Granulomatous Cheilitis
Reader-supported. We may earn a commission from links on this page. Advertising disclosure.
In this article
Granulomatous cheilitis is a rare condition that involves persistent lip swelling. It affects roughly 0.08% of the general population, particularly adults between the ages of 20 and 40.1

While not life-threatening, it can cause permanent damage to the lips if untreated.
What is Granulomatous Cheilitis?
Granulomatous cheilitis, or Miescher cheilitis, is a chronic inflammatory disorder affecting one or both lips.
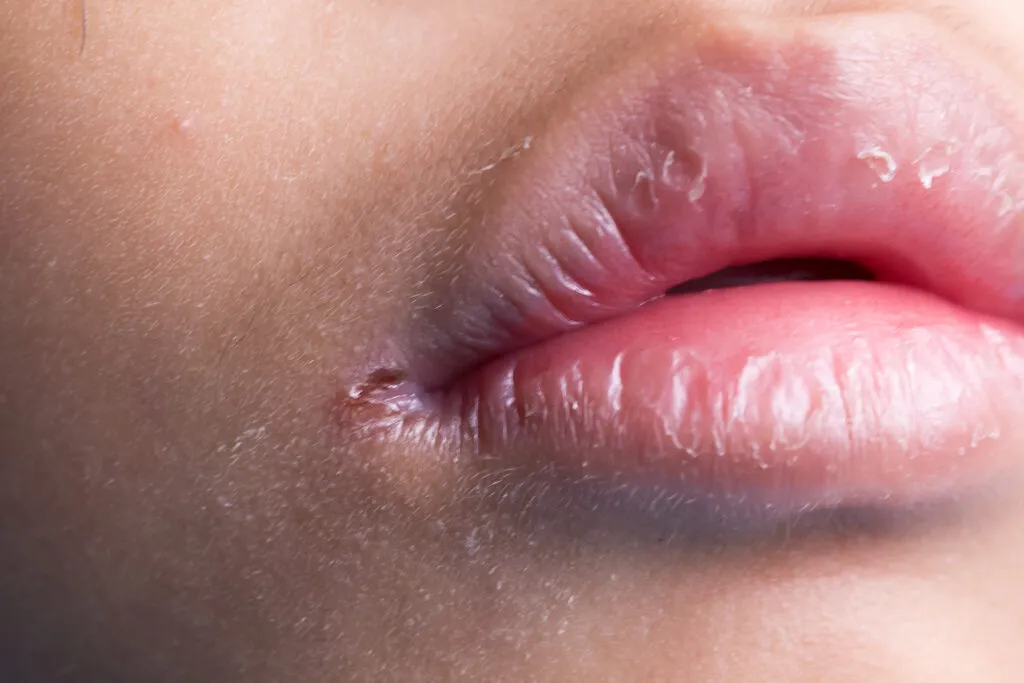
It’s characterized by lips that are:
- Swollen or puffy
- Hard and rubbery
- Dry and cracked
- Discolored
The swelling usually recurs on a long-term basis. It may last for a few hours or days at a time. You may also notice lumps on your cheeks and face.
The lumps and facial swelling associated with cheilitis granulomatosa are benign and usually painless.
What Causes Granulomatous Cheilitis?
Granulomatous cheilitis is often idiopathic, meaning it has no known cause. It’s connected to allergies, viruses, or infections in some people. In others, it may arise from a separate chronic inflammatory disorder.
Some of the possible causes associated with developing granulomatous disease are:
- Allergies or allergic reactions
- Genetic predisposition
- Medication side effects
- Immune response
- Infection
- Conditions such as sarcoidosis or Crohn’s disease
Who is Most Affected by Granulomatous Cheilitis?
Granulomatous cheilitis affects only a tiny fraction of the population, especially adults between 20 and 40. It’s rare in children and slightly more common in women.
Risk factors for the disease include:
- Atopy, or an inherited risk for developing allergies
- Food or other allergies
- Other inflammatory conditions
- Family history of inflammatory conditions
Differentiating Cheilitis Varieties
Cheilitis is a term that describes lip inflammation. Granulomatous cheilitis is one of several cheilitis varieties.
There are two main types of cheilitis: reversible and persistent. Reversible cheilitis can be resolved, whereas persistent cheilitis is typically chronic. Granulomatous cheilitis is the persistent type.
Reversible Cheilitis
Reversible cheilitis may go away on its own or with treatment. The varieties of reversible cheilitis include:
- Cheilitis simplex — The most common type of lip inflammation is brought on by environmental factors like cold, dry weather, or behaviors, such as lip licking.
- Angular/infective cheilitis — Certain infections and nutritional or immune deficiencies can cause the lips to swell.
- Contact/eczematous cheilitis — Allergies or contact with irritants can result in lip inflammation.
- Exfoliative cheilitis — This rare disease looks like skin peeling away from the lips and may come from stress, nutritional deficiencies, or picking at the mouth.
- Drug-related cheilitis — Lip inflammation can occur as a side effect of some medications.
Persistent Cheilitis
Persistent cheilitis means that it recurs or remains long-term. Besides granulomatous inflammation, the varieties of persistent or irreversible cheilitis include:
- Actinic cheilitis — This type is related to sun damage.
- Glandular cheilitis — This variety is connected to smoking, poor oral hygiene, and sunlight exposure.
- Plasma cell cheilitis — Characterized by dense plasma cells, this variety has no known cause.
These all tend to be rare.
Granulomatous Disorders in the Oral Mucosa
Granulomatous diseases encompass a variety of disorders that involve the formation of granulomas. A granuloma is a cluster of cells that manifests as chronic swelling or lumps.
These other granulomatous disorders affect the oral mucosa, which is the mucous membrane lining the inside of the mouth, cheeks, and lips. These disorders include:
- Orofacial granulomatosis — Granulomatous cheilitis is a form of orofacial granulomatosis. It involves the swelling of the lips, oral ulcers, a cobblestone-like appearance to the buccal mucosa (the membrane in the cheeks), and gingival swelling.
