarged tonsils or adenoids blocking the airway
- Narrowed airway from certain conditions
Meanwhile, potential causes of CSA are:
- Heart or kidney failure
- Medications such as opioids
- High altitudes
- Neurological conditions
- Stroke or brain infection
Mixed sleep apnea syndrome may result from a mixture of the causes of OSA and CSA.
Who’s at Risk for Sleep Apnea?
Anyone may develop sleep apnea, but certain risk factors make a person more prone to it. These factors include:
- Older age — Studies show that as you age, the more likely you are to experience chronic sleep disorders, including sleep apnea.
- Being male — Men are two to three times more likely than women to be diagnosed with sleep apnea.
- Weight — Having a higher body weight can increase your risk of developing sleep apnea, as it may apply pressure to your airway and narrow it.
- Genetics — Having a family history of sleep apnea puts you at a higher risk.
- Narrowed airway — Some people have a narrower airway than others due to hereditary or other medical conditions. The more narrow your throat, the likelier you are to develop sleep apnea.
- Alcohol use — Alcohol can relax your throat muscles, which is one cause of obstructive sleep apnea.
- Smoking — Research has uncovered a strong correlation between smoking and obstructive sleep apnea. It can increase inflammation and fluid retention in the airway.
- History of stroke or heart failure — Stroke and heart failure are known causes of central sleep apnea.
- Certain medical conditions — Other medical conditions, such as high blood pressure or hormonal disorders, may raise your likelihood of developing sleep apnea.
- Opioid use — Opioid medications, especially in the long term, can increase your risk of sleep apnea.
- Anatomic traits — Certain anatomic traits, like having a thick neck or large tonsils, may affect your potential for OSA.
What Are the Types of Sleep Apnea
There are three main types of sleep apnea, which have different causes and complications:
1. Obstructive Sleep Apnea (OSA)
Obstructive sleep apnea occurs when your airway becomes temporarily blocked, or obstructed, during sleep. It’s the most common type of sleep apnea.
These obstructions can happen when the muscles of the throat relax, or the tongue falls backward to block the throat.
