What Is Tooth Resorption?
Reader-supported. We may earn a commission from links on this page. Advertising disclosure.
In this article
Tooth resorption occurs when the immune system breaks down a tooth, essentially eating away at it. This makes the tooth non-restorable and in need of an extraction.
Tooth resorption isn’t common, but it happens from time to time. It can occur in both adult and primary (baby) teeth, but it’s normal and not usually harmful in baby teeth.
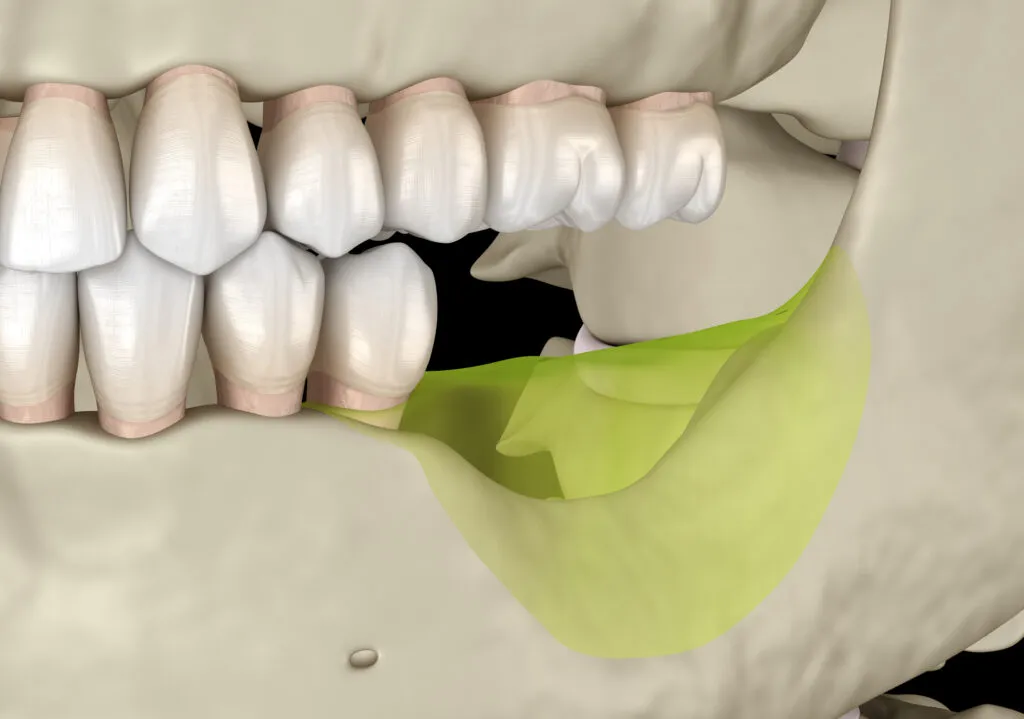
Without the normal resorption of baby teeth, they won’t fall out easily and make space for the adult teeth to erupt.
What are the Types of Tooth Resorption?
Tooth resorption is a condition where the tooth structure gradually erodes. This can occur in three primary ways: internal, external, or combination.
External resorption originates from the outside of the tooth, typically affecting the cementum, which is a thin layer covering the root of the tooth inside the gum socket.
There are three main classifications of external resorption:
- Inflammatory external resorption — Often linked to trauma or surgical procedures, this type can lead to significant tooth loss if left untreated.
- Surface external resorption — This milder form of resorption often heals on its own without intervention.
- Cervical external resorption — Primarily affecting the neck of the tooth, this type can be caused by prolonged trauma or other factors.
Internal resorption is less common and originates from within the tooth, often affecting the pulp. It can be triggered by factors such as trauma or deep fillings. While often asymptomatic, it can be detected on dental X-rays as dark spots within the tooth.
What Causes Tooth Resorption?
Numerous things can cause resorption, but the most common occurs after a trauma or dental surgery.
Other causes of tooth resorption include the following:
- Chronic teeth grinding
- Consistently bleaching the teeth with teeth-whitening products
- Rapid orthodontic treatment
- An untreated cavity or a chronic dental abscess
According to the American Association of Endodontics, the location of trauma (or damage to the tooth) and its supporting structures determine the type of resorption.
How Does a Dentist Diagnose Tooth Resorption?
X-rays like bitewings or periapical radiographs can be used to diagnose tooth resorption. Sometimes it’s difficult to determine the type of resorption, which is important in determining the best type of treatment. In these cases, a 3D Cone Beam X-ray can better visualize the condition.
A dentist could also diagnose tooth resorption through a clinical exam. This may include a visual inspection or both a visual and an endodontic examination.
Pulp exams may be used during your visit. This exam uses hot and cold temperature changes to examine the tooth.
What are the Symptoms of Tooth Resorption?
Many people don’t report pain when first diagnosed with tooth resorption. However, this depends on the severity and the location of the resorption.
For example, some people notice sensitivity if the resorption is near the root surface. Other common symptoms include:
- Brittle and loose teeth
- Holes in the teeth
- Unusual spaces between teeth
- Gum inflammation
- Pain all around the tooth or root
Most people are completely unaware that they have tooth resorption until it becomes a severe condition. Resorption is usually diagnosed during a routine X-ray when dark spots are found around the tooth root.
