Gum Flap Surgery: Treatment Steps, Aftercare & Risks
Reader-supported. We may earn a commission from links on this page. Advertising disclosure.
In this article
If your dentist or periodontist mentioned “gum surgery,” you might be feeling nervous, especially if the idea is new to you. Gum flap surgery, also called periodontal flap surgery, is a common procedure to treat severe gum disease and protect your teeth from further damage.
When caught early, gum disease may be managed with deep cleanings and good home care. But if the infection has caused deep pockets or bone loss, surgery may be the next step.
This guide explains what gum flap surgery involves, who it’s for, and what recovery looks like, so you can make a confident, informed decision.
What is Gum Flap Surgery?
Gum flap surgery is a type of pocket reduction surgery used to treat severe gum disease (also called periodontitis). The goal is to reduce the depth of gum pockets that have formed around your teeth.
Healthy gums usually hug your teeth closely. But with periodontitis, the gum pulls away and forms spaces—or “pockets”—that collect bacteria.
When these pockets are deeper than approximately 5–6 mm, it becomes more difficult to clean below the gumline, and the infection can worsen. Gum flap surgery helps reduce these pockets by opening the gums, thoroughly cleaning the area, and then suturing the gums into a more natural, tighter position.
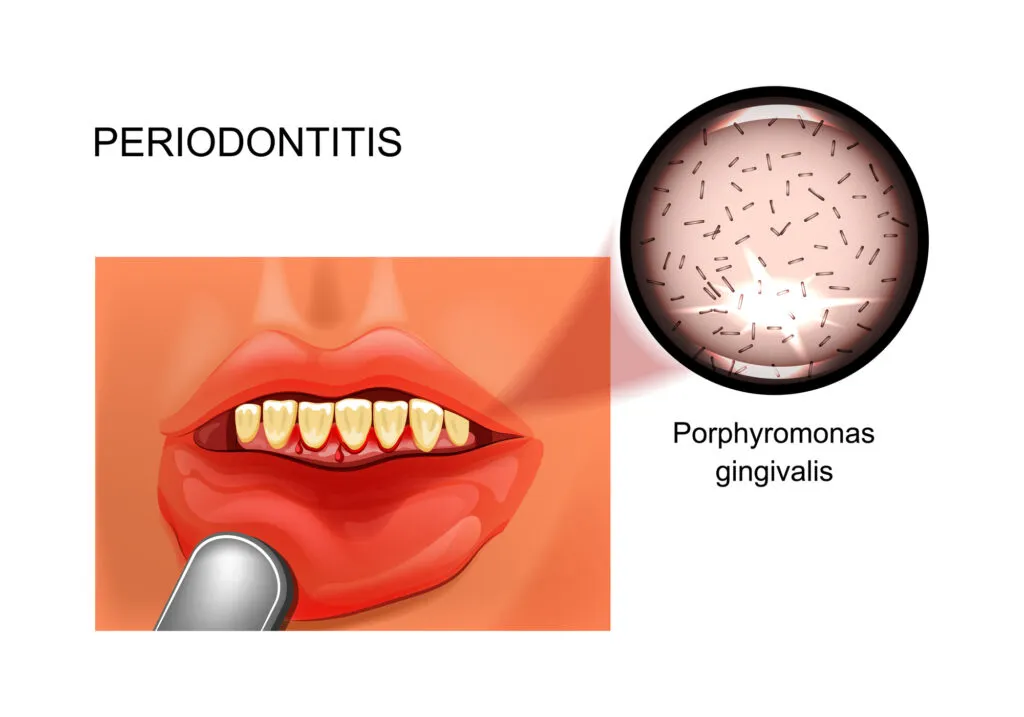
What You Need to Know About Gum Disease
Gum disease starts with plaque buildup that irritates the gums. In its early stage (gingivitis) it causes redness and bleeding.
If not treated, it can progress to periodontitis, where the infection damages the bone and ligaments that support your teeth. Over time, this can lead to tooth loss.
Periodontitis is common and chronic. Treatment helps stop the damage and stabilize your oral health, but it requires ongoing care.
How Gum Surgery Helps
Gum flap surgery lets your periodontist clean deep below the gums. After numbing the area, they make small incisions and gently fold back the gum tissue. This gives them access to remove hardened tartar and infected tissue around the roots.
