Dental Abscess: Causes, Symptoms, Treatment, and Prevention
Reader-supported. We may earn a commission from links on this page. Advertising disclosure.
In this article
A dental abscess is a pocket of pus that forms due to a bacterial infection in or around a tooth. While it sounds alarming, it’s your body’s response to unwanted bacteria invading your tooth.
If left untreated, a dental abscess can cause bacteria to reach the tooth’s inner pulp or the surrounding gum tissue, resulting in pain, swelling, and a feeling of unease.
According to Dr. Nandita Lilly, one of NewMouth’s in-house dentists, “A dental abscess, if not treated accordingly, can lead to hospitalization. In some cases, it can be fatal.”
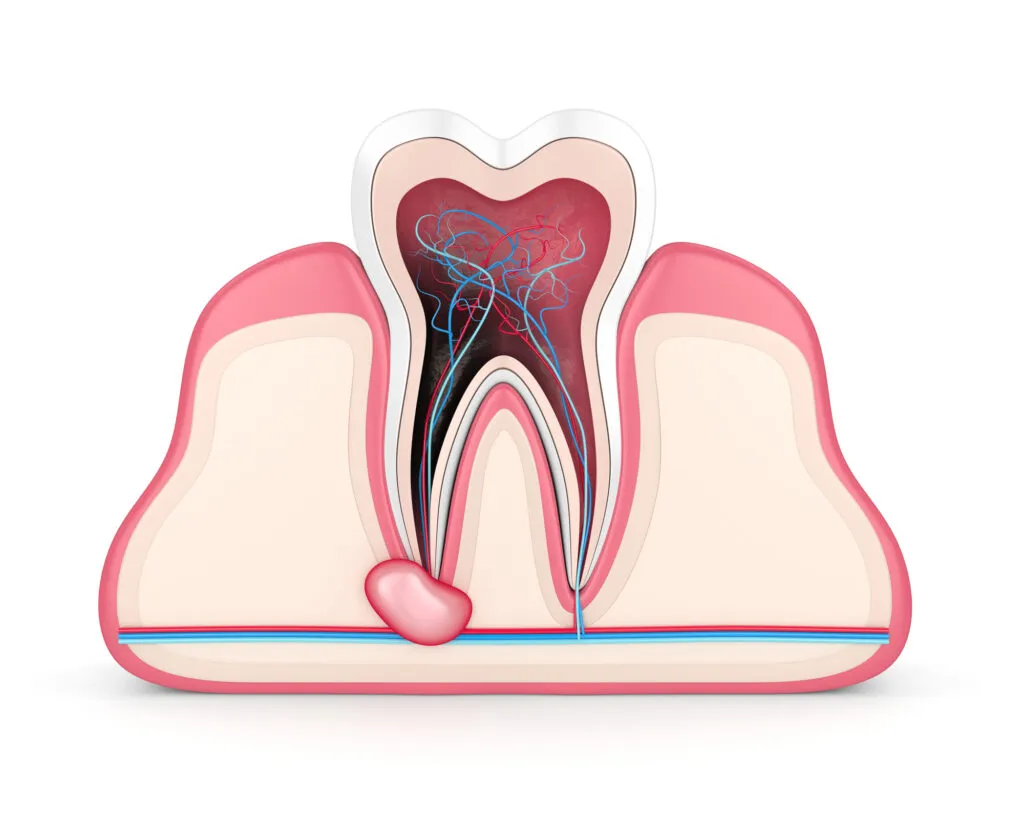
What are the Different Types of Dental Abscesses?
Three main types of dental abscesses form in different regions around a tooth. These include:
- Gingival abscess — Develops around the gums near the tooth base due to the impaction of a foreign object.
- Periodontal abscess — Develops inside the gum tissue and can affect the gums and bone surrounding the tooth.
- Periapical abscess — Develops in the tooth’s root due to bacteria entering the dental pulp (innermost layer of the tooth) through a cavity, crack, or chip in the tooth.

