Endodontists: Root Canal & Dental Pulp Experts
Reader-supported. We may earn a commission from links on this page. Advertising disclosure.
In this article
What is an Endodontist?
Endodontists are dental specialists who treat tooth pain, disease, and infection. They are experts in treating dental pulp issues.
They are often called “root canal specialists” because root canal therapy is the most common treatment they provide.
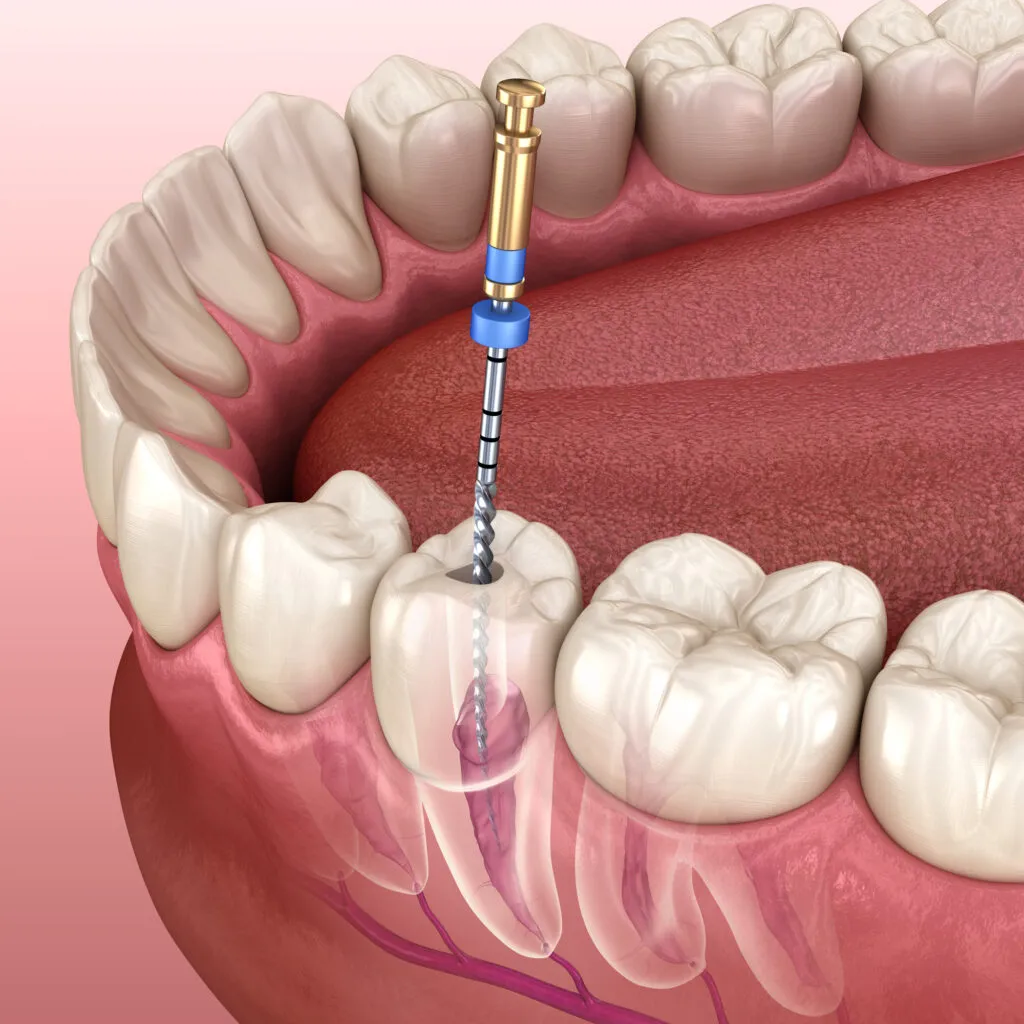
Endodontists have an in-depth understanding of the anatomy of tooth roots, root morphology, dental pulp, and the internal anatomy of teeth. In addition to dental school, these specialists undergo two to three years of advanced education and further training in endodontic care.
