What is Gingivitis and How Do You Treat It?
Reader-supported. We may earn a commission from links on this page. Advertising disclosure.
In this article
Gingivitis, or mild gum disease, is the inflammation of the gum tissue. Prompt treatment can reverse its damage.
Otherwise, gingivitis can progress into periodontal disease, a severe form of gum disease that develops from long-term plaque and calculus buildup. It permanently damages the gums and bones and requires surgical treatment.
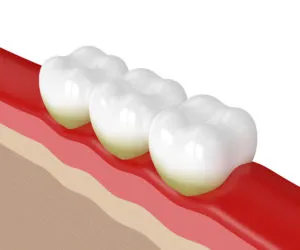
What Causes Gingivitis?
Gingivitis is due to plaque buildup, a sticky film of bacteria that naturally forms on your teeth. The bacteria in plaque cause inflammation and irritation in the gums, leading to gingivitis.
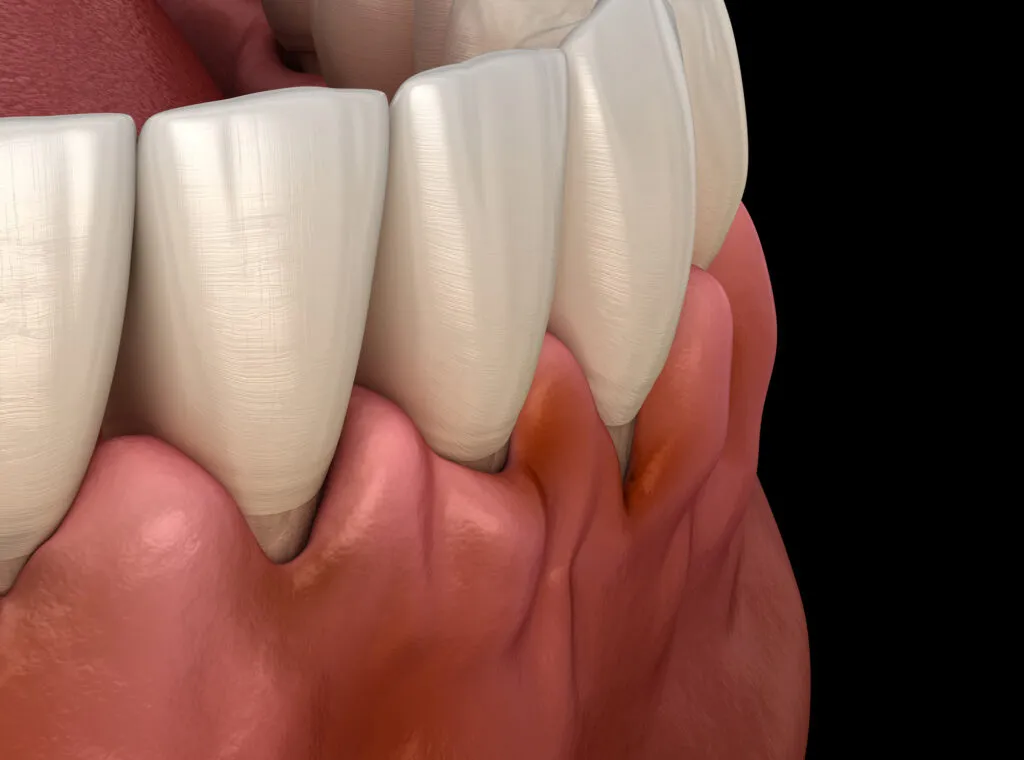
Multiple factors can put you at a higher risk of developing harmful plaque, including:
1. Smoking and Tobacco Use
Smoking is a major risk factor for developing gum disease. Tobacco users are 2 to 20 times more likely to develop periodontitis than their non-smoking counterparts. Using tobacco can also reduce your chances of successfully treating gingivitis or periodontal disease.
2. Poor Oral Hygiene
Taking care of your teeth at home is essential in preventing the plaque build-up that causes gingivitis. Dental professionals recommend brushing your teeth twice daily and flossing at least once daily.
3. Stress
Constant stress weakens the immune system and increases inflammation. While there’s insufficient evidence to show that stress can cause gum disease, it may be a risk indicator for it.
4. Hormonal Changes
People may be at a higher risk of developing gingivitis during hormonal events. These include pregnancy, menses, puberty, and menopause.