Inflammation of the gums or a tooth abscess
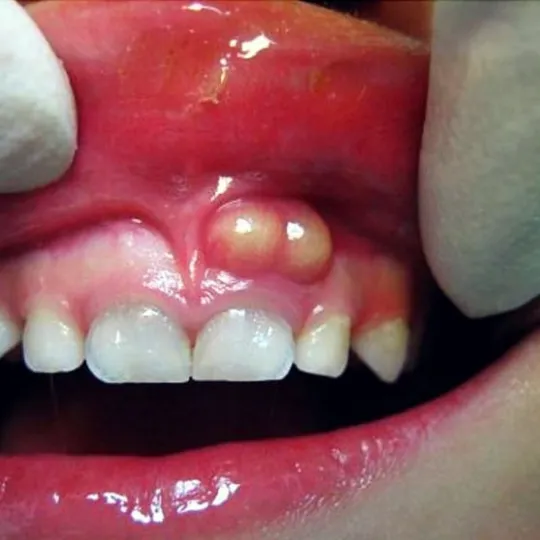
Inflammation of the gums or a tooth abscess
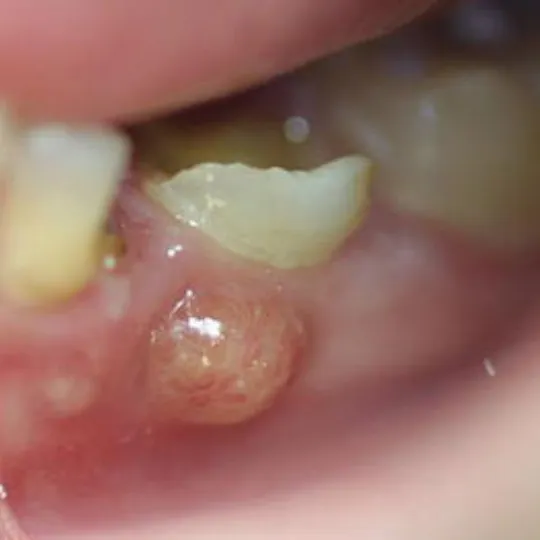
Inflammation of the gums or a tooth abscess
What are the Symptoms of a Dental Abscess?
Depending on the type of dental abscess and how long it has been progressing, common symptoms may include:
- Severe throbbing toothache
- Sensitivity to hot or cold foods
- Pain when biting down
- Discomfort that intensifies at night
- Red, swollen gums near the tooth
- Facial swelling around the cheeks, jawline, or under the eyes
- Feeling that the affected tooth is loose
- Fever and fatigue
- Bad breath and a foul taste in the mouth
The most dangerous symptoms of a dental abscess are having problems with breathing, swallowing, or opening your mouth (lockjaw). You should also call your doctor if you have a high fever and facial swelling around your throat or eyes.
These are warning signs that your body needs immediate medical attention. Getting immediate treatment can stop the infection before it compromises your health.
What Causes a Dental Abscess?
The most common cause of a dental abscess is neglecting oral hygiene. This can lead to a multitude of dental problems that can cause a dental abscess.
Other causes include:
- Injury — Injuries, dental damage, or deep tooth cracks allow bacteria to spread to deeper parts of the teeth or gums, leading to an abscess.
- Underlying medical conditions — Some conditions, like diabetes, HIV/AIDS, and a weak immune system, can increase the risk of developing abscesses.
- Medications and treatments — You may have a higher risk of developing an abscess if you’re taking steroids, chemotherapy, and antibiotics.
- Poor diet — Eating sugary or processed foods can increase the buildup of dental plaque, which can harden into calculus. This results in tooth decay.
- Previous dental issues — This includes cavities, failed dental work, impacted teeth, and tooth grinding.
How Does a Dental Abscess Form?
