TMJ Surgery: Types, Costs, What to Expect, Procedure, and Recovery
Reader-supported. We may earn a commission from links on this page. Advertising disclosure.
In this article
Key Takeaways
- TMJ surgery is a last-resort treatment for severe temporomandibular disorder (TMD). Doctors will only recommend surgery if all other treatments have failed.
- There are five main types of TMJ surgery which range in their invasiveness.
- Recovery can take days, weeks, or months and frequently involves a soft food diet and physical therapy.
- The cost of TMJ surgery varies widely based on your provider, insurance coverage, and the type of procedure. It can cost anywhere from $300 to $50,000.
- TMJ surgery is expensive, irreversible, and typically only recommended when nothing else works.
What is Temporomandibular Joint Disorder (TMD)? Symptoms and Causes
The temporomandibular joint (TMJ) refers to either one of the two joints connecting your lower jaw (mandible) to your skull.
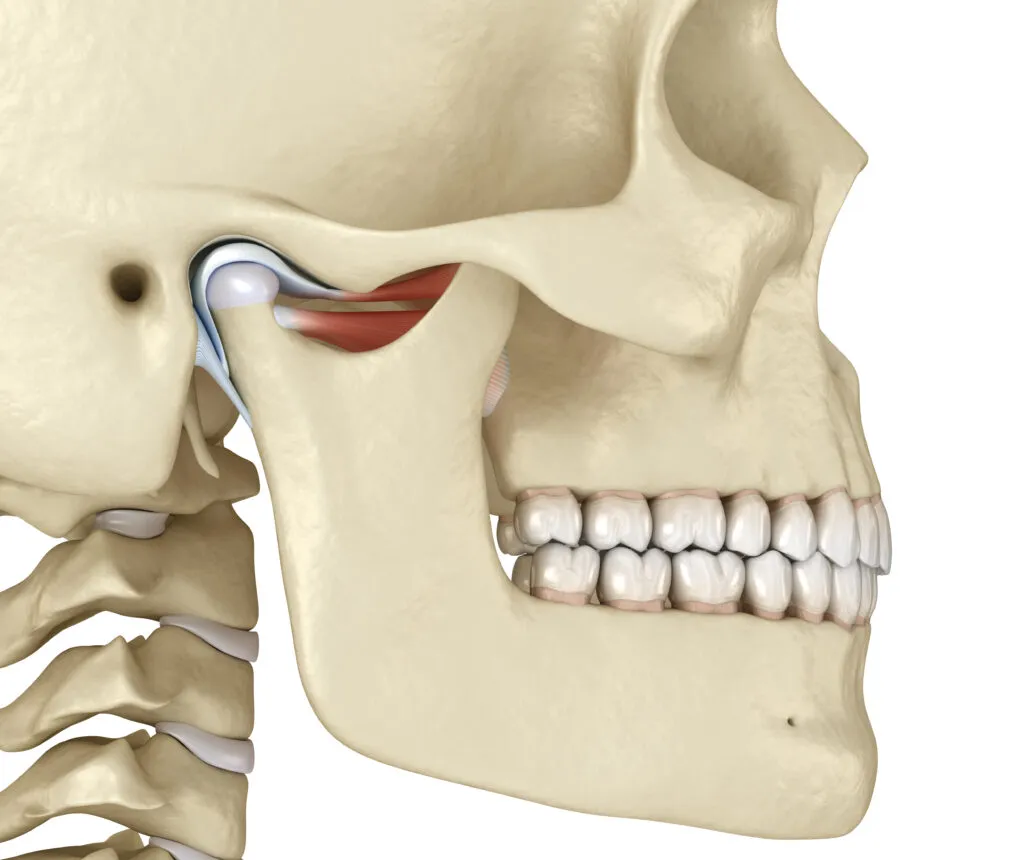
Image of a healthy temporomandibular joint.
