What is an Open Bite?
Reader-supported. We may earn a commission from links on this page. Advertising disclosure.
In this article
What is an Open Bite?
An open bite is a rare type of malocclusion (misalignment) that affects less than 20 percent of the U.S. population.
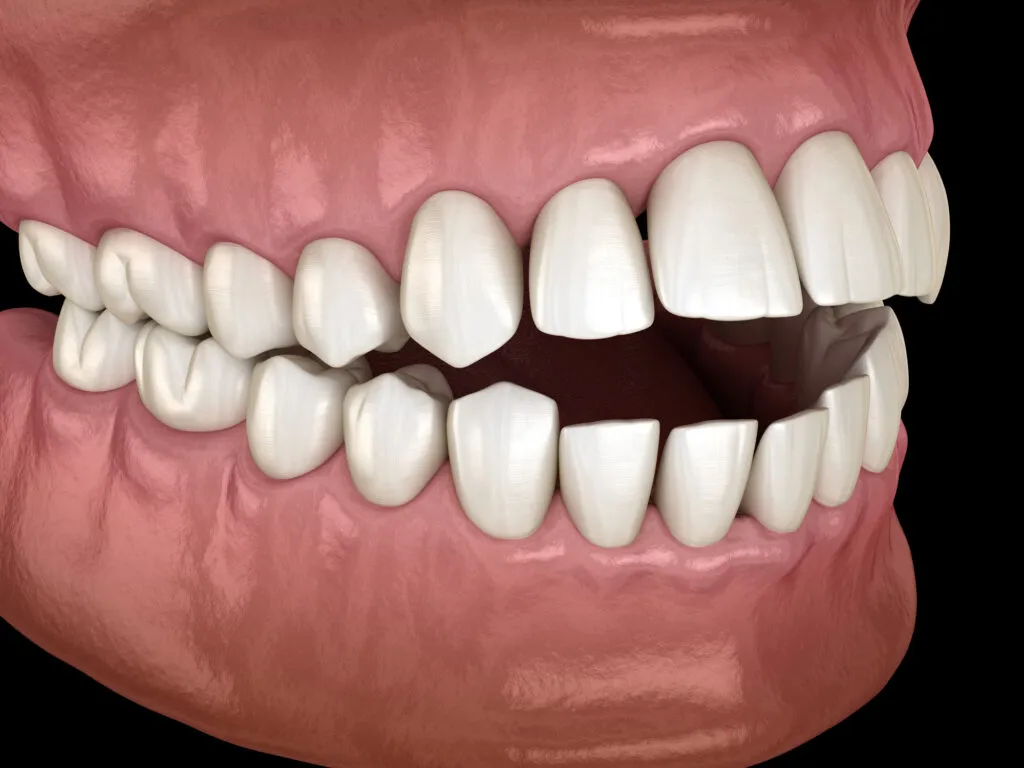
This misalignment occurs when the upper and lower front teeth slant outwards and do not touch when the mouth is closed. It can develop in the front of the mouth (anterior) or the back of the mouth (posterior).
Straighten your teeth at a fraction of the cost. Learn about clear aligners.
Causes of an Open Bite
The underlying causes of an open bite primarily involve skeletal or dental factors, such as:
Genetics and Developmental Factors
Children can develop temporary open bites when the baby teeth fall out and the permanent teeth start to erupt. This type of open bite usually resolves without treatment.
However, more complex open bites may occur if the child inherits skeletal abnormalities that affect jaw growth. Genetic factors that prevent the teeth from fully erupting can also cause problems.
Dental Habits and Behavioral Factors
If an open bite is not caused by genetics, it can be due to poor oral habits. Behaviors and dental habits that can lead to an open bite include:
- Thumb sucking
- Sucking the lower lip
- Mouth breathing
- Excessive pacifier and bottle use
- Tongue thrusting (pushing the tongue against the front teeth)
Babies have an instinct to suck, but they should stop by age 2 or 3. If a child developed this form of malocclusion due to excessive thumb or finger sucking, the condition can still be reversed if the child’s permanent teeth have not grown in yet and skeletal growth is not complete.
Jaw Injuries
Traumatic injuries that cause jaw misalignment can lead to various types of bite malocclusion, including an open bite.
Types of Open Bite
An open bite can describe various types of malocclusion. Open bites are categorized based on their location and cause.
