Trench Mouth Symptoms, Causes & Treatment
Reader-supported. We may earn a commission from links on this page. Advertising disclosure.
In this article
If you’re experiencing sudden gum pain, foul breath, and unexpected bleeding, you might have what’s commonly called trench mouth. Medically, it’s known as acute necrotizing ulcerative gingivitis (ANUG).
Despite its alarming name and painful symptoms, ANUG is highly treatable when addressed promptly. Let’s break down exactly what’s happening and how you can heal quickly.
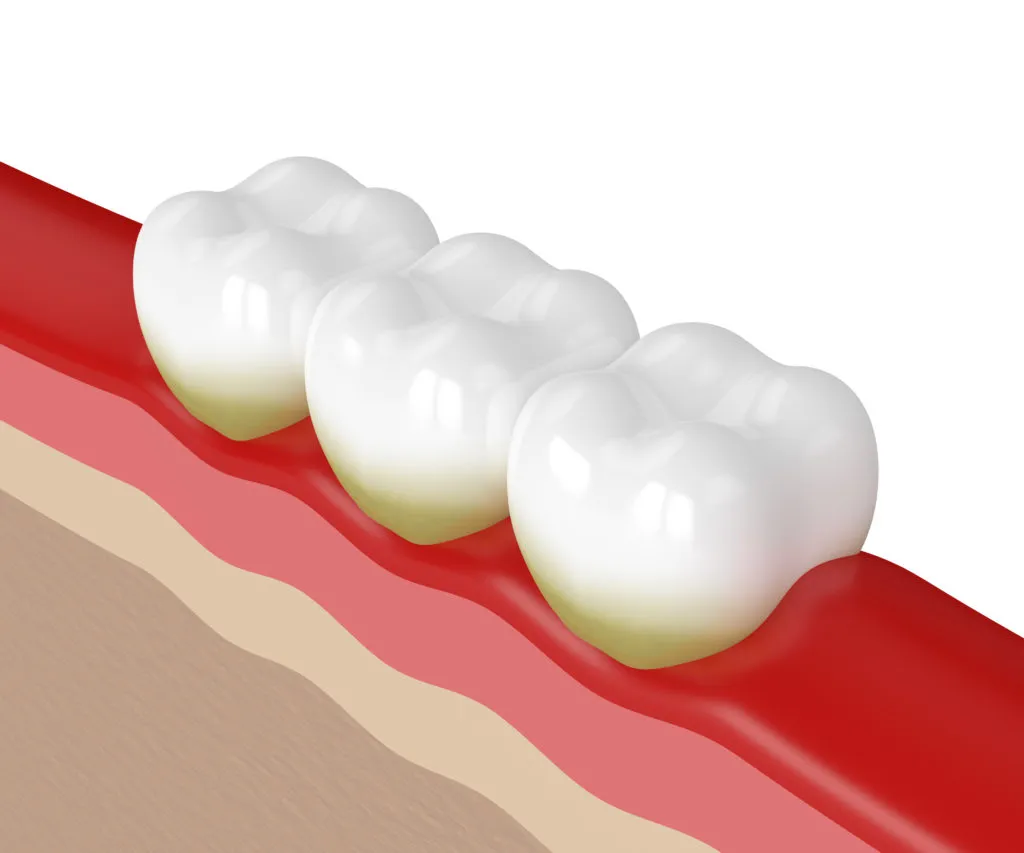
What is Trench Mouth?
Trench mouth (acute necrotizing ulcerative gingivitis) is a severe form of gingivitis. It’s also sometimes referred to as Vincent’s disease or Vincent’s angina.
It earned the nickname “trench mouth” during World War I, when poor hygiene and extreme stress led to widespread outbreaks among soldiers.
However, this condition isn’t just a historical relic. It’s still relevant in 2026, particularly among young adults juggling stress, sleep deprivation, and smoking habits.
How Common is Trench Mouth?
Today, trench mouth is a rare disease. It’s more likely to be found in areas with poor nutrition and sanitation. People who are immunocompromised in developed countries can also develop trench mouth.
Untreated trench mouth can spread to other parts of the mouth and face, leading to severe disfigurement or even death. However, this is rare, and trench mouth can be treated well before these complications develop.
Here are quick facts to clear up some common fears about the condition:
- Not contagious — You won’t spread trench mouth casually.
- Highly treatable — Fast action usually means rapid recovery.
- Preventable — Good dental habits and stress management keep it away.
Trench Mouth Symptoms to Watch For
Acute necrotizing ulcerative gingivitis (ANUG) typically shows clear signs. Catching these symptoms early can mean faster relief and simpler treatment.
These early symptoms include:
- Grayish film — A noticeable layer of dead gum tissue forming between teeth.
- Cratered ulcers — Painful, open sores that resemble small craters.
- Metallic taste & odor — Persistent bad breath or a strange, metallic flavor in your mouth.
- Spontaneous bleeding — Gums bleeding easily, even with gentle brushing or eating.
- Fever or swollen lymph nodes — Potential signs the infection is spreading beyond your gums.
When Should You Go to the Emergency Room?
To tell if your symptoms need urgent care or a regular dentist appointment, refer to this simple guide:
- Same-day dental visit — If your main symptoms are gum pain, odor, and slight bleeding.
- Emergency room — Go immediately if you have severe facial swelling, high fever, difficulty swallowing or breathing, or feel dehydrated due to pain.