2. Central Sleep Apnea (CSA)
Though less common than OSA, central sleep apnea can have equally severe consequences.
Central sleep apnea (CSA) occurs when a person’s brain has trouble sending signals to the muscles that control breathing while asleep. This miscommunication results in pauses in breathing, even though the airway remains clear.
3. Mixed Sleep Apnea Syndrome
Mixed sleep apnea syndrome, also called complex sleep apnea, is a blend of OSA and CSA.
People with mixed sleep apnea syndrome typically have the initial symptoms of obstructive sleep apnea. However, after receiving treatment for OSA, symptoms of central sleep apnea may become more noticeable.
Because of its overlapping symptoms, mixed sleep apnea syndrome can be the most challenging of the types to diagnose and treat.
10 Treatments for Sleep Apnea
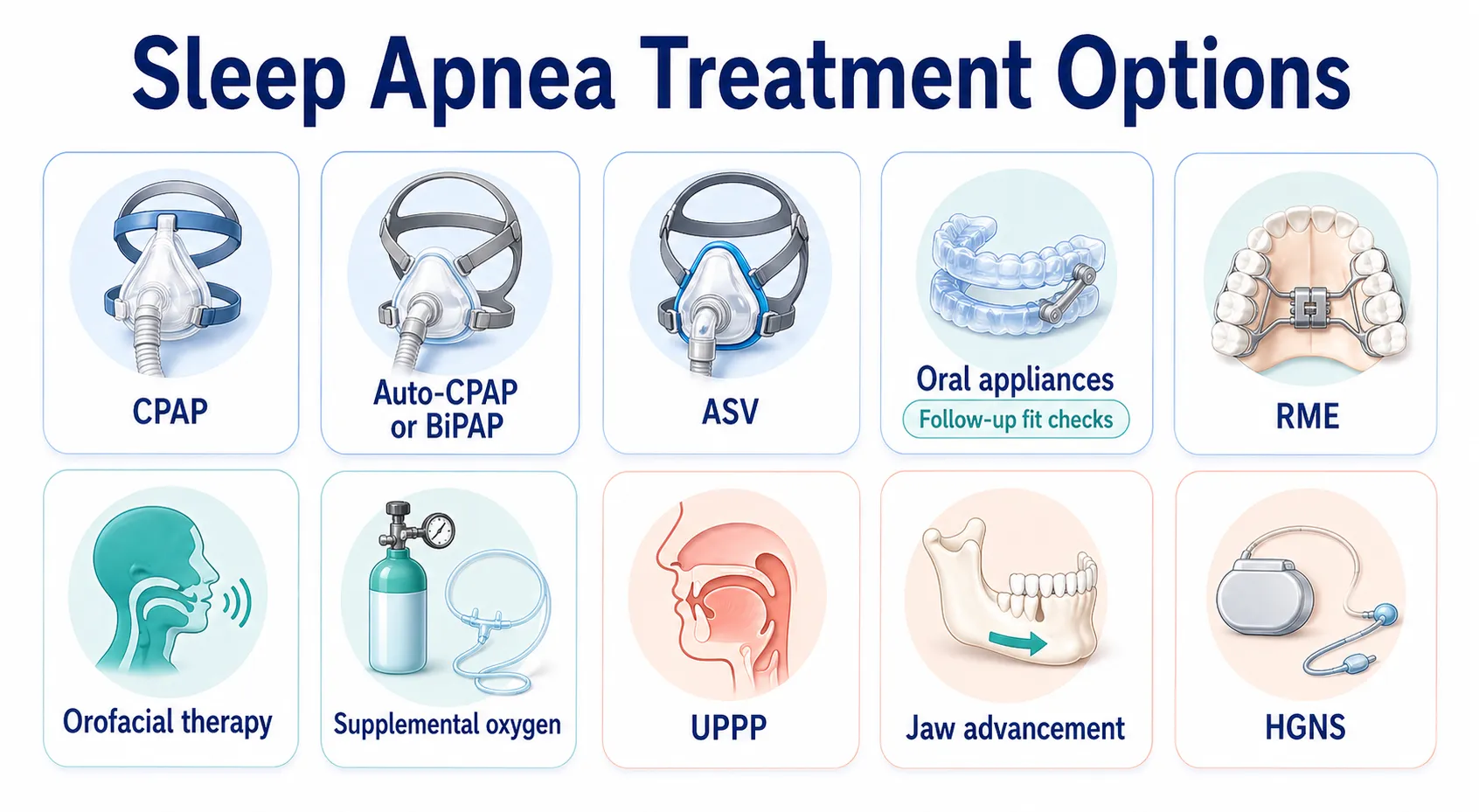 Treatment for sleep apnea depends on the type and severity of the condition. Common treatment options for sleep apnea include:
Treatment for sleep apnea depends on the type and severity of the condition. Common treatment options for sleep apnea include:
1. CPAP (Continuous Positive Airway Pressure) Machine
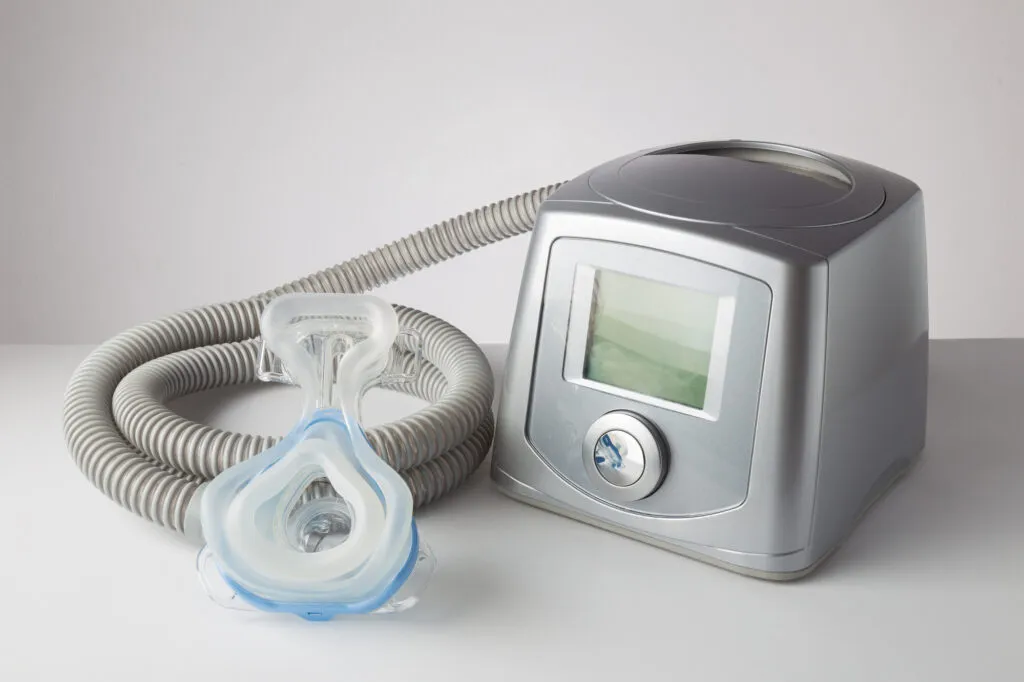
Using a CPAP (continuous positive airway pressure) machine is the first-line treatment for OSA. This treatment method involves wearing a specialized mask that fits over the nose and mouth while you sleep. The mask attaches to a machine that provides constant air pressure and keeps your airway open.
Many people with sleep apnea notice immediate improvements when they start using a CPAP machine. CPAP therapy can improve sleep quality and reduce or eliminate snoring.
However, they can also be uncomfortable. Some people may experience side effects such as a congested or runny nose, dry mouth, or nosebleeds. Approximately 50% of users become nonadherent over time or may refuse treatment.
2. Auto-CPAP or BiPAP Machine
For people who don’t like the standard CPAP machine, doctors may suggest using a different device, like an auto-CPAP machine. It’s a device that automatically adjusts the pressure as you sleep.
Alternatively, bilevel positive airway pressure (BiPAP) machines use two air pressure settings that provide more pressure on inhalation and less on exhalation.
3. Adaptive Servo-Ventilation (ASV)