In some cases, they may reshape the bone or place a graft if there has been bone loss. Once the area is clean, the gums are repositioned and sutured in place. With shallower pockets, it becomes much easier for you—and your dental team—to keep your mouth clean and healthy.
Your periodontist will explain which techniques are right for your situation.
Who Needs Gum Flap Surgery?
If your gum disease is severe and hasn’t responded fully to deep cleanings, your dentist may recommend gum flap surgery.
This procedure is typically reserved for cases where pockets remain deep—usually 5 mm or more—and there’s visible bone loss on X-rays.
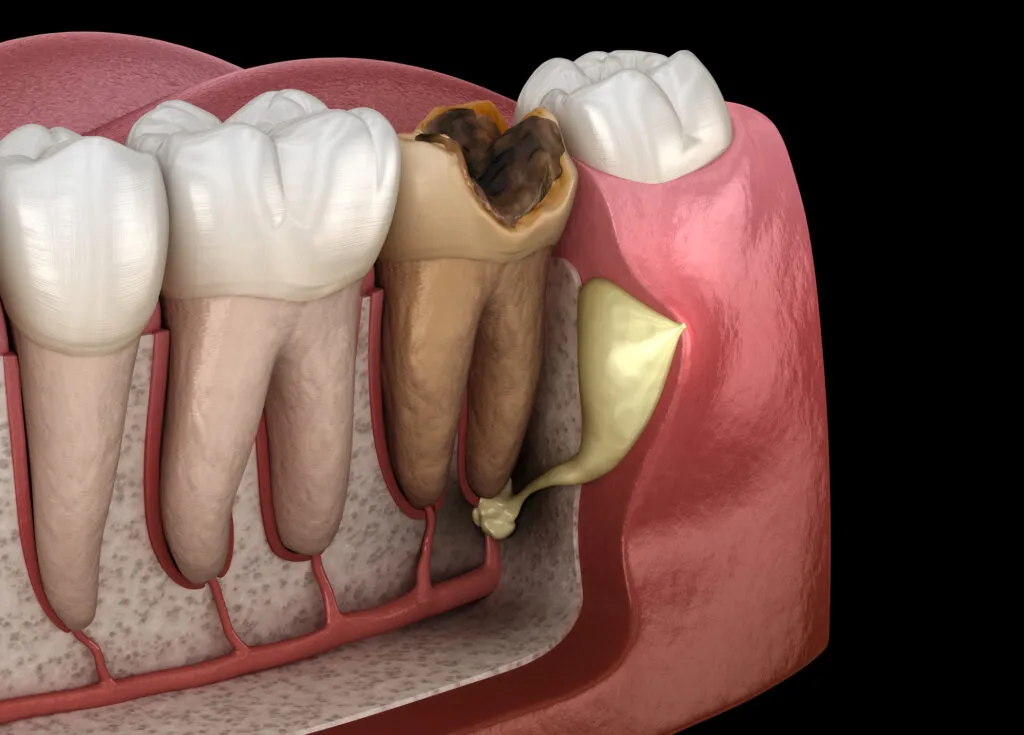
Symptoms of Severe Gum Disease
Advanced gum disease doesn’t always cause pain, but it does leave signs. You might notice:
-
Bleeding gums when brushing or flossing
-
Swollen or red gum tissue that feels tender
-
Bad breath that doesn’t go away
-
Gums pulling away from the teeth (recession)
-
Loose teeth or discomfort when chewing
If you have any of these symptoms, your dentist may measure your periodontal pockets and recommend the next steps.
During a periodontal exam, your dentist or hygienist will gently probe around your teeth to measure pocket depth. Healthy gum pockets have depths of 1 to 3 mm. Deeper pockets may signal attachment loss and infection below the surface.
X-rays help reveal whether the bone that supports your teeth has started to break down. Together, these tools guide whether non-surgical cleaning is sufficient or whether surgery is needed to prevent further damage.
Benefits and Risks of Gum Flap Surgery
Surgery can sound intimidating, but its goal is simple: to stop the damage, reduce harmful bacteria, and help you keep your natural teeth longer.