What’s the Difference Between a Dentist and an Endodontist?
The primary difference between a dentist and an endodontist is their level of expertise. Dentists typically treat a wide range of general oral health issues but might not be advanced specialists.
Endodontists are dentists who have completed extra training and specialize in issues relating to dental pulp. An endodontist is a dentist, while a dentist is not always an endodontist.
What is Dental Pulp?
Dental pulp is a living tissue in teeth that contains sensory nerves and blood vessels. It’s essential for oral health.
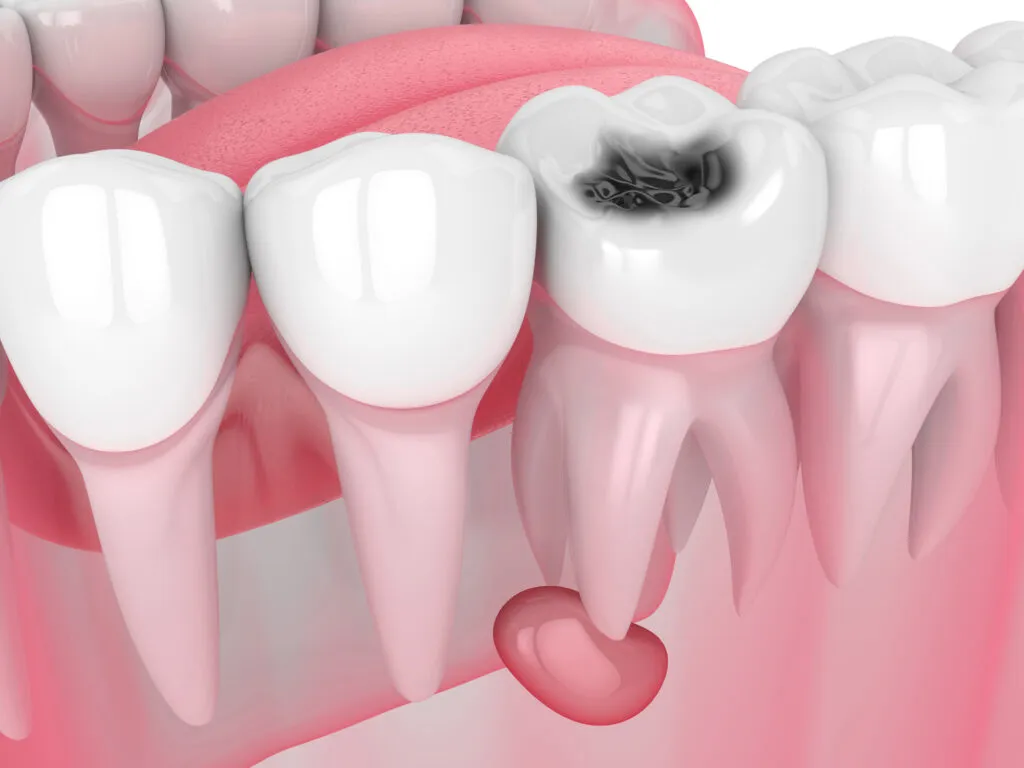
Because pulp is a living tissue, it’s easy to irritate it. Pulp irritation can lead to inflammation and tissue damage in more serious cases.
If tooth decay spreads, it can infringe on the pulp, potentially leading to an infection or severe disease. Even small cavities and trauma-related dental issues can release toxins into the dental pulp.
What Procedures Do Endodontists Perform?