Different types of open bite include:
Anterior Open Bite
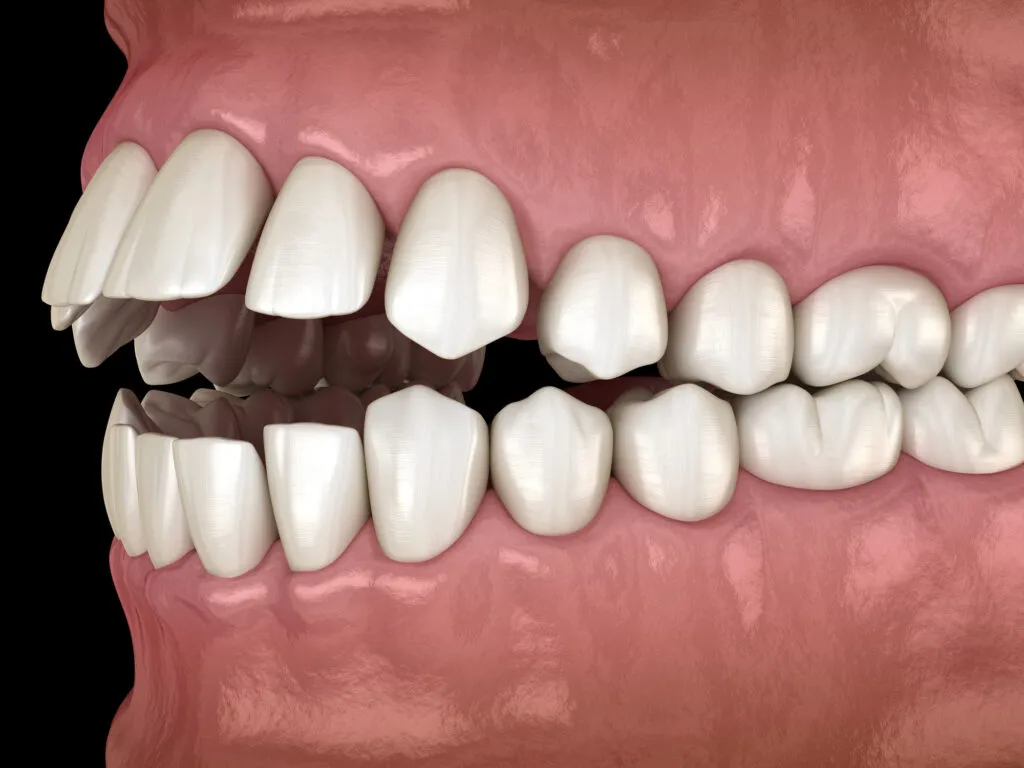
An anterior open bite occurs when the upper and lower jaws’ incisors (front teeth) do not overlap.
It can affect all front teeth or just a few teeth. Treatment is typically necessary because you may be unable to tear food with your front teeth. Speaking may also be difficult.
Treatment can help reduce speech problems, but it is not guaranteed. This is because speech is established in early childhood, and it may not be possible if the permanent teeth have already grown in.
Posterior Open Bite
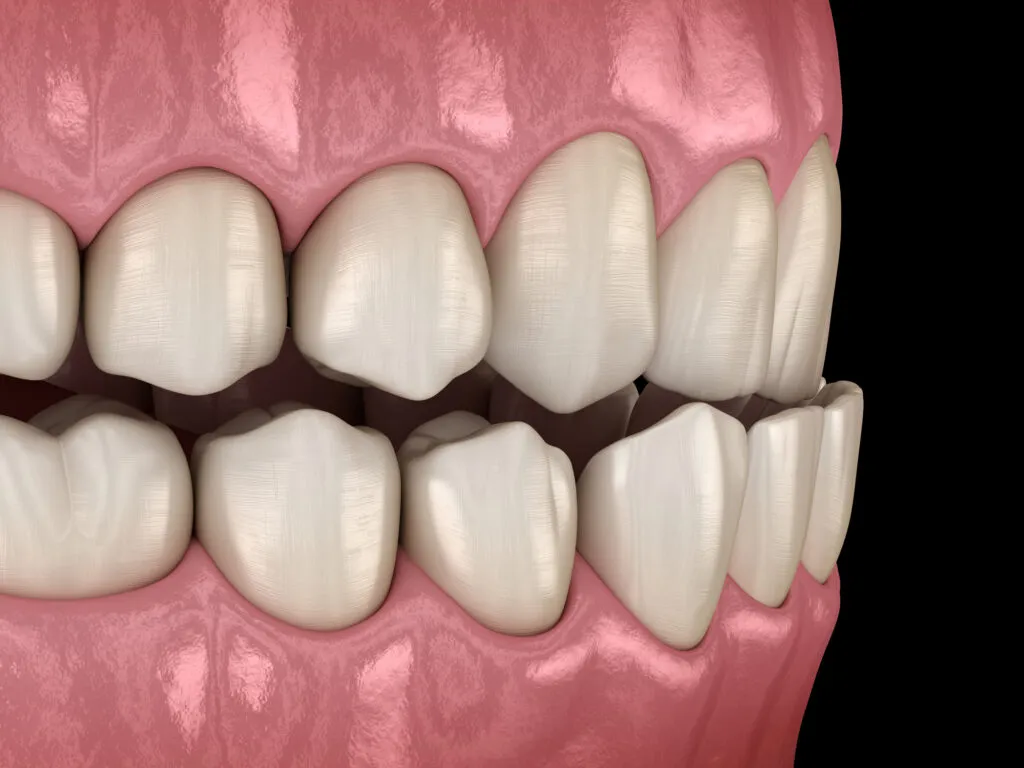
A posterior open bite is the opposite of an anterior open bite. It occurs when the back teeth, including the molars and premolars, do not touch when in occlusion (biting down).
