What Oral Thrush Looks Like, Symptoms & How to Treat it
Reader-supported. We may earn a commission from links on this page. Advertising disclosure.
In this article
What is Oral Thrush?
Oral thrush, or oral candidiasis, is a yeast infection in the mouth. The most common type of fungus that causes oral thrush is Candida albicans. These fungi live in the mucous membranes lining the mouth.
Most people have slight traces of Candida in their mouths. In some cases, the fungi can overgrow and cause thrush. Thrush is difficult to notice, at least initially, and does not cause severe pain. In most cases, thrush does not indicate a serious medical problem, though it can affect the quality of life.
Candidiasis most commonly affects people with weakened immune systems, such as infants or adults taking certain medications. However, the condition can affect people of all ages.
What Does Thrush Look Like?
Oral thrush looks like white spots or lesions on the tongue, palate, or buccal mucosa (lining of the cheek and back of the lips). Lesions associated with oral thrush often have a consistency similar to cottage cheese.
When you wipe the lesions away, they leave a red, raw base. Doing this can also cause minor bleeding. Oral thrush can also cause a mild burning sensation.
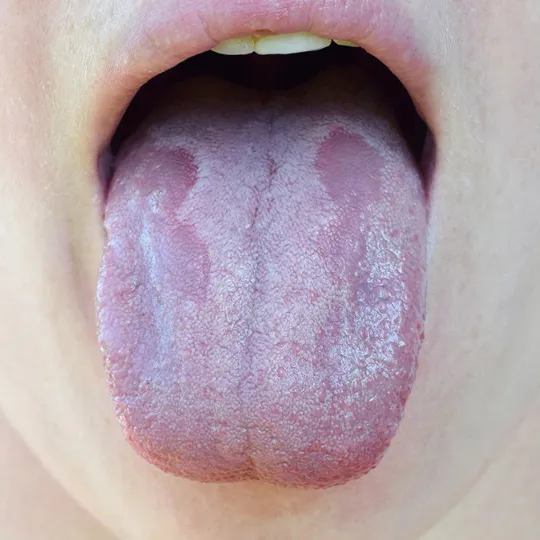
Symptoms of Oral Thrush
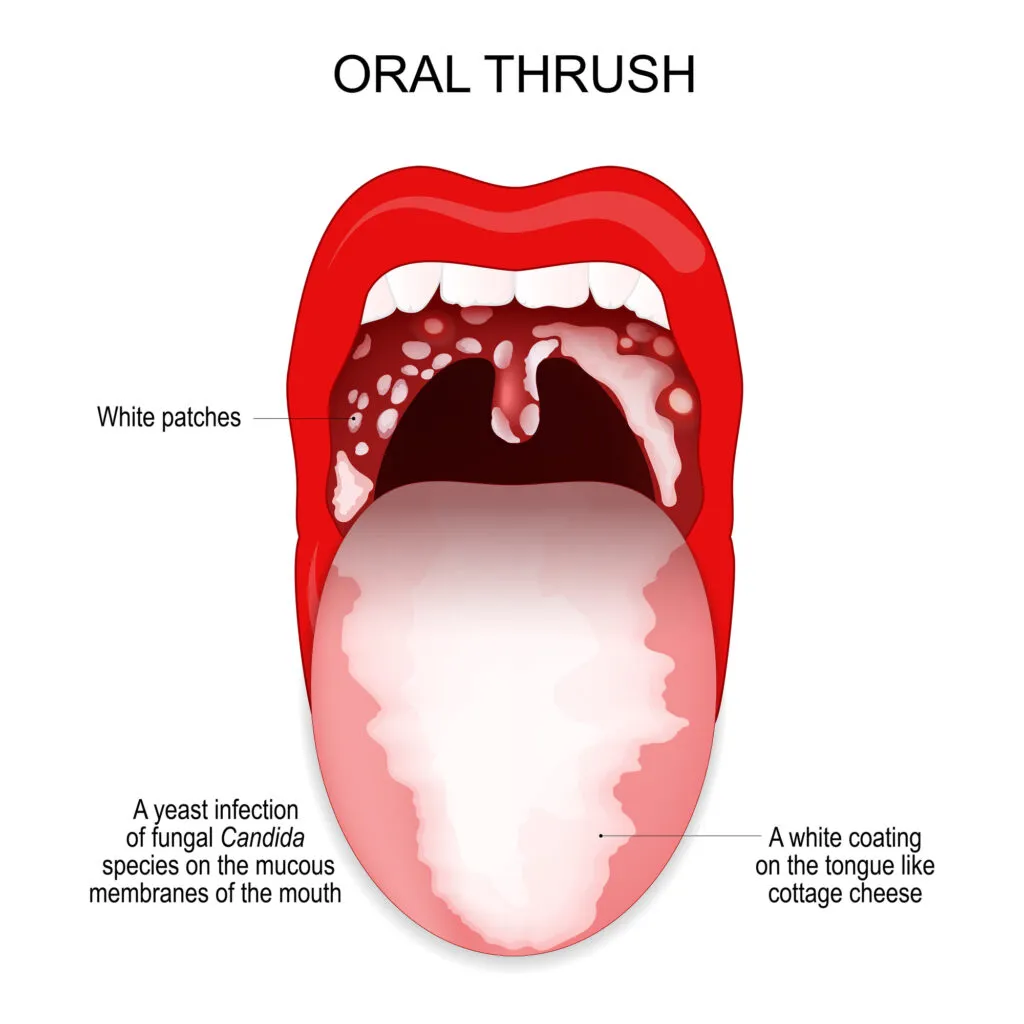
Oral thrush can cause the following symptoms:
- White patches or lesions on the tongue, palate, cheeks, or inner lips
- Sore mouth, lips, cheeks, tongue, or throat
- Redness around the lesions
- Dry or cracked lips
- Decreased sense of taste
- A burning sensation around the lesions
- Cottonmouth or dry mouth
- Reduced ability to swallow, speak, and eat
What Causes Oral Thrush?
Various factors can trigger oral flush, including existing medical conditions and poor oral health. The following are common causes of oral thrush:
Antibiotics