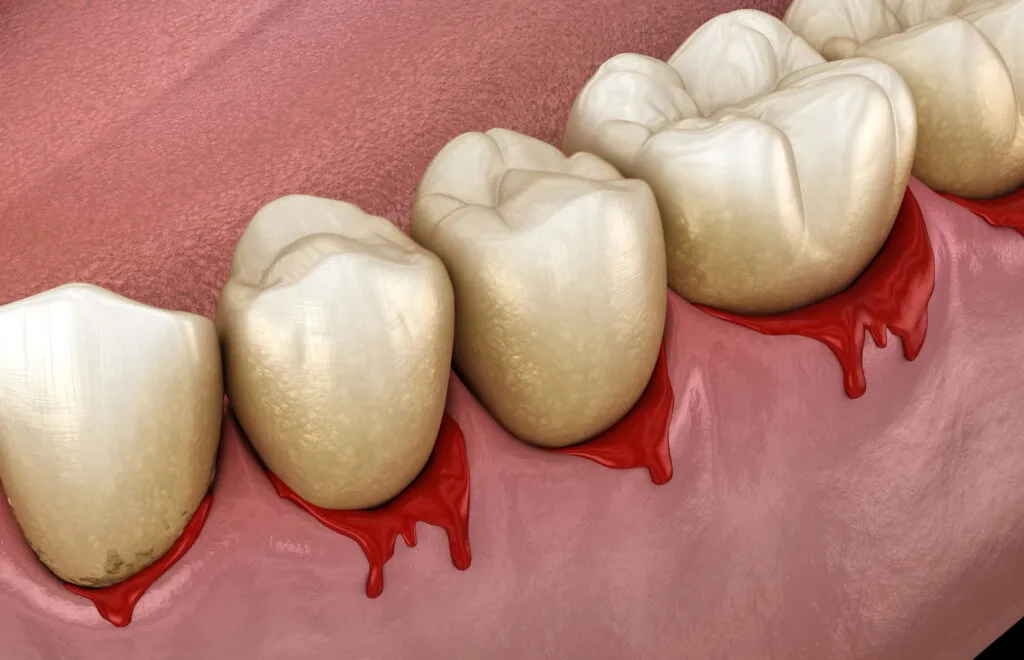
What Causes Trench Mouth?
Trench mouth develops from a combination of harmful bacteria (such as Fusobacterium and Prevotella) and lowered immune defenses. Certain lifestyle factors significantly raise your risk, especially if you’re already run down or stressed out.
Common triggers include:
- Smoking — Reduces blood flow to your gums, impairing healing.
- Stress and poor sleep — Elevated cortisol levels weaken your immune response.
- Poor nutrition — Lack of key vitamins like vitamin C and folate leaves gum tissue vulnerable.
- Poor oral hygiene — Skipping brushing or flossing allows harmful bacteria to thrive.
Despite the historical association, trench mouth doesn’t just affect soldiers or people in extreme situations—it can strike anyone under stress or neglecting their dental care.
Trench Mouth Treatment Options
Treating trench mouth involves professional dental care paired with straightforward home treatments to speed up healing and soothe symptoms.
Professional steps your dentist will take include:
- Gentle debridement — Your dentist will use local anesthetic and special tools to remove necrotic tissue and bacteria from your gums.
- Prescription rinses — You may receive a chlorhexidine gluconate or diluted hydrogen peroxide rinse to control bacterial growth.
- Selective antibiotics — If the infection is severe or spreading, your dentist might prescribe a short course of antibiotics, typically metronidazole.
When at home, you can do the following to ease your symptoms:
- Soft brushing twice daily — Gentle brushing removes plaque without causing further irritation.
- Warm saltwater rinses — Rinse your mouth gently several times daily to soothe inflammation.
- Pain relief — Use over-the-counter pain relievers (like ibuprofen) to manage discomfort.
Home remedies are meant to supplement treatment prescribed by your dentist. When you follow your dentist’s instructions, most patients experience significant pain relief within 24 to 48 hours and complete healing within one to two weeks.
How Much Does Trench Mouth Treatment Cost?
Managing trench mouth is generally affordable, with treatments in the U.S. typically ranging from $150 to $500. These are often covered partially by insurance (usually under coding D4355).
Many dental schools and community clinics offer low-cost care options if affordability is an issue.
Consider seeing a periodontist or medical specialist if:
- You have repeated episodes of trench mouth.
- You are immunocompromised or dealing with other chronic health conditions.
- Symptoms persist or worsen despite initial treatment.
How to Prevent Trench Mouth
Once treated, trench mouth rarely returns if you consistently practice good oral hygiene and manage stress.