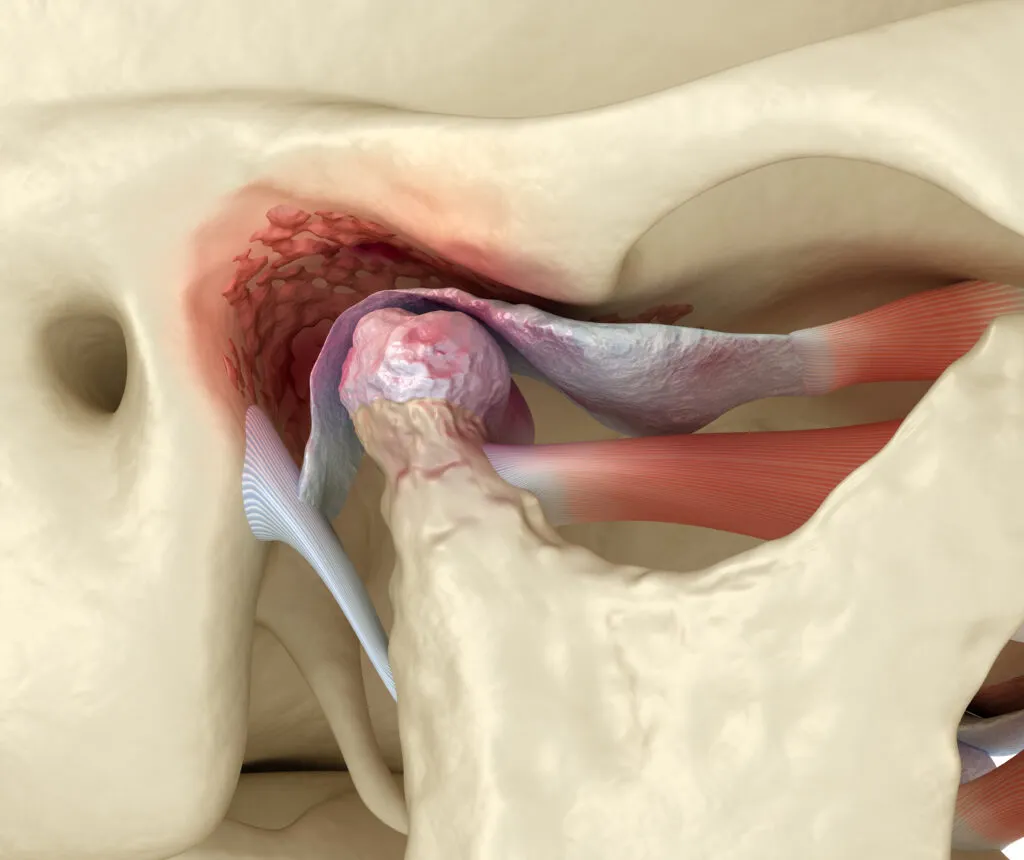
Image of a damaged temporomandibular joint.
TMJ disorders (TMJDs or TMDs) are problems with one or both of these joints. TMD symptoms include:
- Pain at the jaw joint, including pain that spreads to other areas
- Painful popping or clicking of the jaw
- Jaw stiffness
- Jaw locking or limited ability to open and close the jaw
- Buzzing or ringing in the ears
The exact causes of most TMDs aren’t well understood, but experts have found associations with certain genetic and hormonal factors. Potential risk factors for TMJD include:
- Genes that influence how you perceive pain
- Higher estrogen levels
- An injury to the jaw or TMJ
TMDs often come on suddenly and resolve on their own just as quickly. But in some cases, they are persistent (chronic) and require professional attention.
Who Needs TMJ Surgery?
Few people with TMD require surgery. Doctors only recommend TMJ surgery for severe cases when other conservative, non-invasive treatments have failed.
You may be a candidate for TMJ surgery if you have:
- Consistent and intense TMD symptoms
- Difficulty closing and opening your mouth
- Trouble eating or drinking because of your TMD
- No improvement in symptoms from more conservative treatments
- A structural issue or disease in your TMJ
TMJ surgery is generally irreversible. In addition, there’s no guarantee it will solve the problem.
For these reasons, experts recommend people suffering from TMDs try conservative, non-invasive treatments first. Surgery may be a logical next step in cases where other treatments have failed to resolve serious TMJ dysfunction.
Your doctor can help you determine if surgery is necessary.
5 Types of TMJ Surgery: Costs & What to Expect
Once your doctor has determined you as a candidate for TMJ surgery, they will decide which type is most appropriate for you.
Five types of surgical procedures address TMJ disorders. They range from minimally invasive outpatient treatments to intensive open-joint surgery.
1. Arthrocentesis
Arthrocentesis, also known as joint aspiration, is a minimally invasive procedure. It involves flushing the jaw joint with fluid from a syringe to remove tissue debris and reduce inflammation.
What to Expect
Arthrocentesis may be performed under general anesthesia or a combination of local anesthesia and IV sedation.
It’s generally an outpatient procedure, so you can go home the same day. It may take about half an hour to perform.
During the procedure, a surgeon will:
- Insert one or two hypodermic needles into the jaw joint.
- Flush the jaw joint with a sterile fluid, such as a saline solution. This will help remove any unwanted material, such as inflammation or tissue breakdown byproducts.
- Possibly remove scar tissue and inject the joint with medication.
Cost
Arthrocentesis can cost $300 or more.