Benefits Over Time
The primary benefit of gum flap surgery is the reduction of deep pockets that harbor bacteria. With shallower pockets, it becomes easier to clean your teeth effectively and maintain healthy tissue.
Over time, this lowers the risk of further bone loss and tooth loss. Some people also notice less gum bleeding, fresher breath, and better stability in their bite.
Side Effects of Gum Surgery
Because the gum is repositioned to a tighter fit, it may not cover the root as fully as before. This can lead to:
-
Gum recession, making teeth look longer
-
Tooth sensitivity, especially to cold or brushing
-
Increased risk of root decay if oral hygiene isn’t maintained
These are common and manageable. Your dental team may suggest using a fluoride rinse, desensitizing toothpaste, or bonding exposed root areas if needed.
Though uncommon, some people may experience:
-
Prolonged bleeding
-
Infection around the surgical site
-
Swelling that doesn’t go down after a few days
These issues aren’t typical, but they require prompt care. If something doesn’t feel right, your periodontist wants to hear from you.
Ask your dental team what outcomes you can realistically expect from your procedure, and how to manage any side effects.
How To Prepare For Gum Flap Surgery
Good preparation makes your surgery and recovery smoother. Your dentist or periodontist will walk you through specific instructions, but here are the most common steps.
Medication Check
Let your dental team know about all medications and supplements you take, including aspirin, blood thinners, and pain relievers. In some cases, your provider may consult with your doctor before the procedure.
You should never stop prescribed medications without medical advice. Some people may be prescribed an antibiotic to take before surgery, depending on their medical history or infection risk. Others might receive a mild anti-anxiety medication or sedation option if they’re feeling nervous.
Lifestyle and Logistics
To help your body heal:
-
Avoid smoking and other tobacco products before surgery and during healing (your periodontist may recommend at least a week or longer)
-
Avoid alcohol before the procedure and during early healing—especially if you’ll be taking sedatives or prescription pain medication (follow your dental team’s instructions)
-
Arrange for a ride home if you’re receiving sedation or medication that affects alertness
-
Set up soft foods and oral care supplies at home before surgery day
Staying hydrated, getting good rest, and following your dentist’s instructions will all support a better recovery.
Gum Flap Surgery Step By Step
The procedure follows a clear series of steps designed to treat infection and support healing. You’ll be awake and comfortable throughout.
Numbing First
Your periodontist will begin by injecting a local anesthetic to numb the area completely. This stops pain signals, so you won’t feel discomfort, though you may notice some pressure or movement.
If you’re anxious, your dentist may also offer a sedative to help you stay calm. Some people receive a pill, nitrous oxide (laughing gas), or intravenous sedation.
Making Flaps
Once you’re numb, the periodontist makes a small incision to separate the gum tissue from your teeth. The gums are gently lifted to expose the tooth roots, ligaments, and surrounding bone.
This access enables more thorough cleaning than non-surgical methods can provide.
Cleaning Roots
Using special tools, the periodontist removes hardened plaque and tartar from the roots. Any inflamed or infected soft tissue is also cleared away.
If bone has been lost or reshaped by the infection, they may smooth irregular surfaces or perform a bone graft. This can help regenerate bone and improve support for the teeth. Some procedures also use barrier membranes or growth factors to improve healing.
Closing Gums
After cleaning, the gums are repositioned and closed with stitches. These may be dissolvable or require removal in about a week.
A protective periodontal dressing may be placed to shield the site from brushing or chewing while it heals.
Your dental team will schedule a follow-up visit to check healing and remove stitches if needed.
Gum Surgery Recovery and Post-Op Care
The first few days after surgery are the part that most people worry about. But with the right care, recovery is usually smooth and manageable.
First Few Days
Mild swelling, sensitivity, and slight bleeding are normal. These symptoms usually improve within a few days.
To support healing:
-
Take prescribed or over-the-counter pain relievers as directed
-
Apply ice packs (10–15 minutes on/off) for the first 24 hours to reduce swelling
-
Avoid smoking or drinking alcohol during early healing
-
Do not brush or floss the surgical site until your dentist says it’s safe
-
Starting 24 hours after surgery, rinse gently with warm salt water or a prescribed antimicrobial rinse like chlorhexidine
If bleeding is heavy or swelling worsens, especially after the second day, call your dentist. These signs may require follow-up, even if they don’t always mean infection.