Here are some tips to follow to prevent trench mouth from occurring again or in the first place:
- Quit smoking — Utilize resources like nicotine replacement therapy or support groups.
- Control daily stress – Techniques like mindfulness, meditation, or ensuring adequate sleep can significantly reduce recurrence risk.
- Daily plaque removal — An electric toothbrush, floss, and interdental brushes help maintain optimal oral health between professional cleanings.
- Nutrition boost — Ensure your diet includes foods rich in vitamin C, folate, and iron—essential nutrients for strong gum tissue.
The sooner you act, the faster you’ll heal. If your gums hurt, bleed easily, or appear gray and ulcerated, schedule a same-day dental appointment immediately.
Maintain diligent oral hygiene and stress management going forward. Taking these simple steps ensures rapid recovery, keeps your mouth healthy, and puts trench mouth behind you permanently.
Sources
- Necrotising periodontal disease (acute necrotising ulcerative gingivitis) – Adult summary guidance. Health Service Executive, Health Service Executive, 2023.
- Acharya et al. Necrotising gingivitis and the dental team. BDJ Team, 2024.
- Gasner, N.S. and Schure, R.S. Necrotizing Periodontal Diseases. StatPearls. National Center for Biotechnology Information, 2023.
- Management of periodontal disease in people with HIV. HIV Clinical Guidelines, New York State Department of Health, AIDS Institute, 2020.
- Ciribè et al. Management of necrotizing gingivitis in paediatric patients: A scoping review and two case reports. Children, 2024.
- A step-by-step guide to develop national action plans for noma prevention and control in priority countries. World Health Organization, World Health Organization Regional Office for Africa, 2022.
- Sobolewska, E., and Wójcik-Chwastek, V. Impact of nutrition on the condition of the oral mucosa and periodontium: A narrative review. Dental and Medical Problems, 2023.

UCLA-trained dentist practicing in public health. Focuses on whole-body approach to dental care.
Related Articles

What is Gum Disease: How To Prevent and Treat It
Gum disease is a serious infection that can cause tooth loss and other health problems. Find out more about the causes,...

Dental Calculus Causes & Treatment
This article will discuss dental calculus buildup, its effects on teeth and gums, how to prevent its development, and ho...

What is Eagle Syndrome?
What is Eagle Syndrome? Eagle syndrome (or styloid syndrome) is a rare condition that can cause sharp jaw and neck pain,...

Bleeding Gums: Causes, Remedies & Treatment
Bleeding gums can be a sign of gum disease. They can also be caused by other things like brushing too hard or hormonal c...