Because antibiotics can alter the balance of microorganisms in the mouth, anybody taking antibiotics may develop thrush symptoms.
According to Dr. Khushbu Aggarwal, NewMouth’s in-house dentist, “Antibiotics, although necessary, can upset the delicate balance of the microorganisms in your body. Make sure to take antibiotics with a probiotic such as yogurt.”
Dry Mouth
Dry mouth is an oral condition that occurs when the salivary glands in the mouth do not produce enough saliva. Inadequate saliva production increases the risk of oral thrush.
Poor Oral Hygiene
Using an old toothbrush with harbored fungus can cause thrush. Switching toothbrushes or toothbrush tips at least every three months is recommended to prevent the spread of bacteria and fungus.
“A good rule of thumb is to switch out your toothbrush once the bristles start to splay or after you have gotten over a sickness like the common cold,” says Dr. Aggarwal.
HSV-1 Infection
Herpes simplex virus type 1 (HSV-1) is a highly contagious infection that causes cold sores and may also cause mild candidiasis. HSV-1 is a lifelong disease that spreads through close personal contact, such as kissing and sharing utensils.
Cancer Treatment
Oral thrush is the most common fungal infection cancer patients get while receiving treatment. Cancer treatments weaken the immune system, which can trigger the overgrowth of Candida fungus.
Pregnancy
Pregnant women are at a higher risk of developing oral candidiasis due to extreme hormonal changes and a weakened immune system, especially during the third trimester.
Steroids
According to Dr. Aggarwal, steroids compromise the immune system. Using steroid medications long-term can cause thrush flush. If you frequently use an asthma inhaler with steroids, you have an increased risk of developing oral candidiasis.
Bottles and Pacifiers
Pacifiers and baby bottles can make a baby’s mouth too moist, creating an ideal environment for yeast to multiply. Babies should not sleep with a bottle or a pacifier in their mouths.