How to Manage Tooth Resorption
Tooth resorption is managed by preserving the affected parts of the tooth. If an external factor causes resorption, it will have to be removed. This can include a night guard or an orthodontic appliance.
Depending on the severity of resorption, several types of dental treatment are available to preserve the tooth, including:
Root Canal Treatment
Endodontists can place calcium hydroxide for younger teeth with immature roots to limit the amount of root resorption. The goal is to stop the progression of root resorption and allow it to continue to form normally.
Gum Surgery
If the root is completely formed, a surgical endodontic procedure is usually required to remove harmful, damaged cells so the resorption does not continue.
Dentists sometimes perform small surgeries to remove the damaged cells in teeth that show early resorption. A root canal and crown can help preserve the natural tooth for more severe cases.
Tooth Extraction and Dental Implant
In cases of severe root resorption, the tooth may need to be extracted and replaced with a dental implant. This is the most effective way to restore the function and aesthetics of the affected tooth.
How Can You Prevent Tooth Resorption?
To prevent tooth resorption, you must do the following:
- Brush and floss regularly
- Maintain a healthy diet to avoid tooth decay
- If you play any contact sports, wear a mouthguard to prevent trauma
- If you grind your teeth, talk to your dentist about a night guard to help protect the teeth from damage
- Visit your dentist for routine visits, so X-rays and proper clinical examinations can be performed
Early diagnosis of tooth resorption can help avoid long-term dental problems. If your dentist notices any signs of tooth resorption, they may want to see you sooner for follow-ups and monitor the tooth for any changes.
Sources
- “Glossary of Endodontic Terms, 10th edition.” American Association of Endodontists.
- Consolaro, A. “External Cervical Resorption: Diagnostic and Treatment Tips.” Dental Press
- Dindaroğlu, F, and Doğan, S. “Root Resorption in Orthodontics.” Turkish Journal of Orthodontics, Turkish Orthodontic Society, 2016.
- Heboyan A, Avetisyan A, Karobari MI, et al. “Tooth root resorption: A review.” Science Progress, 2022.
- Aidos et al. “Root Resorption Classifications: A Narrative Review and a Clinical Aid Proposal for Routine Assessment.” Eur Endod J, 2018.
- Thomas et al. “An insight into internal resorption.” ISRN Dent, 2014.

UCLA-trained dentist practicing in public health. Focuses on whole-body approach to dental care.
Related Articles

How to Brush Your Teeth Properly
Find out how to properly brush your teeth with a manual or electric toothbrush. You will also learn common toothbrushing...

Why Do I Wake Up With a Dry Mouth? Causes and How to Stop It
If you're experiencing dry mouth at night, you're not alone. This article covers the causes of dry mouth at night, treat...

The Best Tongue Scrapers for Fresher Breath & Improved Health
A tongue scraper is an oral hygiene tool that cleans your tongue. Read on to learn about its benefits, how to use it, an...

White Spots on Tongue: 7 Causes, What They Look Like, and When to Worry
White spots on your tongue most often come from oral thrush, leukoplakia, or geographic tongue. See what each cause look...