In a normal bite, the back teeth in the upper jaw should be positioned slightly on the outside of the teeth in the lower jaw.
Treatment is usually necessary because patients cannot chew properly.
Dental vs. Skeletal Open Bite
A dental open bite results from a tooth eruption impediment, while a skeletal open bite is due to abnormal facial growth (genetics).
This may include irregular development of the molars or jawbones that grow away from each other.
Find the best at-home clear aligners for mild misalignment. See our expert recommendations.
Why Is it Important to Treat an Open Bite?
Though some childhood open bites resolve without treatment, other types of malocclusion won’t go away on their own. If an open bite remains uncorrected, it can cause additional problems, such as:
- Trouble swallowing
- Pain and difficulty biting and chewing food
- Speech problems
- Esthetic concerns
Schedule a dental appointment if you think you or your child has an open bite. Your dentist will provide an accurate diagnosis and recommend the most effective treatment.
Open Bite Treatment
There are many options for treating an open bite. Depending on the person’s age and the type of open bite, treatment options may include:
- Behavioral changes
- Orthodontic treatment
- Jaw surgery
Behavior Modification
Many children have open bites during the primary and mixed dentition phase, which is when baby teeth are falling out, and permanent teeth begin to grow in. This type of malocclusion may self-correct to a normal bite.
However, treatment requires addressing oral habits like thumb-sucking early enough for the jaw and permanent teeth to develop normally.
Orthodontic Treatments
Several orthodontic treatments can correct an open bite, including:
High Pull Headgear
High pull headgear attaches to the top of the head, back of the head, and upper jaw.
The appliance controls jaw growth and improves teeth alignment. Headgear is used in combination with braces.

Clear Aligners
Clear aligners, such as Invisalign, can be effective only in treating minor anterior open bites.
Vertical Chin Cup
A vertical chin cup is a common orthopedic appliance used to correct an open bite. The appliance controls the growth of the lower part of the face and prevents the chin from growing backward or downward.
Roller Appliance
Roller appliances help prevent tongue thrusting against the front teeth. Tongue thrusting can encourage an open bite and upper front teeth protrusion (overjet).
The appliance consists of a small roller-type bead that strengthens the tongue muscles and is connected to two braces on the molars in the upper jaw.
Bite Block
Bite blocks can be placed on the two back molars in the lower jaw (both sides) to slowly correct an anterior open bite. The appliance moves the teeth back over time and removes the space between the upper and lower teeth.
Jaw Surgery (Orthognathic Surgery)
Surgical treatment is typically necessary for adults with skeletal open bites. This is because their jaw and teeth are fully developed.
Children may also require jaw surgery if their permanent teeth are fully grown in, and the jaw is fully developed. During surgery, an oral surgeon correctly places the patient’s upper and lower jaws. Then plates and screws are inserted to keep the jaws in the correct position.
Straighten your teeth conveniently at home. Compare the best clear aligner brands.
What is the Prognosis for an Open Bite?
Treatment to correct an open bite can be successful at any age. However, treatment is simpler and less involved before the permanent teeth grow in.
Children should have a dental evaluation while some baby teeth remain as early as 7 years of age. Early behavior intervention can help prevent an open bite as children’s jaws develop.
Treating an open bite in adults is more complex. In these cases, behavioral and orthodontic treatments may be necessary. For some, jaw surgery may be needed.
Sources
- Cobourne, Martyn T., and Andrew T. DiBiase. Handbook of Orthodontics E-Book. Elsevier, 2015.
- Recognizing and Correcting Developing Malocclusions: a Problem-Oriented Approaches to Orthodontics. Wiley, 2015.
- Rohit, Kulshrestha. “Open Bite Malocclusion: An Overview.” Journal of Oral Health and Craniofacial Science, 2018.
- “7 Common Bite Problems in Children and Adults.” American Association of Orthodontists, 2019.
- Ngan, P., and Fields, HW. “Open bite: a review of etiology and management.” Pediatric Dentistry, 1997.
- Cambiano, AO., et al. “Nonsurgical treatment and stability of an adult with a severe anterior open-bite malocclusion.” Journal of Orthodontic Science, 2018.

UCLA-trained dentist practicing in public health. Focuses on whole-body approach to dental care.
Related Articles

Crossbite: Types, Causes, Complications & Treatment
Crossbites can cause a variety of problems. This article discusses what it is, the different types, causes, complication...
Types of Underbites: Causes, Risk Factors & Treatment Options
An underbite occurs when the lower jawbone protrudes over the upper jaw. Learn more about its types, causes, complicatio...
Crowded Teeth: Causes, Treatment & Risks
Crowded teeth can cause a number of problems. Learn about the causes, treatment, and risks of untreated dental crowding.
Overbite Treatment: 5 Options You Should Consider
An overbite is a common dental condition that can cause aesthetic and functional problems. If you're looking for overbit...