- Wegener’s granulomatosis — This disorder has the potential to be fatal. While the inflammation affects the oral mucosa, gums, and upper respiratory tract, it can also spread to other organs like the kidneys.
- Sarcoidosis — Though sarcoidosis most commonly affects the lungs, it can occasionally present with oral lesions inside the mouth and on the lips.
Granulomatous Cheilitis and Crohn’s Disease
Crohn’s disease is an inflammatory bowel disease (IBD) that causes inflammation and irritation in the digestive tract.
Preliminary research shows a possible connection between Crohn’s disease and developing granulomatous inflammation, though the exact association remains unclear. The inflammatory condition has been found in less than 1% of patients with Crohn’s disease.
Some studies suggest cheilitis granulomatosa might be an early warning sign of Crohn’s disease.
Understanding Associated Syndromes
Granulomatous cheilitis is commonly associated with a rare neurological disorder called Melkersson-Rosenthal syndrome.
The disorder causes recurrent orofacial swelling, facial paralysis, and folds in the tongue. This swelling is persistent and can become permanent.
Successful treatment for Melkersson-Rosenthal syndrome usually involves NSAIDs, corticosteroid therapy, antibiotics, and immunosuppressive treatments.
Symptoms and Clinical Manifestations
The primary symptom of orofacial granulomatosis is the swelling of one or both lips.
Other symptoms you might notice include:
- Puffy or lumpy lips
- Lumps or swelling in the cheeks
- Inflammation in the forehead, eyelids, or scalp (rare)
The first time it happens, the lip inflammation may occur suddenly and resolve within a few hours or days.
Typically, the lip enlargement will recur over a chronic basis and may last longer after the first bout, sometimes becoming permanent. Over time, your lips may also become:
- Dry and cracked
- Hard or rubbery
- Reddish-brown
- Peeling or bleeding
Significance of Swelling
Persistent idiopathic swelling (or chronic inflammation without a known cause) can indicate orofacial granulomatosis. It’s especially likely if you notice swelling in the upper or lower lip, cheeks, jaw, or forehead.
How is Granulomatous Cheilitis Diagnosed?
Your doctor will diagnose granulomatous cheilitis by clinically examining your oral and maxillofacial region. They’ll check any lumps or swelling and review your personal and family medical history.
Depending on what they find in their preliminary exam, your doctor may order tests for clinical and pathological analysis.
Diagnostic Tests and Procedures
Your doctor might run the following tests to determine whether you have cheilitis granulomatosa:
- Blood or urine tests to check for underlying conditions
- Allergy testing, like a skin prick test
- Biopsy of the swollen area to check for granulomas
These tests can help determine if you have a condition causing your orofacial granulomatosis, like an inflammatory disorder.
Always inform your provider if you’re experiencing other symptoms, such as gastrointestinal symptoms, as they could help make a diagnosis.
Differential Diagnosis
Since cheilitis granulomatosa shares symptoms with other conditions, you’ll need to see a doctor to determine the cause. Identifying between similar conditions is known as differential diagnoses.
Your doctor will check if you have facial palsy and a fissured tongue to rule out Melkersson-Rosenthal syndrome.
They’ll also ask about other symptoms that may seem unrelated to ensure you don’t have Wegener’s granulomatosis, sarcoidosis, or cutaneous tuberculosis.
Treatment for Granulomatous Cheilitis
While there’s no cure for orofacial granulomatosis, your doctor may prescribe certain treatments to reduce your symptoms. They may also recommend lifestyle changes to manage your health and prevent flare-ups.
Available Treatment Modalities
The most common successful treatment for granulomatous cheilitis is corticosteroids. Corticosteroids are an anti-inflammatory therapy that may help reduce swelling.
Depending on the severity of the inflammation, your doctor might prescribe a corticosteroid as a cream, mouthwash, oral medicine, or injection.
If you have a food allergy causing your condition, you may also need to make diet changes as part of your treatment.