Eating Soft Foods
For the first week or two, stick to cool, soft foods that won’t irritate the area. Good choices include:
-
Yogurt, pudding, and Jell-O
-
Scrambled eggs and mashed potatoes
-
Pasta, smoothies, and soft fruits
Avoid crunchy, spicy, or seedy foods until your gums have healed and stitches are gone.
Long-Term Gum Health After Surgery
Surgery is the start of long-term gum care, not the end. To keep the benefits, you’ll need to stay on top of hygiene and maintenance.
Your dentist may schedule cleanings every 3 to 4 months to monitor your gums and remove any new buildup. At home, daily brushing and flossing—or interdental brushes or water flossers—are key to keeping pockets from reforming.
Because gums may recede slightly after surgery, some tooth roots can be exposed. This increases the chance of root sensitivity and root decay. Using fluoride toothpaste or rinses, desensitizing pastes, or protective dental bonding can help.
In some cases, a gum graft may be recommended later if recession becomes severe. Staying smoke-free, managing diabetes, and wearing a night guard (if you grind your teeth) can also improve your long-term results.
Costs and Treatment Planning
Cost is often the biggest worry, but there are ways to plan for it. Treatment ranges depend on how severe your gum disease is and what procedures you need.
- Non-surgical treatments like scaling and root planing usually cost $200–$300 per quadrant (one-fourth of the mouth).
- Gum flap surgery can cost between $1,000 and $3,000 for a localized area.
- More extensive cases involving grafts or sedation may cost more.
Most dental insurance plans cover periodontal treatments—often 80% for non-surgical care and 50% for surgical procedures. Your provider may also offer payment plans, financing, or refer you to a dental school for lower-cost care.
The best way to understand your cost is to ask for a written treatment plan and check with your insurance before scheduling.
When to Call Your Periodontist
Knowing when to call helps you feel safer during healing. Mild symptoms are expected—but some signs mean you should get in touch.
Call your dentist right away if you notice:
-
Bleeding that doesn’t slow after applying gentle pressure with gauze for 20–30 minutes
-
Worsening pain, swelling, or pressure
-
Pus, unusual discharge, or a foul odor
-
Fever or chills
-
Difficulty swallowing or breathing
Even if you’re unsure, it’s always better to check. Save your dental office’s number in your phone before surgery day, including their after-hours line if they have one.
Next Steps For Your Gum Health
You do not have to figure this out alone. Gum flap surgery is a common procedure that helps manage severe gum disease and protect your teeth long term.
If you’ve been told you might need surgery, talk to your periodontist about your options. Ask what outcomes they expect, how to prepare, and what support you’ll need during healing.
The sooner you take the next step, the better your chances of preserving your smile.
Sources
- American Academy of Periodontology. “Surgical procedures.” perio.org, n.d.
- Healthline. “Periodontal surgery: Preparation, procedure, recovery, cost and more.” Healthline, 2018.
- Humana. “Gum disease (periodontal) treatment – dental costs & coverage.” Humana, 2020.
- Jennifer L. McCoy, DDS. “Periodontal flap surgery.” Jennifer L. McCoy, DDS, n.d.
- Mayo Clinic. “Periodontitis - Diagnosis and treatment.” Mayo Clinic, 2022.
- StatPearls. “Overview of periodontal surgical procedures.” NCBI Bookshelf, 2024.
- Virginia Family Dentistry. “Periodontal post-op instructions.” Virginia Family Dentistry, n.d.

Board-certified general dentist specializing in patient education and preventive dentistry.
Related Articles
LANAP Laser Gum Surgery
LANAP Laser Gum Surgery is a new and innovative gum disease treatment. This article discusses the benefits and costs of...
Full Mouth Debridement - Procedure, Costs & Prevention
What is Full Mouth Debridement? Full mouth debridement is a non-surgical dental procedure. It removes plaque and tartar...
Periodontal vs. Regular Teeth Cleaning
Unsure of the difference between a periodontal cleaning and regular cleaning? Here's everything you need to know about t...
Types of Bone Grafts, Complications & Risks
What is a bone graft? Discover everything you need to know, including the five types of bone grafts, side effects, post-...