Thoroughly clean pacifiers and bottle nipples in the dishwasher or soak them in hot water after each use to remove bacteria and fungus.
The American Academy of Pediatrics recommends stopping pacifier use altogether after a baby turns six months old to prevent thrush and other oral conditions such as bite changes.
Uncontrolled Diabetes
High levels of glucose make it easier for Candida fungus to grow. More specifically, people with diabetes who do not monitor their blood sugar accurately have a higher risk of developing yeast infections.
Weakened Immune Systems
People who have diabetes, HIV/AIDS, or take steroid medications are also at risk of developing thrush. In these cases, thrush can be life-threatening since the body is not strong enough to fight it off.
Oral Thrush Treatments
Thrush is a non-life-threatening infection. With proper treatment, it typically goes away within a few days to two weeks. If it doesn’t resolve within this timeframe, contact your general dentist.
The first line of treatment for oral thrush is topical medications. If these are not effective, then additional medication may be necessary.
Treatments may include:
1. Antifungal Medications
Antifungal medications kill fungi inside the mouth. Common medications used to treat thrush include miconazole, clotrimazole, nystatin, itraconazole, and fluconazole. They may come as a tablet, a mouth rinse, or a lozenge.
2. Antiseptics
Antiseptic medications prevent the growth of Candida fungus while also killing harmful bacteria in your mouth. Paroex mouthwash, for example, is an effective treatment for oral candidiasis.
3. Dietary Supplements
Doctors may prescribe probiotics to support the growth of “healthy” bacteria. Eating unsweetened yogurt can also reduce the symptoms and discomfort of candida infections.
While more research is necessary to determine specific strains of probiotics that help with oral thrush, the general theory is that live cultures help improve the condition.
4. Throat Lozenges
If oral thrush causes a sore throat, throat lozenges (cough drops) can relieve discomfort. These medications can be bought directly at a drugstore without a prescription. They are also relatively inexpensive.
How Do You Prevent Oral Thrush?
The best way to prevent thrush is to practice good oral hygiene.
Children and adults should:
- Brush their teeth with fluoride toothpaste twice a day
- Floss once a day
- Use mouthwash regularly
- Clean oral appliances, such as retainers or dentures, regularly
Every six months, you should also visit a dentist for teeth cleanings.
Oral Thrush in Babies and Children
Babies and children are susceptible to developing candidiasis because they have decreased immunity. Infants are most vulnerable to developing thrush in their first year of life.
Young children are more likely to develop the condition if they:
- Have taken antibiotics due to illnesses
- Do not clean orthodontic appliances before use
- Use an inhaler for asthma
- Have a weaker immune system than most children
- Frequently use a pacifier (babies)
- Were born prematurely and had a low birth weight
If a mother has a vaginal yeast infection while giving birth, the baby can contract oral thrush during vaginal delivery.
What Oral Thrush Looks Like: Symptoms & How to Treat it
NewMouth PodcastSources
- “Candidiasis Basics.” Centers for Disease Control and Prevention, 2021.
- Nowak, Arthur J. “Pediatric Dentistry: Infancy through Adolescence.” Elsevier, 2019.
- “Oral thrush: Overview.” Cologne, Germany: Institute for Quality and Efficiency in Health Care (IQWiG); 2006.
- “Thrush (Oral Candida Infection) in Children.” Health Encyclopedia – University of Rochester Medical Center.

UCLA-trained dentist practicing in public health. Focuses on whole-body approach to dental care.
Related Articles

What Are Canker Sores?
Are you struggling with canker sores? Here's everything you need to know about these pesky mouth ulcers, including how t...

Why Is My Tongue Itchy?
Find out why your tongue might be feeling itchy and what you can do about it. You will find the causes and home remedies...
What Is Burning Mouth Syndrome?
Burning mouth syndrome (BMS) is a complex condition. Here's what you need to know about it, including the symptoms, caus...

The Effects of Food on Dental Hygiene and Health
Learn how your overall health affects your oral health through nutrition, medications, medical conditions, and more. We...