Roughly 60 to 75 percent of pregnant women develop gingivitis. Gum disease can also pass from mother to baby, which may lead to low birth weight or preterm birth.
5. Nutritional Deficiencies
Poor nutrition makes it difficult for the body to fight bacterial infection, putting you at a higher risk of developing gum disease. The buildup of dental plaque is also more likely, especially when consuming sugary or processed foods long-term.
6. Medications and Diseases
Cancer, diabetes, and HIV make it difficult to fight off infections, including gingivitis. Some prescription medications can also increase your risk of gum disease, including certain blood pressure medications, heart disease medications, anti-seizure medications, and immunosuppressants.
7. Dry Mouth
A dry mouth occurs when the salivary glands in the mouth don't produce enough saliva to keep the mouth wet. This condition is often a side effect of aging. Medications, smoking, radiation therapy, and mouth breathing can also lead to dry mouth and gum disease.
8. Other Causes
Other factors that can cause gingivitis include:
- Viral, fungal, and bacterial infections
- Impacted or infected teeth
- Allergic responses
- Genetic disorders
- Conditions that affect the mucus membranes
- Injury
- Foreign materials or dental restoration devices, such as dentures and dental pastes
Is Gingivitis Curable?
Yes, plaque-induced gingivitis is curable if you act quickly. Undergoing professional dental cleaning and maintaining good oral hygiene can reverse most cases of gingivitis.
Forty-six percent of all adults aged 30 and up show signs of gum disease. Many people don’t realize they have it until it progresses into periodontal disease since gingivitis typically doesn’t cause symptoms.
You must attend regular dental check-ups to monitor for gingivitis. The earlier your dentist catches it, the less likely you’ll develop periodontal disease or lose teeth.
What are the Stages of Gum Disease?
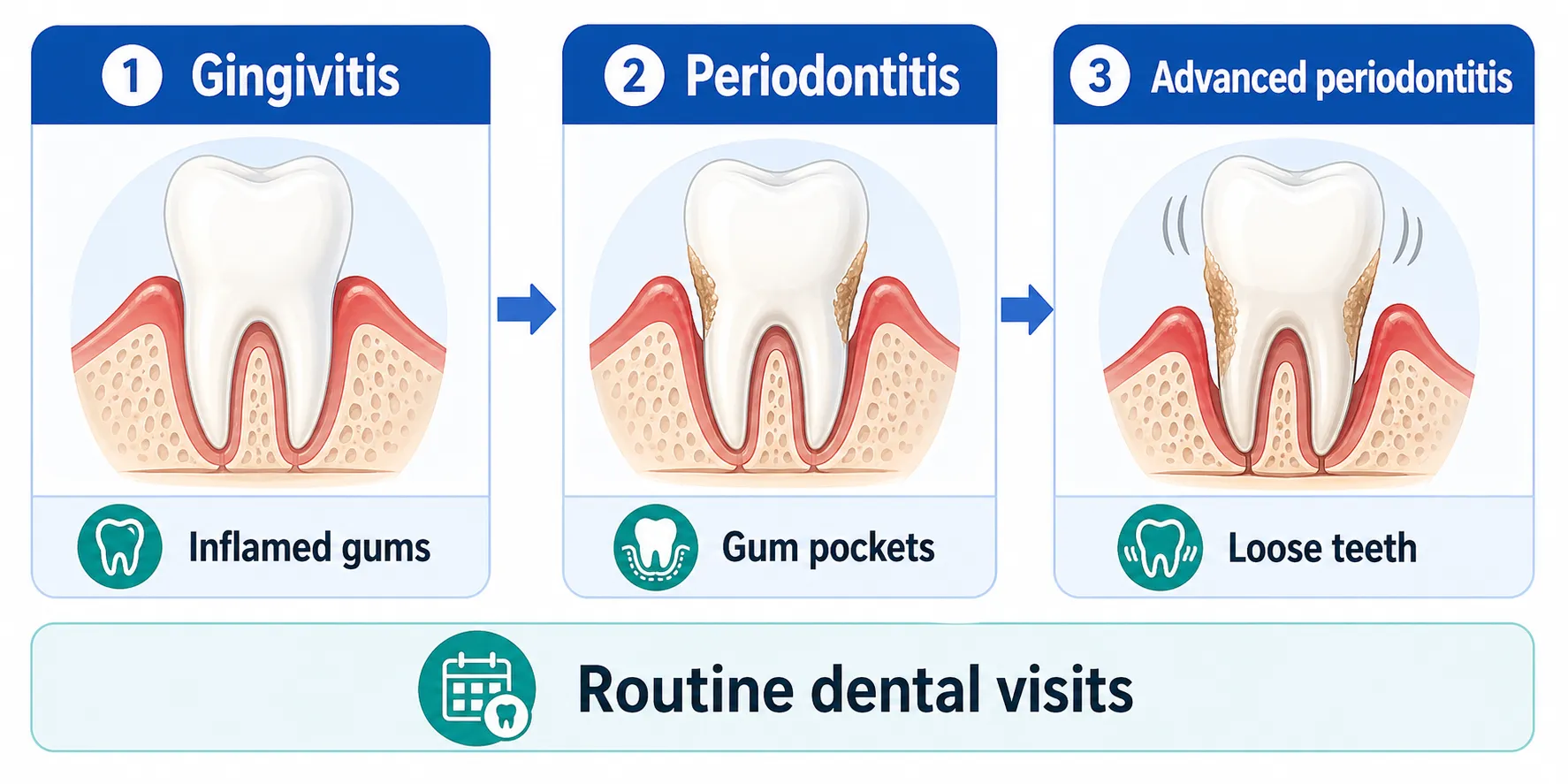
There are three stages of gum disease:
1. Gingivitis
Gingivitis is the early stage of gum disease. It occurs when you accumulate a film of plaque in your mouth.
During this first stage, you may notice inflamed, red, or swollen gums. However, sometimes no symptoms are present.
2. Periodontitis
Untreated gingivitis progresses to the intermediate stage of gum disease, periodontitis. It involves the following:
- Plaque continues to build up, harden, and collect below the gum line
- Plaque releases toxins that trigger increased gum inflammation
