What is a Dry Socket & What Does it Look Like?
Reader-supported. We may earn a commission from links on this page. Advertising disclosure.
In this article
What is a Dry Socket?
A dry socket (alveolar osteitis) is a complication that can occur after a tooth extraction, particularly wisdom teeth. This condition arises when the exposed bone underneath the extraction site gets inflamed.
Typically, a blood clot forms in the socket—the space in the jawbone where the tooth was—to aid healing by protecting the underlying bone and nerves. However, if this clot dislodges or doesn’t develop, it leads to a dry socket.
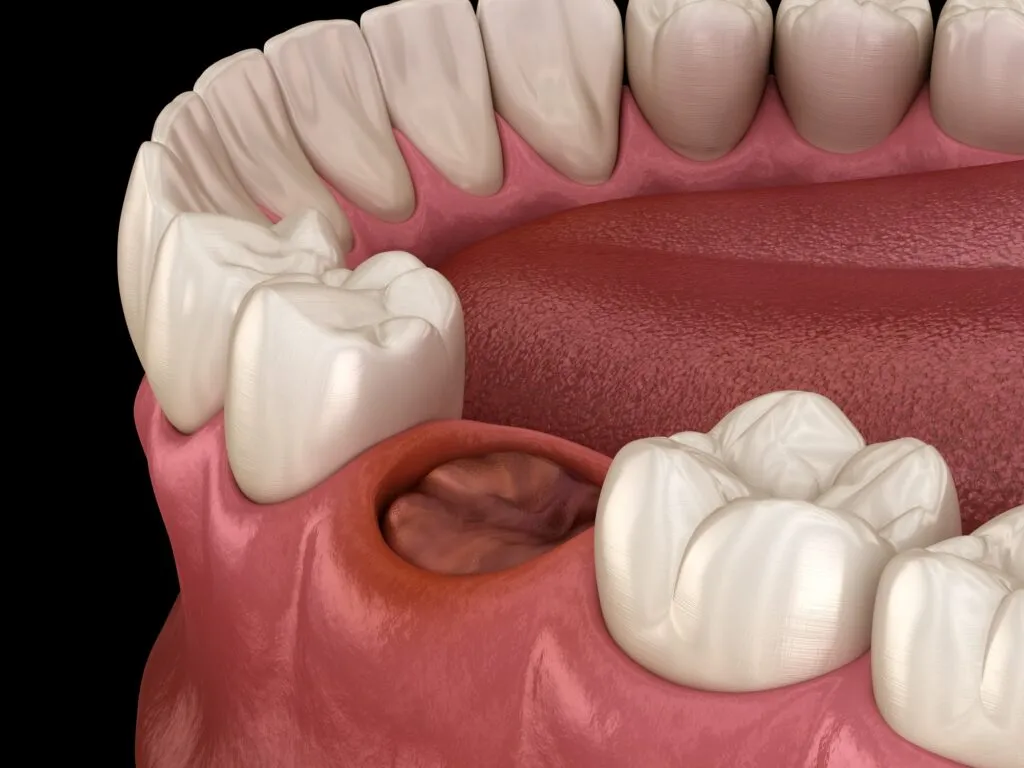
Dry socket is relatively uncommon, occurring in 1 to 5% of tooth extractions. However, it’s more frequent in wisdom tooth removals, affecting up to 38% of cases. It is most likely to develop in:
- The lower jaw
- People older than 30 years
- Females
- Infected teeth prior to surgery
What Does a Dry Socket Look Like?
A dry socket appears as a hole where the tooth was removed. You’ll see the bone that once surrounded the extracted tooth. The empty tooth socket where the tooth was pulled may appear dry or have a whitish, bone-like color.
Food debris or clumped bacterial material can entirely expose the socket bone or cover it. The socket may appear in various colors, including black, yellow, and green, when food debris or bacteria surround it.