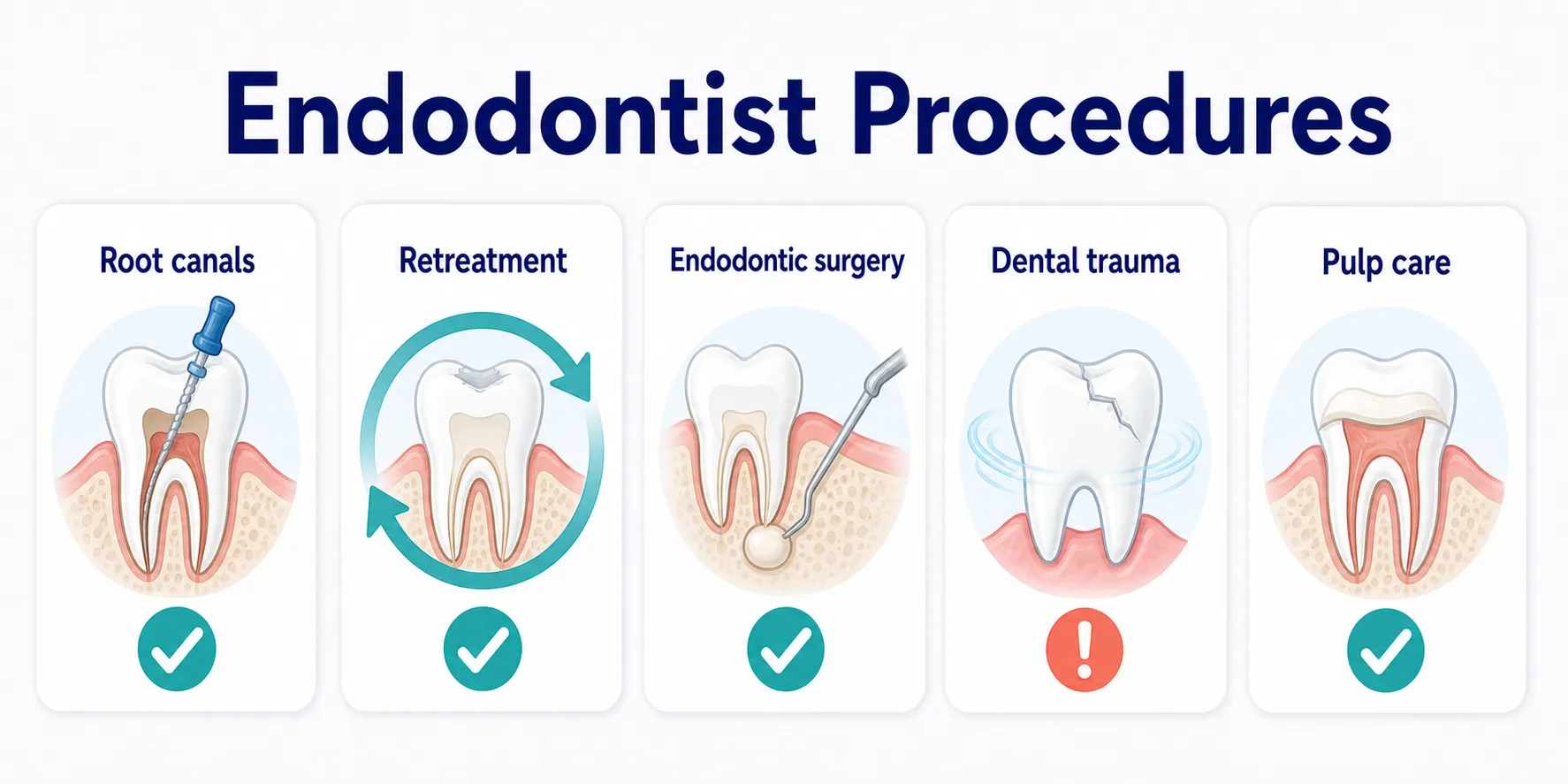
Endodontists spend most of their time diagnosing and treating root canals.
However, they also specialize in endodontic retreatment, endodontic surgery, and trauma-related dental injuries:
Root Canal Treatment
Endodontists specialize in root canal treatment, also called endodontic treatment or root canal therapy. A root canal is necessary when the pulp within a tooth is severely infected or damaged.Root canal treatment involves removing the infected pulp within a tooth. It saves the tooth and eliminates the need for extraction.