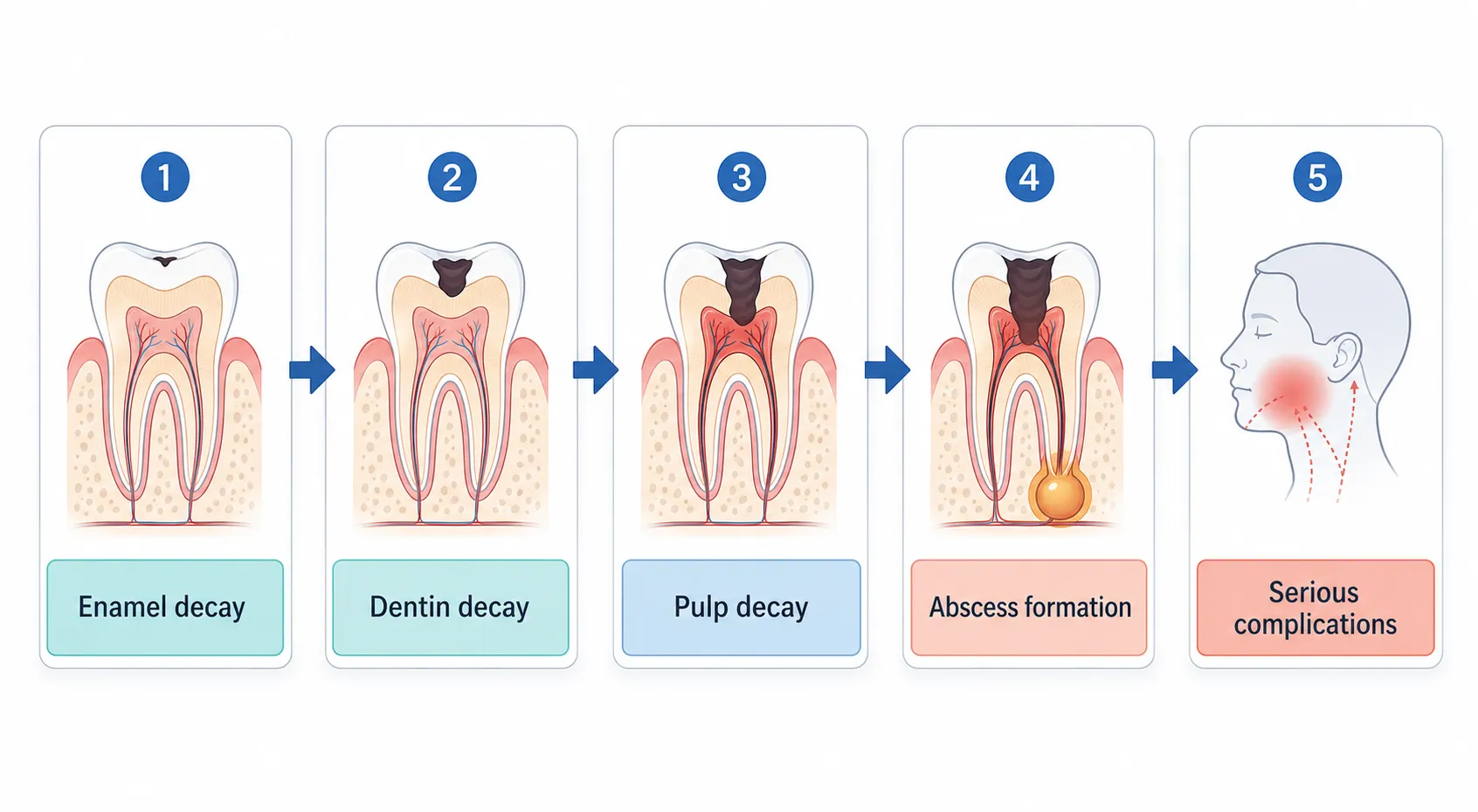
A dental abscess doesn’t happen overnight. It develops slowly, gradually building up from tooth decay to severe complications.
The stages of abscess formation may include:
1. Enamel Decay
The first stage is damage to the enamel or outer layer of the tooth. Plaque buildup on a tooth can often lead to enamel decay.
Some people may not experience symptoms because the decay is far from the nerve inside the tooth. Others develop tooth sensitivity or decalcified white spots prone to enamel breakdown.
2. Dentin Decay
If you don't treat your enamel decay, it will progress to the dentin layer of your tooth. Dentin is a bone-like, yellow-hued structure under the tooth's enamel layer.
Many people experience increased tooth sensitivity during this stage of decay, and for others, a small hole may develop in the tooth.
3. Pulp Decay
If untreated, the decay will progress to the pulp, the innermost layer of your tooth. This layer contains nerves, blood vessels, specialized cells, and connective tissues.
If bacteria reach this layer, they can attack the tooth’s nerve, causing severe pain. Eventually, the tooth’s nerve dies, and an abscess forms.