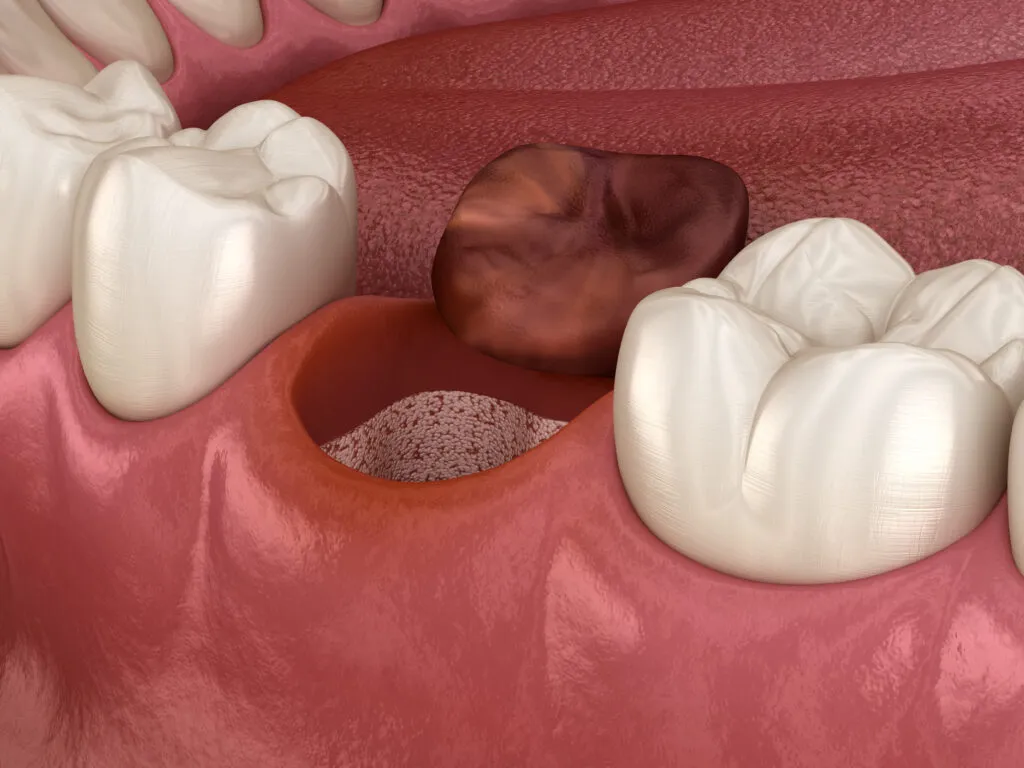
By contrast, a socket with a blood clot healing correctly should appear dark red. As the blood clot transforms into new tissue, it should gradually blend in with the rest of your gums.
What Causes a Dry Socket?
A dry socket forms when the blood clot doesn’t form, dissolve, or dislodge before the tooth removal site heals. According to Dr. Nandita Lilly, one of NewMouth’s in-house dentists, “the highest risk of dry socket development is within the first four days after surgery.”
Common risk factors for dry sockets include:
- Bacteria or an infection in the area
- Trauma due to a complicated extraction, like an impacted wisdom tooth
- Food particles that collect inside the socket
- Mechanical motions such as smoking, sucking through a straw, or aggressive rinsing and spitting
- Nicotine, alcohol, and carbonated drinks
- Changes in hormones due to menstruation or birth control pills
Symptoms of a Dry Socket
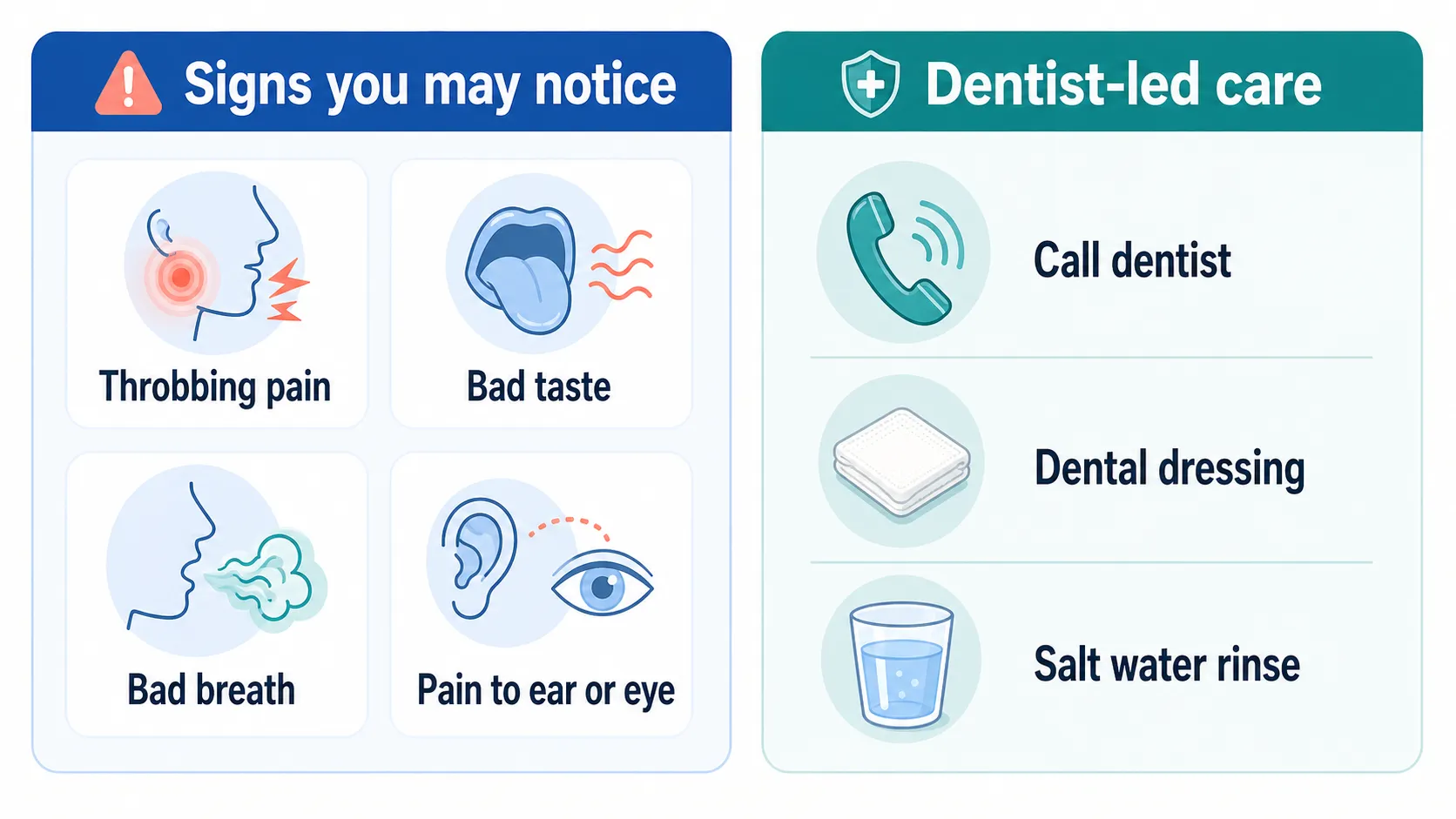
Symptoms of dry socket include:
- Throbbing pain that radiates from the socket and can extend up to the ear, eye, temple, or neck on the same side of tooth extraction
- Unpleasant taste in the mouth
- Bad breath or foul odor from the mouth
- Slight fever
Symptoms of dry socket typically begin within the first 2 to 4 days after oral surgery for tooth extraction. It can last several weeks.