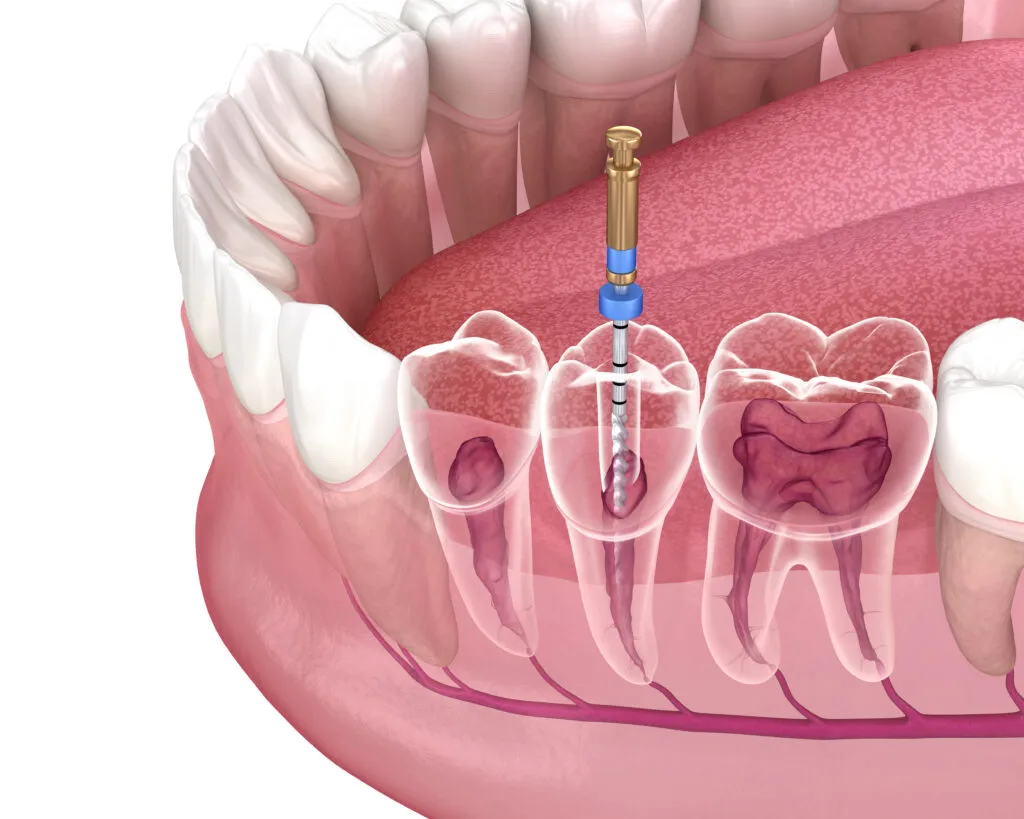
On average, endodontists complete 25 root canals per week, while general dentists perform about two per week.
Dental Extraction and Implants
When a tooth dies or is determined unsavable, extraction is typically necessary. An endodontist is skilled at complex tooth extractions.
After extracting the infected tooth, the endodontist will place a dental implant where the permanent tooth used to be. A dental implant (artificial tooth root) mirrors the shape of a screw. It is surgically inserted into the jawbone and bonds with the natural bone.