This airflow device has a built-in computer that learns and stores your normal breathing pattern. While you sleep, the machine uses pressure to normalize your breathing and prevent breathing interruptions.
ASV might be more effective than other positive airway pressure devices in treating complex sleep apnea. However, ASV is not a suitable option for people with predominantly CSA and/or advanced heart failure.
4. Oral Appliances
Dentists can make custom-fit oral appliances to wear in your mouth while sleeping. Although CPAP machines are more effective, some people with sleep apnea find oral devices easier to use.
There are two primary types and some hybrid devices that have the features of both:
- Mandibular repositioning mouthpieces — These cover the upper and lower teeth, positioning the jaw forward so it cannot block the airway.
- Tongue retaining devices — These appliances hold the tongue forward to prevent it from blocking the airway.
You’ll need to follow up with your dentist regularly when using these devices to ensure the fit remains optimal.
The US Food and Drug Administration (FDA) has also recently approved an appliance that uses electrical stimulation on the tongue to prevent it from collapsing backward during sleep. It must be worn for 20 minutes daily for 6 weeks to see results.
5. Rapid Maxillary Expansion (RME)
RME is an effective orthodontic treatment for OSA, primarily for children. It’s a technique used to widen or expand the upper jaw if it’s too narrow. This enlarges the size of the nasal cavity and can substantially increase the airflow through the nose.
The procedure involves placing a fixed metal appliance on the upper teeth. The metal framework attaches to metal bands or a plastic splint cemented to the back teeth. In the parts that run across the palate, there’s an expansion screw that gradually widens the upper jaw.
RME is more effective in children since the bone is softer than in older people.
6. Orofacial Therapy
The aim of orofacial therapy is to increase and strengthen muscle tone, endurance, and movement. It consists of specific exercises for the facial muscles.
Training the muscles decreases the likelihood of airway collapse and improves sleep quality. Studies also found that orofacial therapy helps adherence to CPAP treatment.
