Dental Abscess: Identifying and Treating It at Home
Reader-supported. We may earn a commission from links on this page. Advertising disclosure.
In this article
Although minor infections may heal on their own, neglecting dental abscesses can put you at risk of short and long-term complications. The pain can worsen, and infection can spread to other parts of your face.
This can severely damage your tooth and surrounding structures, leading to tooth loss or bone damage. Additionally, if the infection spreads into your bloodstream, you may be at risk of a life-threatening condition called sepsis.
How Can You Identify a Dental Abscess?
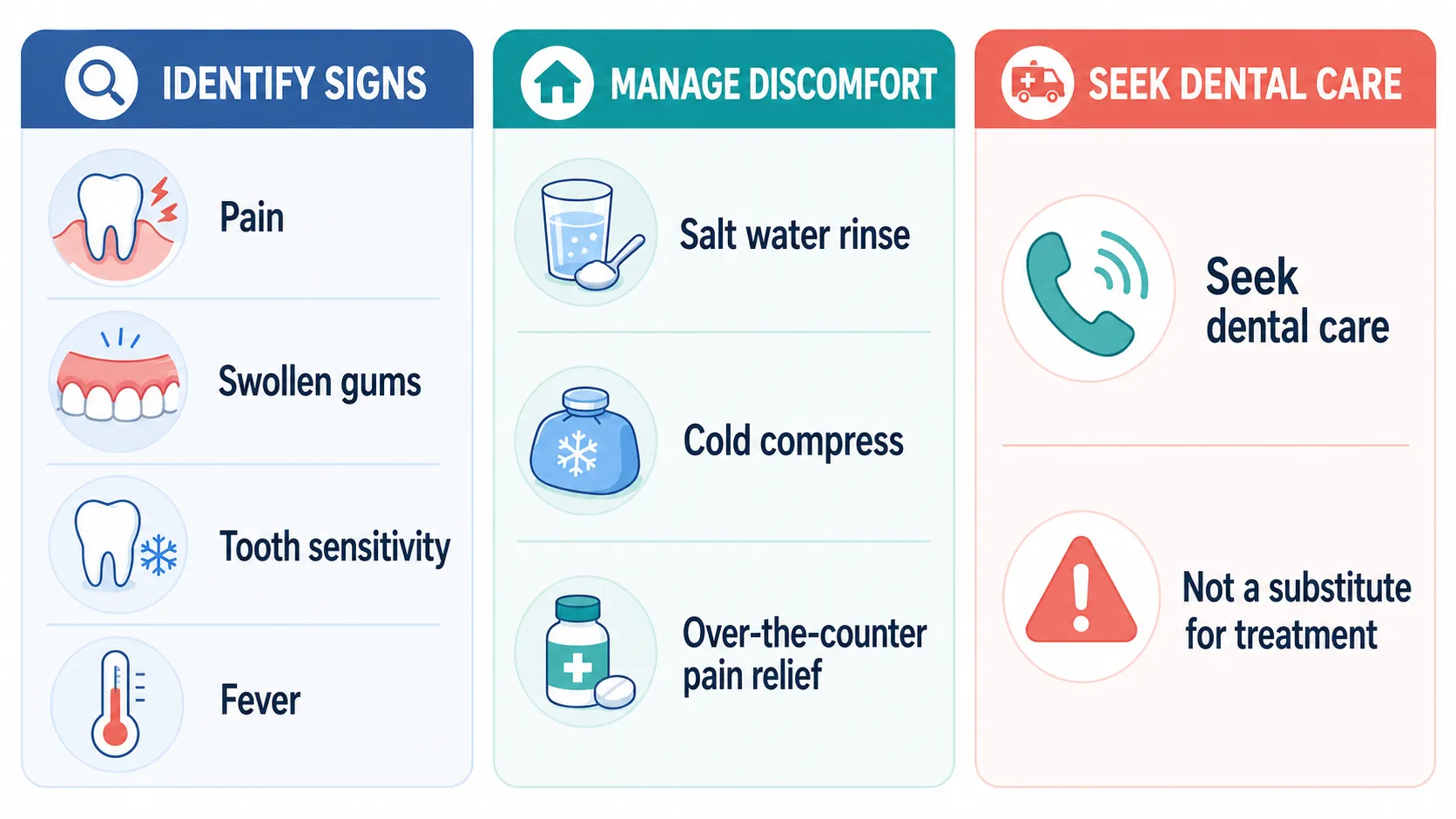
A dental abscess is a pocket of pus caused by a bacterial infection in your teeth or gums. There are different types of dental abscesses, and each type can influence the symptoms a person experiences and how quickly they need treatment.
- Periapical abscess — An infection that forms at the tip of the tooth’s root. It typically occurs when bacteria reach the dental pulp.
- Periodontal abscess — A collection of pus that forms alongside a tooth in the gums, specifically in the periodontal pocket.
- Gingival abscess — A localized infection in the gum tissue, also known as a gum abscess.
More general signs of a dental abscess include:
- A pus-filled bump
- Pain in the affected area
- Swollen glands or gums
- Tooth sensitivity
- Fever
- Bad taste in the mouth
- Bad breath
- Loose or shifting teeth
How to Manage Dental Abscess Pain At Home
Dental abscesses are often painful, so it is important to manage the symptoms while you wait for treatment.
Here are some things you can do while waiting for professional dental treatment:
- Salt water rinse to clean the area and reduce swelling
- Cold compress to reduce inflammation and swelling
- Crushed garlic for its antibacterial properties
- Clove oil for pain relief
- Tea for its anti-inflammatory properties
- Over-the-counter pain relievers (Ibuprofen, naproxen, etc.)
- Oral anesthetics and gels
You should also avoid foods and drinks that can worsen your pain. This includes sugary, starchy, hot, or cold foods and drinks.
Remember, these remedies aren’t a substitute for treatment. We still strongly recommend seeing a dental professional to treat your abscess.
When Should You See a Dentist for a Dental Abscess?
You should seek dental care immediately if you have a dental abscess, especially if you’re experiencing the following:
- Fever or general uneasiness
- Swelling that spreads to the face or neck
- Difficulty breathing or swallowing
- Persistent or severe throbbing pain
- Pain that doesn’t respond to over-the-counter pain relievers
- Bad taste in your mouth
- Visible pus or discharge
Your dentist will first examine the abscess with X-rays and a thorough exam. This helps them check for swelling and pus and see how deep the infection is and whether it’s reached the surrounding bone.
Typical treatment options for abscesses include:
- Incision and drainage — If there’s a pus buildup, your dentist might make a small cut to drain it, providing temporary pain relief.
- Root canal — Depending on the tooth’s condition, a root canal may be used to clean out the infection and save the tooth.
- Tooth extraction — In some cases, the damage can be too severe, so your dentist might remove the tooth entirely.
- Antibiotics — If the infection spreads, you might be prescribed antibiotics to fight it more effectively.