2. Arthroscopy
Arthroscopic surgery involves opening one or several holes in the skin above the TMJ. Your doctor will use that opening to perform needed procedures on the joint.
What to Expect
TMJ arthroscopy requires general anesthesia. It’s slightly more invasive than arthrocentesis and may take longer.
It’s an outpatient procedure during which a surgeon will:
- Make small incisions around the TMJ and insert a thin metal tube called a cannula.
- Use the cannula to insert an illuminated camera called an arthroscope. They’ll use the arthroscope to inspect the joint.
- Perform any needed repair or removal procedures with surgical tools inserted through the cannula.
Cost
Arthroscopy can cost $5,000 or more per joint.
3. Arthrotomy or Arthroplasty (Open-Joint Surgery)
Rather than simply inserting tools through tiny incisions, open-joint surgery is more intensive. The joint space is opened completely to expose the jaw joint.
What to Expect
Open-joint TMJ surgery may take 1 to 2 hours and is performed under general anesthesia. You may need to spend the night in the hospital afterward.
During the procedure, your surgeon will:
- Expose the joint to be operated on by carefully making an incision a few inches long.
- Repair, reposition, or modify parts of the joint once they’ve opened up the joint space. This may include the cartilage disc of the TMJ.
Cost
The cost of open-joint surgery for TMJ disorders varies widely depending on the specifics of the procedure. It can cost $5,000 on the low end or up to tens of thousands of dollars.
4. Temporomandibular Joint Replacement
TMJ replacement is a special kind of open-joint TMJ surgery. Once the joint is exposed, your surgeon will replace it with bone taken from elsewhere in your body or with a prosthesis.
What to Expect
Joint replacement surgery is an inpatient procedure and may take more than an hour under general anesthesia.
Your surgeon will:
- Make one or more incisions to expose the joint
- Reshape or remove certain tissues
- Replace part of the TMJ, or the entire TMJ, with a prosthesis
Cost
TMJ replacement costs include both open-joint surgery and the replacement material itself. It may cost from $40,000 to $70,000.
5. Modified Condylotomy
A condylotomy is a kind of osteotomy that is essentially a controlled fracture.
The name condylotomy comes from the condyle, which is the rounded end of your lower jaw that fits into the TMJ. Increasing the amount of space for the condyle to move may ease TMJ pain and locking.
What to Expect
A modified condylotomy takes place under general anesthesia and lasts less than 2 hours. You may be able to go home the same day, but you’ll need several weeks to heal fully.
During the procedure, your surgeon will:
- Make an incision from the inside of your mouth to gain access to the bone.
- Cut the bone and position it properly
- Put the soft tissue surrounding the bone back in place.
Cost
A modified condylotomy typically costs between $15,000 and $30,000.
How Much Does TMJ Surgery Cost?
The cost of TMJ surgery depends primarily on the type.
| Type of TMJ Surgery | Cost |
|---|---|
| Arthrocentesis | $300+ |
| Arthroscopy | $5,000+ per joint |
| Arthrotomy/Arthroplasty | $5,000+ |
| Temporomandibular Joint Replacement | $40,000 to $70,000 |
| Modified Condylotomy | $15,000 to $30,000 |
Will Insurance Cover TMJ Surgery?
Insurance may or may not cover all or part of the costs of TMJ surgery. It depends on your insurance provider and your specific plan.
The cost of TMJ surgery can vary widely, depending on whether your insurance provides coverage and how your doctor prices the procedure.
Potential Complications of TMJ Surgery
Complications may result from invasive TMJ procedures. These include:
- Post-operative bleeding
- Infections
- New or persistent problems with the TMJ or other structures (e.g., injury to facial nerves or other nearby structures)
In some cases, these issues may require additional surgeries. Talk to your doctor for a better understanding of the procedure and to discuss specific risk factors.
TMJ Surgery Recovery Timeline
Recovery time from TMJ surgery depends on the specific procedure. Generally, the more invasive the surgery, the longer your jaw will take to heal.
| Arthrocentesis (Minimally Invasive) | After 1 to 3 days, you should be able to return to work, school, or other obligations. Your doctor might recommend jaw exercises and a soft diet. |
|---|---|
| Arthroscopy (Minimally Invasive) | Recovery can take anywhere from a couple of days to a week.You may receive physical therapy following recovery.You might be required to keep a soft diet for several weeks as your jaw heals. |
| Open-Joint Surgery or Joint Replacement (Invasive) | A full recovery may take anywhere from 2 weeks to several months.Recovery may be more painful than for less invasive procedures.Physical therapy will be a part of the recovery process. |
| Modified Condylotomy (Invasive) | You may need up to a week to rest before returning to work, school, or other obligations.Your doctor will use rubber bands to hold your upper and lower jaws together for several weeks.You’ll be required to follow a soft or liquid diet. |
Aftercare
Depending on the kind of surgery you’ve had, you may need days, weeks, or even months to heal and resume normal activities.