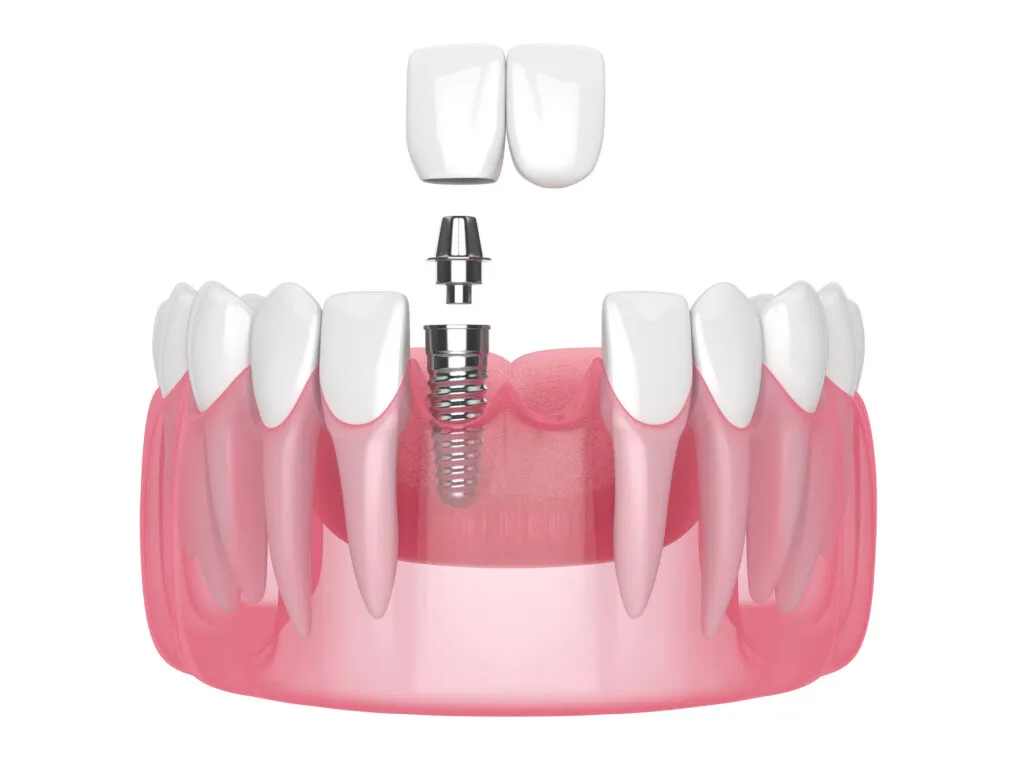
Then, a dental crown goes on top of the implant and becomes the only visible part of the artificial tooth.
Tooth extraction and dental implant treatment are recommended when a root canal isn’t enough to preserve a tooth. Common indicators for implant placement include:
- Tooth decay — If a tooth with extreme decay is left untreated, it commonly results in tooth loss.
- Periodontal disease — A severe gum disease that causes inflammation, tooth infections, and eventually bone loss.
- Old age and medications — Tooth loss is more common after age 55. Older people who take medications for heart disease, high cholesterol, or high blood pressure are even more susceptible.
- Trauma or injury — Damaged teeth caused by an injury, car accident, or fall can lead to complete tooth loss, partial tooth loss, or small chips.
Endodontic Retreatment
Root canals are usually successful and can last a lifetime with proper care. However, restorations can occasionally fail, which results in the need for “retreatment.”
Endodontic retreatment is necessary if the treated tooth heals improperly, becomes painful, or is infected months or years after treatment. The procedure helps relieve dental pain and discomfort and promotes healing.
A tooth may not heal after root canal therapy for a few reasons, including:
- The root canals were not treated properly during the first procedure
- Complicated tooth canal anatomy (such as narrow or curved root canals) was not detected during the first procedure
- Dental crown placement was postponed following the root canal procedure
- Salivary contamination was not prevented during any phase of treatment
Endodontic Surgery
Nonsurgical root canal therapies may not be enough to save a patient’s tooth. In these cases, an endodontist will perform microsurgery, also called endodontic surgery.
Endodontic surgery involves finding the fractures or root canals an X-ray didn’t detect. The procedure removes calcium buildup in a root canal, treats damaged root surfaces, and stabilizes the surrounding bone near the tooth.
Microsurgery might be necessary if root canal treatment isn’t enough. The tooth won’t need to be extracted during surgery.
4 Types of Dental Pulp Diseases
There are four common dental pulp conditions (pulpitis), including:
1. Reversible Pulpitis
Reversible pulpitis is caused by tooth decay and exposed dentin (the layer under tooth enamel). It’s typically minor and doesn’t require a tooth extraction or root canal.
Treatment involves removing the cavity and covering the tooth with a filling to protect it from infection. Reversible pulpitis commonly develops after dental procedures and often resolves without treatment.