Medications and Their Role
Your doctor may recommend other treatments if they discover an underlying condition related to your cheilitis granulomatosa. Common medications include:
- Antibiotics for infections
- Immunosuppressants
- Allergy medicine
By taking prescribed medications that treat your underlying issues, you may notice a reduction in your cheilitis or other symptoms.
Living With Granulomatous Cheilitis
Though granulomatous cheilitis can’t be cured, living comfortably while managing the condition is possible. The swelling tends to come and go, so you won’t always have inflammation in your lips.
When the inflammation flares up, you can use your prescribed corticosteroids. You may also need to take extra care of your lips during flares.
Prevention and Care Recommendations
You can’t prevent yourself from developing orofacial granulomatosis, but you may be able to learn your triggers and stop or ameliorate recurring flare-ups.
Tips for reducing your flare-ups and symptoms include:
- Avoid allergens such as foods, food additives, cosmetics, or other substances that cause an allergic reaction
- Eat an anti-inflammatory diet high in fruits and vegetables and low in processed foods
- Call your doctor if you develop other symptoms or need a prescription refill
Prognosis and Long-term Outlook
Cheilitis granulomatosa is typically chronic and will continue over the long-term. The swelling may come and go but has no cure.
If you have orofacial swelling, you should see your doctor to prevent permanent damage to your lips.
Summary
Granulomatous cheilitis, or Miescher cheilitis, is a condition that causes persistent swelling in the lips. It may also cause lumps in other parts of the face. It’s a chronic condition that recurs periodically and has no known cure.
Some underlying conditions, such as inflammatory disorders or allergies, may cause cheilitis granulomatosa. In other cases, there may be no obvious cause. Adults between the ages of 20 and 40 are at a higher risk for developing it, as are those with a genetic predisposition.
While there’s no cure for granulomatous inflammation, your doctor can treat underlying conditions that may be related, such as Crohn’s disease. They will also prescribe corticosteroids, an anti-inflammatory treatment, to reduce your symptoms.
What is Granulomatous Cheilitis?
NewMouth PodcastSources
- Jamil, R et al. “Cheilitis Granulomatosa.” StatPearls, National Library of Medicine, 2023.
- Lugović-Mihić, L et al. “Differential Diagnosis of Cheilitis – How to Classify Cheilitis?” Acta Clinica Croatica, National Library of Medicine, 2018.
- Dos Santos, H et al. “Plasma cell cheilitis: the diagnosis of a disorder mimicking lip cancer.” Autopsy Case Reports, National Library of Medicine, 2019.
- Alhassani, A et al. “Granulomatous diseases: Oral manifestations and recommendations.” The Saudi Dental Journal, National Library of Medicine, 2019.
- Triantafillidis, J et al. “Granulomatous cheilitis associated with exacerbations of Crohn's disease: a case report.” Journal of Medical Case Reports, National Library of Medicine, 2008.
- “Melkersson-Rosenthal Syndrome.” National Institute of Neurological Disorders and Stroke, National Institutes of Health, 2023.
- Devani, A. “Answer: Can you identify this condition?” Official Publication of The College of Family Physicians of Canada, National Library of Medicine, 2007.

UCLA-trained dentist practicing in public health. Focuses on whole-body approach to dental care.
Related Articles

Why is My Tongue Green and How Can it Be Cured?
Why Is My Tongue Green? Overgrowth of bacteria or other germs commonly causes a green tongue, though it can have other c...

Why Is My Tongue Black?
Why is my Tongue Black? Keratin (a protein) and bacteria/fungi buildup can cause a black tongue. Dark beverages or foods...

How Long Does the Healing Process Take for a Busted Lip?
A busted lip usually heals within a few days. Learn common causes, 7 home treatments, when to see a doctor, and how to r...
Cracked Teeth: 5 Types of Tooth Fractures
A cracked tooth can be a painful experience. Here's what you need to know about the five types of cracked teeth, how to...