4. Abscess Formation
Once the bacteria reach your pulp, they can spread deeper into your gums or jawbone. Your gums may begin to swell, and you may notice a pimple-like bump on your gums.
The abscess formation may cause throbbing pain in your teeth, gums, and surrounding tissues.
5. Serious Complications
Leaving your tooth abscess untreated could lead to serious complications. For instance, severe tooth decay can cause your tooth to break and require extraction.
One of the more severe complications is sepsis. This is a life-threatening condition that happens when bacteria spreads to your bloodstream.
Other conditions include:
- Bone infection — Leaving the tooth untreated can result in an infection that affects surrounding facial bones.
- Sinus infections — Frequent, painful sinus infections or oral soft tissue infections can develop due to an untreated abscess.
- Septicemia — Septicemia is a life-threatening condition that occurs when your entire bloodstream becomes infected.
- Brain abscess — A dental abscess infection can travel to the brain, resulting in a brain abscess. This is life-threatening and requires treatment in the emergency room or hospital.
How is a Dental Abscess Treated?
A tooth abscess will not go away on its own. If a dentist does not drain it, it can spread to other areas of the body, including the jaw, head, neck, and bloodstream.
Three treatment options are available, depending on the type and severity of the infection. They are:
- Incision and drainage — Recommended when the abscess is treated early. Involves making a small incision to drain pus from the abscess before cleaning the infected area and prescribing antibiotics.
- Root canal treatment — A dentist removes the infected dental pulp before cleaning, shaping, and sealing the root canal system. They’ll also cover the tooth with a dental crown.
- Tooth extractions — This is typically used when the tooth can’t be saved. Your tooth may also be removed if it’s damaged from an injury, disease, or decay.
Many dentists recommend taking OTC painkillers while you wait for treatment. You can also take them after treatment alongside the antibiotics your dentist may prescribe.
How Long Does It Take to Recover From a Dental Abscess?
After an extraction, the infection will drain through the empty socket. The area can take ten days to a few weeks to fully recover after treatment.
Your dentist will schedule check-ups with you to ensure proper recovery. You may still have an infection if you are experiencing:
- Extreme pain, even with painkillers
- A fever
- Difficulty eating, speaking, or breathing
How to Prevent a Dental Abscess
The best way to prevent most oral conditions and diseases is to have good oral hygiene. This involves:
- Brushing your teeth twice daily with fluoridated toothpaste and a regular or electric toothbrush
- Replacing your toothbrush or toothbrush head every 3 to 4 months
- Flossing your teeth daily with dental floss, floss sticks, or a water flosser
- Use a fluoridated or antiseptic mouth rinse daily to prevent plaque buildup and tooth decay
- Visit your dentist for routine teeth cleanings, X-rays, and dental exams at least every six months
- Eating a balanced, healthy diet
- Reducing sugar intake
Dental Abscess: Causes, Symptoms, Treatment, and Prevention
NewMouth PodcastSources
- “Abscessed Teeth.” American Association of Endodontists.
- Hupp, J., and Ferneini, E. “Head, Neck, and Orofacial Infections: an Interdisciplinary Approach.” Elsevier, 2016.
- Sanders J.L., and Houck R.C. “Dental Abscess.” Treasure Island (FL): StatPearls Publishing, 2023.
- Shweta, P. “Dental abscess: A microbiological review.” Dent Res J (Isfahan), 2013.
- Erazo et al. “Dental Infections.” Treasure Island (FL): StatPearls Publishing, 2023.
- “Dental abscess.” NHS Choices, NHS, 2022.

Board-certified general dentist specializing in patient education and preventive dentistry.
Related Articles

ClearClub Custom Night Guard Review
ClearClub Custom Night Guard Reviews Pros These are some of the pros we found while scanning hundreds of reviews: Compet...

Can I Use Miswak Sticks to Clean My Teeth?
Miswak is a natural tool used for centuries to clean teeth. It's derived from the Salvadora persica tree (often referred...

What Causes Sores on Tongue?
What are Tongue Sores? Tongue sores, or ulcers, are common and can affect anyone, lasting from a few days to 2 weeks. 1...

The Benefits of Dental Probiotics
Your body is home to a unique set of microbes, and about 700 species live in your mouth. 5, 7 These include microscopic...