- Follow-up and prevention — Your dentist will want to see you again to ensure the infection is cleared and discuss how to prevent future abscesses.
The sooner you get treatment for a dental abscess, the better your chances of avoiding complications or lasting damage. If left untreated, the infection can spread and potentially become life-threatening.
What Causes Dental Abscesses?
Regardless of the type, a dental abscess is a sign of a serious infection. The potential causes for dental abscesses include:
- Tooth decay — The most common culprit of periapical abscesses, allowing bacteria to invade the inner tooth chamber.
- Gum disease — Severe gum disease weakens the attachment of teeth, creating spaces for bacteria to thrive within the gums.
- Trauma — A cracked or chipped tooth provides an entry point for bacteria.
- Foreign objects — Items like food particles or toothbrush bristles caught in the gums can lead to infection.
Although home remedies can help manage the discomfort, they won’t solve the underlying infection. If you think you have an abscess, talk to your dentist immediately.
How to Prevent Dental Abscesses
In most cases, dental abscesses are preventable. Maintaining good oral hygiene and avoiding harmful lifestyle choices can significantly lower your risk of developing dental abscesses.
Here are some tips to help do just that:
- Brush and floss regularly
- Use antibacterial mouthwash
- Clean your toothbrush after using it
- Visit your dentist regularly
- Limit alcohol consumption and quit smoking
- Eat healthy foods (leafy greens, fruits, plain yogurt, etc.)
- Avoid acidic and sugary foods
- Wear mouthguards during activities that can impact your face
- Take vitamins to boost your immune system
- Stay hydrated to wash away food debris
You should also take steps to manage systemic conditions linked to dental abscesses and infections, like diabetes. Managing these can reduce your risk of dental abscesses and other oral problems.
Dental abscesses can significantly affect your overall well-being. Although some remedies can provide temporary relief at home, they are not replacements for professional treatment.
If you notice the early signs of a dental abscess, get professional help immediately. Early treatment can help maintain your oral health and prevent long-term complications.
Sources
- “Dental Abscess.” Ada, 2022.
- Sanders JL. & Houck RC. “Dental Abscess.” Treasure Island (FL): StatPearls Publishing, 2023.
- Shweta, P. “Dental abscess: A microbiological review.” Dent Res J (Isfahan), 2013.
- Altıntaş E. “Complications of dental infections due to diagnostic delay during COVID-19 pandemic.” BMJ Case Reports CP, 2022.
- Bayetto et al. “Dental abscess: A potential cause of death and morbidity.” Australian Journal of General Practice, 2020.
- “Dental abscess.” NHS, 2022.

Board-certified general dentist specializing in patient education and preventive dentistry.
Related Articles

Dental Insurance No Waiting Period
Find out what a dental insurance waiting period is, why some plans have waiting periods, how to locate dental insurance...

Why is The Roof of My Mouth Yellow?
The simplest explanation for this discoloration is the food you've eaten. Certain foods and drinks, like coffee, tea, or...
What Food Should You Avoid To Maintain Good Oral Health?
When it comes to teeth, sometimes the tastiest foods can be the biggest culprits in creating problems. Bacteria in your...
What Are the Different Types of Tooth Files?
Tooth files are small precision instruments used to clean and shape areas inside teeth. Most dental files are made of st...
