What to Expect During Wisdom Teeth Removal
Reader-supported. We may earn a commission from links on this page. Advertising disclosure.
In this article
Wisdom teeth are the third set of molars that usually emerge in your late teens or early twenties. However, they often lack enough space to erupt properly, leading to impaction, crowding, or the formation of cysts.
Dentists often recommend removing impacted wisdom teeth to prevent complications like pain, infection, or damage to surrounding teeth.
Why Do I Have to Remove Wisdom Teeth?
Early wisdom teeth removal is often easier and less complicated, especially when the roots are less developed. Younger people tend to experience faster healing and less downtime than older adults.
Addressing wisdom teeth early can save you potential discomfort and complications down the road. Even if your wisdom teeth don’t hurt now, they can cause trouble later.
Since they’re way in the back, they’re awkward to clean properly. This increases risks like:
- Partial eruption — When just part of the tooth pokes through, it creates a little pocket where food and germs love to hang out.
- Gum disease — Infection in those pockets, called ‘periodontal disease,’ can weaken the bone supporting your teeth.
- Damage to surrounding teeth — A wisdom tooth pushing sideways can cause cavities on the tooth right in front of it.
Do I Need a Wisdom Tooth Removal?
A few symptoms can indicate you should visit a dentist for wisdom tooth removal:
- Pain in the back of the mouth
- Inflamed or bleeding gums
- Fluid-filled sacs or cysts
- Earaches or headaches
- Jaw pain or stiffness
- Crooked or overcrowded teeth
- Fever and swollen glands
What Happens During Wisdom Teeth Removal?
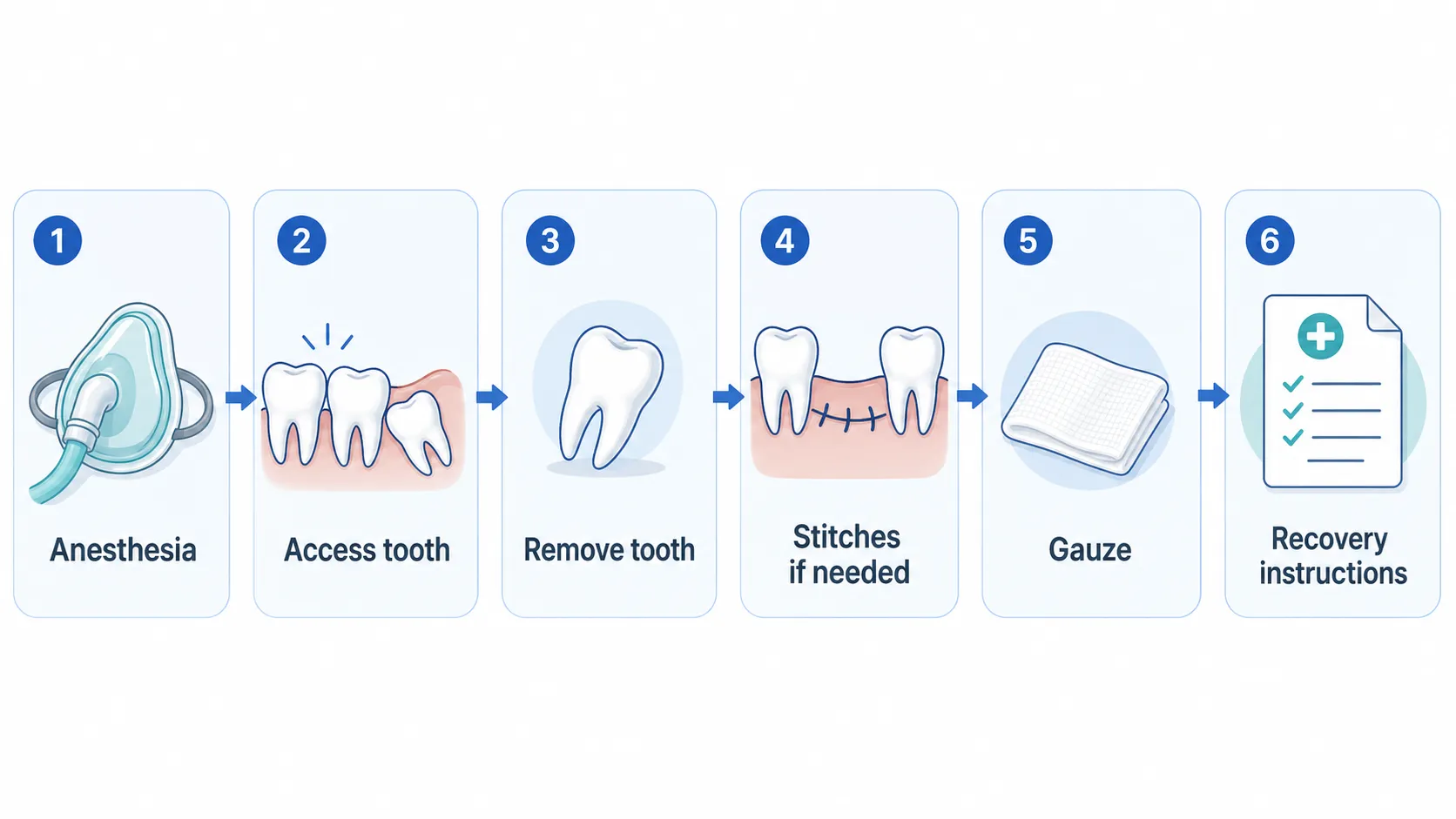
What you can expect during wisdom teeth removal varies depending on your teeth. Here’s a basic step-by-step rundown:
- Your dentist will ensure your comfort throughout the process, either through numbing the area or providing sedation, depending on your preference and the complexity of the procedure.