7. Supplemental Oxygen
Using supplemental oxygen while you sleep may help if you have CSA. It can also help people who don’t prefer CPAP machines.
Supplemental oxygen can prevent hypoxemia or low oxygen levels. However, it doesn’t prevent obstructive events or improve daytime fatigue.
8. Uvulopalatopharyngoplasty (UPPP)
Uvulopalatopharyngoplasty (UPPP) is a widely performed OSA surgery. It’s an invasive procedure that involves removing soft tissue, including the tonsils, uvula, and part of the soft palate, to enlarge the airways.
Alternatively, doctors can use radiofrequency ablation to shrink the tissues at the rear of the mouth instead of removing them. This avoids the risk of major surgery and has similar benefits to UPPP.
Doctors may not always recommend UPPP to treat sleep apnea, as it doesn’t consistently help. It primarily benefits people with enlarged tonsils and a relatively normal palate.
9. Jaw Advancement Surgery
Maximum mandibular advancement surgery (MMA) is successful in 75 to 100% of cases. It involves moving the upper jaw (maxilla) and lower jaw (mandible) forward, enlarging the airways, and reducing airflow resistance.
Many experts now consider MMA the gold standard in surgical orthodontic treatment for OSA.
However, the surgery is not without risks. Some people experience temporary hearing changes and temporary or permanent facial numbness. The jaw can also return to its original position following surgery.
10. Hypoglossal Nerve Stimulation (HGNS)
In this procedure, a surgeon inserts a small electrical stimulation device into the chest wall. The device stimulates the hypoglossal nerve that controls muscles in the tongue. The stimulation rhythm synchronizes with a person’s breathing to relieve upper airway constriction.
This approach doesn’t require permanent alteration of the airway tissues. Research also shows that it’s effective and can decrease OSA symptom scores by 68% following 1 year of use.
The Importance of Treating Sleep Apnea
Treating any type of sleep apnea is essential to getting a full night’s sleep and avoiding severe health complications that may arise as a result. Left untreated, sleep apnea can lead to a host of issues, including:
- High blood pressure
- Heart disease
- Diabetes
- Increased risk of motor vehicle or workplace accidents
- Impaired cognitive function
- Lower job performance
- Exacerbated mood disorders
- Interference with attention and concentration
Early diagnosis and proactive treatment can alleviate symptoms and prevent serious complications from developing. Treating sleep apnea can improve your quality of life and may even extend your life expectancy.
If you have the symptoms of sleep apnea, contact your doctor immediately for evaluation and diagnosis.
How is Sleep Apnea Diagnosed?
A sleep specialist or sleep medicine doctor diagnoses sleep apnea by assessing your symptoms, family history, and medication use.
They may order tests to rule out other medical conditions and request a sleep study to help with their diagnosis.
Sleep Studies for Sleep Apnea Diagnosis
Sleep studies allow medical professionals to monitor your sleep and diagnose any chronic conditions, including sleep apnea.
A sleep study may take place during an overnight stay at a specialized sleep lab. Alternatively, people can use portable monitoring devices in their home.
The study involves placing sensors on the face, eyelids, chest, limbs, and fingers. These sensors measure brainwaves, heart and breathing rates, blood oxygen levels, and muscle movements.
The results may help diagnose sleeping disorders like obstructive sleep apnea or central sleep apnea.
How to Manage Sleep Apnea Naturally
Some people may be able to manage mild sleep apnea with lifestyle changes. Doctors may recommend these options for treating obstructive sleep apnea before trying other treatments.
Tips for managing your sleep apnea naturally include:
- Lose weight if recommended — Weight loss helps reduce fatty tissue that blocks the airways.
- Increase physical activity levels — Exercise boosts oxygen levels and improves sleep quality, improving energy levels.
- Reduce alcohol consumption — Alcohol reduces the tone of the upper airway breathing muscles and can lead to weight gain.
- Quit smoking — Research shows that smoking increases OSA symptoms and daytime sleepiness.
- Avoid strong pain relievers — Medications such as opioids and high-dose benzodiazepines can increase obstructive sleep apnea symptoms. These powerful drugs relax the breathing muscles and slow the breathing rate.