- Gums start to pull away from the teeth, forming periodontal pockets
- Plaque and tartar migrate into these pockets, which are difficult to clean
- There will be a separation between the gums and the teeth
- You may lose teeth at this stage
Unlike gingivitis, periodontitis is irreversible. However, you can slow it down with treatments like scaling and root planing.
3. Advanced Periodontitis
Without treatment, periodontitis will become more severe. The symptoms of advanced periodontitis include:
- Extreme separation between the gums and teeth
- Very loose teeth that make chewing difficult
- Bleeding, swollen gums
Gum disease may require tooth extractions or surgery when it advances to this stage.
What are the Symptoms of Gingivitis?
Gingivitis doesn’t always cause noticeable symptoms, so you may not detect it for some time without routine dental visits. However, some people may notice warning signs that point to mild gum disease, including:
- Dark red or purple gums
- Puffy or tender gums
- Sensitive teeth and gums
- Swelling in the gums
- Gums bleeding when brushing or flossing
Periodontitis Symptoms
When gingivitis progresses into periodontitis, you’ll notice these more obvious symptoms:
- Receding gums or a gummy smile
- Loose teeth
- Separation of the gums from the teeth
- Chronic bad breath throughout the day
How is Gingivitis Diagnosed?
To diagnose someone with gingivitis, a dentist will:
- Ask questions about symptoms, medical history, risk factors for gingivitis, and family history of gum disease
- Examine the teeth and gums for signs of bleeding, inflammation, loose teeth, or receding gums
- Use a probe to measure pockets around the teeth (in healthy gums, these pockets aren’t more than 1 to 3 millimeters)
- Take X-rays to assess bone loss or damage
Your dentist may also recommend a medical evaluation to check for underlying health conditions. They may refer you to a periodontist (gum disease specialist) if you have advanced gum disease.
How Do You Treat Gingivitis?
The primary treatments for gingivitis include:
1. Professional Teeth Cleanings
The only way to completely reverse gingivitis is to remove plaque and tartar. A dental hygienist or dentist will use specialized instruments to clean your teeth and gums. These materials remove plaque and tartar that a regular toothbrush cannot.
2. Scaling and Root Planing
Scaling removes tartar buildup and plaque from the teeth and below the gum line. Dental professionals use hand, laser, or ultrasonic devices during scaling to ensure they can clean teeth thoroughly.