In the meantime, here are some guidelines:
- Listen to your doctor — They’ll advise you on how long to rest when you can go back to work or school, and what you need to do in the meantime.
- Stick to soft foods — You may be required to maintain a soft or even entirely liquid diet following surgery. Stock up on these foods before your surgery.
- Follow recovery guidelines — Your doctor might provide orthotic devices (such as mouth guards), and physical therapy sessions to help your jaw heal and strengthen.
- Take medication as needed — The pain and swelling following surgery may be intense. Your doctor may prescribe pain medication.
- Attend follow-up visits — Your doctor will likely want to see you a few times after surgery to check your progress. You may need to have stitches removed if they aren’t resorbable.
- Contact your doctor in emergencies — If you experience severe pain or have other symptoms such as fever or difficulty breathing, contact your doctor immediately.
Non-Surgical Treatment for TMD
You may not be a candidate for TMJ surgery. Your doctor may want you to try more conservative treatments before resorting to surgical procedures.
Less invasive treatments for TMD include:
- Physical (manual) therapy, which gently stretches and strengthens the muscles and soft tissues of the TMJ area.
- Cognitive behavioral therapy (CBT), which can help you stop clenching your jaw or grinding your teeth unconsciously.
- Medications to manage pain and inflammation such as Aleve, Advil, and/ or Flexeril, amongst others.
- Orthotic devices such as night guards or occlusal splints.
- Complementary treatments like acupuncture, which are unconventional but may be combined with conventional ones.
- Botox injections to relieve pain temporarily.
- Diet changes such as avoiding chewing gum, sticky foods like caramel, or hard foods like nuts.
In most cases, doctors and dentists only recommend TMJ surgery after these treatments have failed.
TMJ Surgery: Types, Costs, What to Expect, Procedure, and Recovery
NewMouth PodcastSources
- Murphy, M., et al. “Temporomandibular disorders: a review of etiology, clinical management, and tissue engineering strategies.” The International Journal of Oral & Maxillofacial Implants, National Library of Medicine, 2013.
- "TMD (Temporomandibular Disorders)." National Institute of Dental and Craniofacial Research, National Institute of Health, 2023.
- Smith, S., et al. “Potential genetic risk factors for chronic TMD: genetic associations from the OPPERA case control study.” The Journal of Pain, National Library of Medicine, 2011.
- Berger, M., et al. “Association between estrogen levels and temporomandibular disorders: a systematic literature review.” Menopause Review, National LIbrary of Medicine, 2015.
- “Surgical Management of TMJ Disorders.” American Society of Temporomandibular Joint Surgeons, 2023.
- “Surgery.” The TMJ Association, 2023.
- Wright, E. ,et al. “Management and treatment of temporomandibular disorders: a clinical perspective.” The Journal of Manual & Manipulative Therapy, National LIbrary of Medicine, 2009.
- Monje-Gil, F., et al. “Temporomandibular joint arthrocentesis. Review of the literature.” Medicina Oral, Patologia Oral y Cirugia Bucal, National LIbrary of Medicine, 2012.
- Murakami, K. “Rationale of arthroscopic surgery of the temporomandibular joint.” Journal of Oral Biology and Craniofacial Research, National Library of Medicine, 2013.
- Yoda, T., et al. “Clinical guidelines for total temporomandibular joint replacement.” The Japanese Dental Science Review, National Library of Medicine, 2020.
- Werther, J. "Modified condylotomy." Journal of Oral and Maxillofacial Surgery, Elsevier Inc, 2004.
- Puricelli, E., et al. “Clinical-surgical treatment of temporomandibular joint disorder in a psoriatic arthritis patient.” Head & Face Medicine, National Library of Medicine, 2013.

UCLA-trained dentist practicing in public health. Focuses on whole-body approach to dental care.
Related Articles

Bleeding Gums: Causes, Remedies & Treatment
Bleeding gums can be a sign of gum disease. They can also be caused by other things like brushing too hard or hormonal c...

What Causes Bumps Under the Tongue?
It's common to notice bumps, bubbles, or pimples under your tongue (ventral surface). They may appear suddenly and may n...

Is It Safe to Gargle With Hydrogen Peroxide?
Is it Safe to Gargle with Hydrogen Peroxide? Gargling with diluted hydrogen peroxide is safe when done correctly. Its po...
Misaligned or Crooked Jaw
The upper and lower jaws are meant to fit together evenly and painlessly. However, jaws can develop misaligned or uneven...