- Change sleeping positions — Some people breathe easier lying on their side. Beds that elevate the head may also help.
If you have severe sleep apnea, you should seek medical advice on further treatment.
Outlook and Prognosis of Sleep Apnea
Untreated sleep apnea stresses the heart, reduces life expectancy by several years, and can directly lead to death. However, effective treatment can control symptoms so that you can lead a normal life without long-term health effects.
Risks of Untreated Sleep Apnea
Without treatment, sleep apnea can cause serious health problems, including:
- High blood pressure
- Stroke
- Cardiac arrhythmias
- Enlargement of the heart muscle
- Congestive heart failure and/or heart attacks
- Diabetes
- Obesity
Many people with heart failure or an abnormal heart rate have sleep apnea, as sleep apnea can have serious effects on the body.
Additional serious effects include:
- Hypoxia or low oxygen levels
- Altered carbon dioxide levels
- Pressure changes in the chest that affect the heart
- Increased levels of inflammation
Anyone experiencing these symptoms should schedule an appointment with their doctor as quickly as possible.
Summary
Sleep apnea is a potentially serious sleep disorder in which breathing repeatedly stops and restarts. Obstructive sleep apnea (OSA) involves blockages of the airways, while central sleep apnea (CSA) involves problems with nerve signals.
Treatments such as continuous positive airway pressure (CPAP) machines, oral devices, and surgery effectively treat sleep apnea. Lifestyle changes such as weight loss, quitting smoking, and reducing alcohol consumption can also help.
Undiagnosed sleep apnea can cause serious health problems such as high blood pressure, stroke, and heart failure without treatment. Seeking medical help is essential if you’re experiencing sleep apnea symptoms so you can get back to having healthy sleep.
Sources
- Surani, S., and Taweesedt, P.“Obstructive Sleep Apnea: New Perspective.” Medicina (Kaunas), National Library of Medicine, 2023.
- “Causes and risk factors.” National Heart, Lung, and Blood Institute, National Institutes of Health, 2022.
- Singh, J. “Basics of Central Sleep Apnea.” American College of Cardiology, 2020.
- Punjabi, N.M. “The Epidemiology of Adult Sleep Apnea.” Proceedings of the American Thoracic Society, National Library of Medicine, 2008.
- Lin et al. “Gender Differences in Obstructive Sleep Apnea and Treatment Implications.” Sleep Medicine Review, National Library of Medicine, 2008.
- Krishnan et al. “Where There is Smoke…There is Sleep Apnea.” Chest, National Library of Medicine, 2014.
- “Sleep studies.” National Heart, Lung, and Blood Institute, National Institutes of Health, 2022.
- Chang et al. “Obstructive sleep apnea treatment in adults.” Kaohsiung Journal of Medical Sciences, Wiley Online Library, 2019.
- “FDA authorizes marketing of novel device to reduce snoring and mild obstructive sleep apnea in patients 18 years and older.” U.S. Food and Drug Administration, 2021.
- Gottlieb, G. “Supplemental oxygen for obstructive sleep apnea: Is there a role after all?” American Journal of Respiratory and Critical Care Medicine, ATS Journals, 2019.
- Maresch K. “Hypoglossal Nerve Stimulation: Effective Long term Therapy for Obstructive Sleep Apnea.” AANA Journal, National Library of Medicine, 2018.

UCLA-trained dentist practicing in public health. Focuses on whole-body approach to dental care.
Related Articles

Sleep Apnea Risk Assessment
Take our free online sleep apnea risk assessment to evaluate your risk factors and get personalized recommendations. Bas...

Mouthguards for Sleep Apnea
A custom-fitted mouthguard is one of many treatment options to help reduce sleep apnea symptoms. Learn about this and sl...

What to Expect During Wisdom Teeth Removal
Learn about the wisdom teeth removal procedure, aftercare, and costs. Discover why it's essential and get tips for a smo...
Dental Anesthesia
Dental anesthesia eliminates pain and reduces anxiety during procedures. Here are the three types, their benefits, and p...