After scaling, they may also perform root planing. Root planing involves smoothening the tooth’s root surfaces to prevent bacteria from sticking and help the gums adhere back to the teeth.
Scaling and root planing may require a local anesthetic. It could also take more than a few dental visits to complete.
3. Ongoing Oral Hygiene Practices
After your professional dental treatment, you’ll need to practice vigilant oral care. It includes brushing your teeth twice daily, flossing at least once per day, and seeing your dentist for cleanings every six months.
4. Regular Dental Checkups
Make sure to schedule regular checkups and cleanings every 6 to 12 months. People with risk factors for gingivitis or a history of it should get cleanings and checkups every two weeks to 3 months.
Regular dental checkups ensure your teeth and gums remain in their best condition. Your dentist or dental hygienist can also catch and treat gingivitis before it worsens.
5. Fixing Teeth or Poorly Fitted Dental Devices
A dentist or periodontist can fix braces and dentures that don’t fit properly. They can also fix teeth that are misshapen or crooked, which can cause them to harbor bacteria.
When your dental devices fit better, it becomes more manageable to maintain good oral hygiene. Having a solid oral hygiene routine can make gingivitis treatment easier or prevent the need for it altogether.
6. Invasive Treatments
No further treatment is necessary if your gum disease doesn’t progress beyond the early stages. However, your dentist will recommend more invasive treatment if you have periodontitis.
Common treatment options for periodontal disease include:
How to Treat Gingivitis At Home
If you have a mild form of gingivitis, you can treat the condition at home by:
- Brushing your teeth twice a day, at least two minutes at a time
- Flossing once daily
- Rinsing with mouthwash
- Massaging your gums to increase blood flow to the gum tissue
If you suspect you have gingivitis, consult a dentist on the best treatment option.
How to Prevent Gingivitis
All gum disease is preventable if you practice diligent oral hygiene. You can prevent gingivitis and its more advanced stages by following these simple steps:
- Brush your teeth twice daily
- Floss at least once daily
- Use mouth rinse
- Replace your toothbrush every few months
- Consider using an electric toothbrush
- Visit your dentist for a professional cleaning every six months
- Don’t smoke or use tobacco
- Manage stress and chronic conditions
- Address dry mouth
Summary
Gingivitis is the earliest stage of gum disease, involving mild inflammation of the gums. Plaque buildup causes it, the natural film of bacteria that forms on teeth.
The main symptoms of gingivitis are red, swollen, and bleeding gums, though many people will notice no signs at all. Periodontitis is irreversible and involves bone loss, separation of the teeth from the gums, and loose teeth.
Gingivitis is easy to treat and prevent. Talk to a dental professional immediately if your gums are red, swollen, sensitive, or bleed easily.
What Is Gingivitis And How Do You Treat It?
NewMouth PodcastSources
- “Gum Disease Facts.” Centers for Disease Control and Prevention, 2024.
- Naderi et al. “The Impact of Smoking on Gingiva: a Histopathological Study.” Iranian Journal of Pathology, 2015.
- Goyal et al. “Stress and periodontal disease: the link and logic!!” Indian Psychiatry Journal, 2013.
- “Talking to Pregnant Women about Oral Health.” Centers for Disease Control and Prevention, 2024.
- “Gingivitis and periodontitis: Overview.” InformedHealth.org, 2020.
- Wada-Takahashi et al. “Effect of physical stimulation (gingival massage) on age-related changes in gingival microcirculation.” PLoS One, 2020.
- Goes et al. “Clinical efficacy of a 1% Matricaria chamomile L. mouthwash and 0.12% chlorhexidine for gingivitis control in patients undergoing orthodontic treatment with fixed appliances.” Journal of Oral Science, 2016.

UCLA-trained dentist practicing in public health. Focuses on whole-body approach to dental care.
Related Articles
Cost of Dental Check Ups
How Much Does a Dental Check-Up Cost? A dental checkup can cost between $0 to $500+ depending on several factors, includ...

What to Expect During Dental Cleanings
What happens during a dental cleaning? Learn more about each process step, from the first oral examination to the final...

What to Expect During Wisdom Teeth Removal
Learn about the wisdom teeth removal procedure, aftercare, and costs. Discover why it's essential and get tips for a smo...

How to Become a Dental Hygienist
Wondering how to become a dental hygienist? This guide will walk you through everything from what is a dental hygienist...