If you underwent a tooth extraction more than a week ago and haven’t felt any intense pain since, it’s likely that the clot has started healing. This significantly reduces the likelihood of developing dry socket.
Dry Socket Treatment
If you begin to experience symptoms of a dry socket, contact your dentist or oral surgeon as soon as possible. Professional treatment for a dry socket typically consists of the following steps:
- Clean the extraction site with sterile saline (saltwater) and scrape the socket to promote blood flow.
- Fill the socket with medical dressings to prevent new food particles and debris from entering the tooth socket.
- Visit your dentist regularly to have them change the dressing after placing it during the healing process.
- Your dentist or oral surgeon may prescribe you antibiotics, pain medications, a special mouthwash, or irrigation solutions to assist in healing. You can also take over-the-counter pain relievers.
- Gently rinse your mouth with lukewarm salt water a few times daily and after meals. Avoid alcohol-based mouthwashes, as they increase the risk of dry sockets.
Caring for a Dry Socket at Home
To care for a dry socket at home, you should:
- Take pain medicine and oral antibiotics as your doctor prescribes
- Apply ice to the jaw
- Carefully rinse the dry socket as recommended by the dentist
- Apply clove oil to the extraction site for severe pain relief
- Eat soft foods until fully healed
- Refrain from smoking or drinking alcohol
Oral antibiotics don’t significantly decrease the risk of dry sockets because there are hundreds of bacteria types in the mouth. Therefore, you can still develop a dry socket even if you have good oral hygiene.
How to Prevent Dry Sockets
Try these practices after tooth extraction to avoid developing dry sockets:
- Avoid smoking, sucking motions, and drinking through straws
- Prevent strenuous exercise while the area is still healing
- Rinse your mouth gently because aggressive rinsing and spitting can make the blood clot fall out
- Refrain from brushing the extraction site for at least a week post-op
- Only gently brush the neighboring teeth around the extraction site.
- Until the extraction site heals, stick to soft foods like smoothies, eggs, soup, and mashed potatoes
- Refrain from drinking hot liquids, carbonated drinks, alcohol, and caffeine
These practices help your mouth heal and prevent a dry socket from forming. Be sure to follow them carefully.
Sources
- Mamoun, J. “Dry Socket Etiology, Diagnosis, and Clinical Treatment Techniques.” Journal of the Korean Association of Oral and Maxillofacial Surgeons, 2018.
- Navas et al. “Case report: Late Complication of A Dry Socket Treatment.” International Journal of Dentistry, 2010.
- "Dry Socket." HealthLinkBC.
- U.S. National Library of Medicine. “Dry socket.” MedlinePlus, 2022.
- Balaji et al. “Textbook of Oral and Maxillofacial Surgery.” Elsevier, a Division of Reed Elsevier India Private Limited, 2013.
- Daly et al. "Local interventions for the management of alveolar osteitis (dry socket)." Cochrane Database of Systemic Reviews, 2012.

UCLA-trained dentist practicing in public health. Focuses on whole-body approach to dental care.
Related Articles
What Are the Different Types of Tooth Files?
Tooth files are small precision instruments used to clean and shape areas inside teeth. Most dental files are made of st...

Proven Methods to Get Rid of Bad Breath
Bad breath (halitosis) is a common problem with various potential causes. A consistent oral hygiene routine is the best...

How Can You Finance Dental Care?
In the United States, high dental costs are a major barrier to care. Dental procedures can cost thousands of dollars, wh...

Is Dental Financing Possible with Bad Credit?
Bad credit can limit different aspects of your finances. If you have bad credit and need dental work immediately, it can...