2. Symptomatic Irreversible Pulpitis
Symptomatic irreversible pulpitis develops when cavities get very close to or inside the pulp chamber (interior of a tooth). Traumatic dental injuries can also cause irreversible pulpitis if the trauma exposes the pulp.
Teeth with this condition are hypersensitive to cold stimuli and develop lingering pain. Root canal treatment is usually recommended.
3. Asymptomatic Irreversible Pulpitis
Asymptomatic irreversible pulpitis is similar to symptomatic irreversible pulpitis (minus the symptoms). You might notice mild or no discomfort, though the affected tooth will be sensitive to cold.
Despite the lack of symptoms, this form of pulpitis also requires root canal treatment.
4. Pulpal Necrosis (Dead Tooth)
Pulpal necrosis is when the tissue inside a tooth dies. When this happens, debris, inflammatory cells, and bacteria replace the healthy dental pulp within the tooth.
A tooth with pulpal necrosis will not respond to cold and may result in bone loss. Treatment involves root canal therapy or removal of the affected tooth.
When Do I Need a Root Canal?
The need for root canal therapy or a similar endodontic treatment depends on the type and severity of the pulpitis. You’ll need a root canal if you have a severe infection in a tooth or irreversible damage to the pulp.
An endodontist will examine your mouth using radiographic images and pulp testing. They may use thermal and electrical testing to determine the severity of the pulpitis.
Various factors contribute to the need for a root canal, including:
- Severe tooth decay — Untreated cavities result in severe tooth decay over time. This can provoke a response from the dental pulp.
- Gum inflammation — When the gums become inflamed, it is more likely that the bacteria will travel to a tooth’s root. Bacteria can severely damage the pulp over time.
- Tooth chips and cracks — Habitual tooth grinding and clenching (bruxism) can also lead to pulpitis as the enamel thins.
- Injury or trauma — If a permanent tooth is dislodged due to a traumatic injury, root canals may be necessary to protect it from further damage or infection.
- Large cavity fillings — Teeth with large cavities and fillings are more prone to dental pulp infections.
Summary
Endodontists are dentists with extra training and expertise in oral health issues related to dental pulp. They have an in-depth understanding of tooth anatomy and complex dental problems.
The most common procedure an endodontist performs is a root canal treatment. Root canal therapy removes inflamed or infected tissue, or dental pulp, inside a tooth. Endodontists can also perform microsurgery, tooth extractions, and dental implant placements.
You can see a general dentist for a root canal, though your dentist might refer you to an endodontist for expert treatment.
Sources
- “Endodontic Retreatment.” American Association of Endodontists, 2023.
- Hollins, C. “Basic Guide to Dental Procedures.” John Wiley & Sons, Inc., Google Books, 2015.
- Syrbu, J. “The Complete Pre-Dental Guide to Modern Dentistry.” Google Books, 2013.
- Goldberg, M., et al. “Dentin: Structure, Composition and Mineralization.” Frontiers in Bioscience – Elite, National Library of Medicine, 2011.
- Mathew, S., et al. “Diagnosis of cracked tooth syndrome.” Journal of Pharmacy and BioAllied Sciences, National Library of Medicine, 2012.
- Chen, E., et al. “Dental Pulp Testing: A Review.” International Journal of Dentistry, National Library of Medicine, 2009.

Experienced general dentist and adjunct professor. Advocates for preventive dentistry and dental education.
Related Articles
Gum Flap Surgery: Treatment Steps, Aftercare & Risks
What is gum flap surgery? This article discusses the surgery steps, cost, and aftercare. You'll also learn its possible...
Dental Specialties: Compare Your Treatment Options
Having the right dentist can make all the difference. Learn about 6 different dental specialties and how they differ fro...
LANAP Laser Gum Surgery
LANAP Laser Gum Surgery is a new and innovative gum disease treatment. This article discusses the benefits and costs of...
How Does Sedation Dentistry Eliminate Dental Anxiety?
Dental anxiety is a problem for many people, but sedation dentistry can help. Learn about its benefits, side effects, th...