- Using specialized tools, your dentist will carefully loosen and remove the wisdom tooth. Sometimes, they may need to divide the tooth into smaller sections for easier extraction.
- If necessary, your dentist may place dissolvable stitches to promote faster gum tissue healing.
- To control bleeding and aid in clot formation, your dentist will place gauze over the extraction site, and you’ll need to bite down on it for a short period.
Does Wisdom Teeth Removal Require Anesthesia?
Most wisdom teeth removal procedures don’t require anesthesia. However, your dentist may use a local anesthetic to numb the area. This will numb the extraction site so you don’t feel any pain during the procedure.
Your dentist may recommend IV sedation or nitrous oxide for people anxious about the procedure. General anesthesia is only used in special cases, like complex surgery or severe anxiety.
How Much Does Wisdom Teeth Removal Cost?
A simple wisdom tooth extraction (non-impacted wisdom teeth) usually costs $75 to $200 per tooth. For impacted wisdom teeth, you can expect to pay around $225 to $600 per tooth.
Most dental insurance plans cover up to half the cost of wisdom teeth removal if the procedure is medically necessary.
What Happens After Wisdom Tooth Removal?
Wisdom teeth removal is usually safe, but it’s important to know both the normal healing process and signs that something is off.
During the first week after the procedure, expect the following:
- Some bleeding and pinkish saliva for the first day or so is normal
- Swelling that peaks after a few days, then slowly goes down
- Pain around the first 48 hours
- A sore throat may happen due to the breathing tube used with some sedation
After the procedure, you must apply gentle pressure on the gauze pad placed over the extraction site for at least 30 minutes to control bleeding. You should also relax and avoid strenuous activity for the rest of the day.
Other aftercare tips include:
- Avoid rinsing or spitting — This can dislodge the blood clot and delay healing.
- Stick to soft foods and liquids — Choose foods like soup, yogurt, and mashed potatoes.
- Avoid smoking and alcohol — These can interfere with healing and increase the risk of complications.
- Manage pain properly — Take prescribed or over-the-counter pain medication as directed.
When to Call Your Doctor
You must inform your doctor right away of the following:
- Soaking through gauze pads after a few hours or if bleeding is persistent or heavy
- A fever after surgery (could be a sign of infection and should not be ignored)
- If your pain intensifies or becomes unmanageable despite medication
- Nausea or vomiting that doesn’t subside or becomes severe
- Numbness in the lips, chin, or tongue after surgery that persists for more than a few days
Always follow your dentist’s instructions and monitor for complications. Contact your dentist if you experience excessive bleeding, severe pain, fever, or unusual symptoms.
Sources
- Ouassime et al. “The wisdom behind the third molars removal: A prospective study of 106 cases.” Ann Med Surg (Lond), 2021.
- “How it's performed - Wisdom tooth removal.” NHS.
- “Wisdom teeth: Learn More – Should you have your wisdom teeth removed?” InformedHealth.org, Updated 2023.
- “Removing wisdom teeth.” Healthdirect Australia Limited.
- Yoon JY, Kim EJ. “Current trends in intravenous sedative drugs for dental procedures.” J Dent Anesth Pain Med, 2016.

UCLA-trained dentist practicing in public health. Focuses on whole-body approach to dental care.
Related Articles
How Much Does Wisdom Tooth Removal Cost?
Find out how much it costs to have your wisdom teeth extracted. Our simple guide will discuss the cost of wisdom tooth e...
General Dentistry: Common Treatments & Procedures
General dentists are the most common dental providers, offering oral surgery, restorative services, and preventive care....
Dental X-rays: Types & Risks
Dental X-rays help detect cavities, bone loss, and other oral health issues early. Here are the common types of dental X...

The 7 Symptoms of a Cavity
A cavity is a small hole in your tooth that can be caused by decay. Read about cavities, including their causes, signs,...
