Why Do Teeth Turn Black?
Reader-supported. We may earn a commission from links on this page. Advertising disclosure.
In this article
Noticing a dark spot on your tooth can feel unsettling, especially when you can’t tell whether it’s a simple stain or something more serious.
Most black discoloration falls into two broad categories: surface stains that sit on the enamel and deeper changes that start inside the tooth. Because these two categories behave differently, the right treatment depends on confirming what type of discoloration you have.
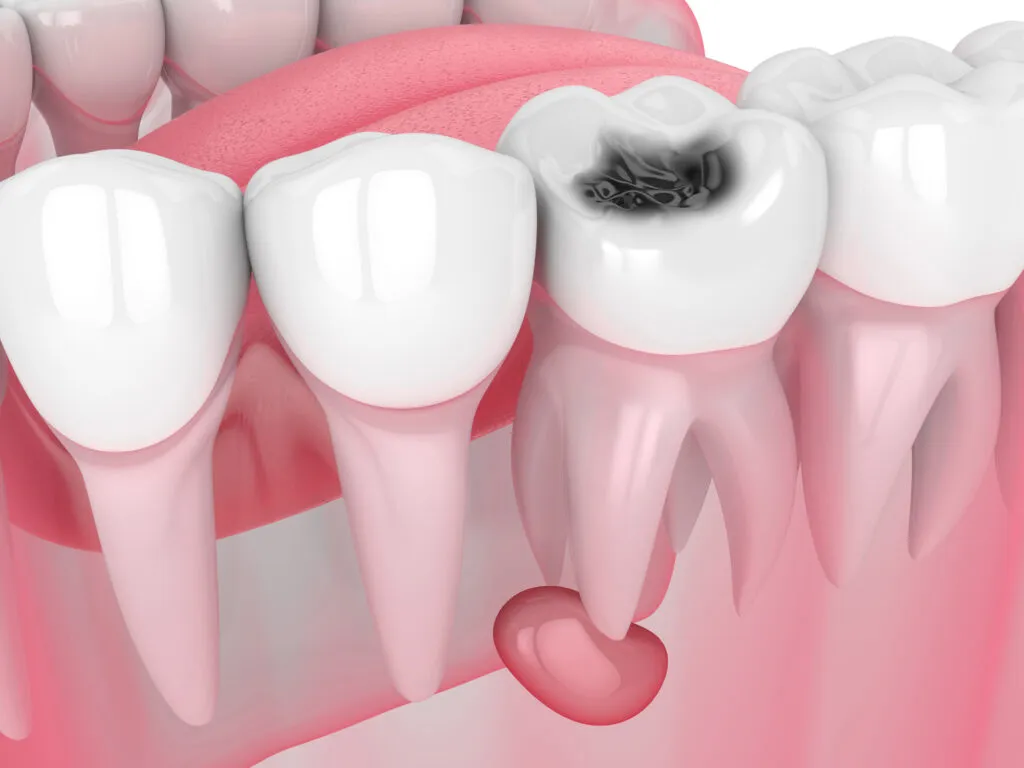
Some stains look dramatic but are harmless, while others signal decay or changes in the pulp that need timely care. Even so, any new discoloration should be checked so a dentist can confirm whether it’s a stain or something that requires treatment.
Extrinsic Causes of Black Teeth and Their Fixes
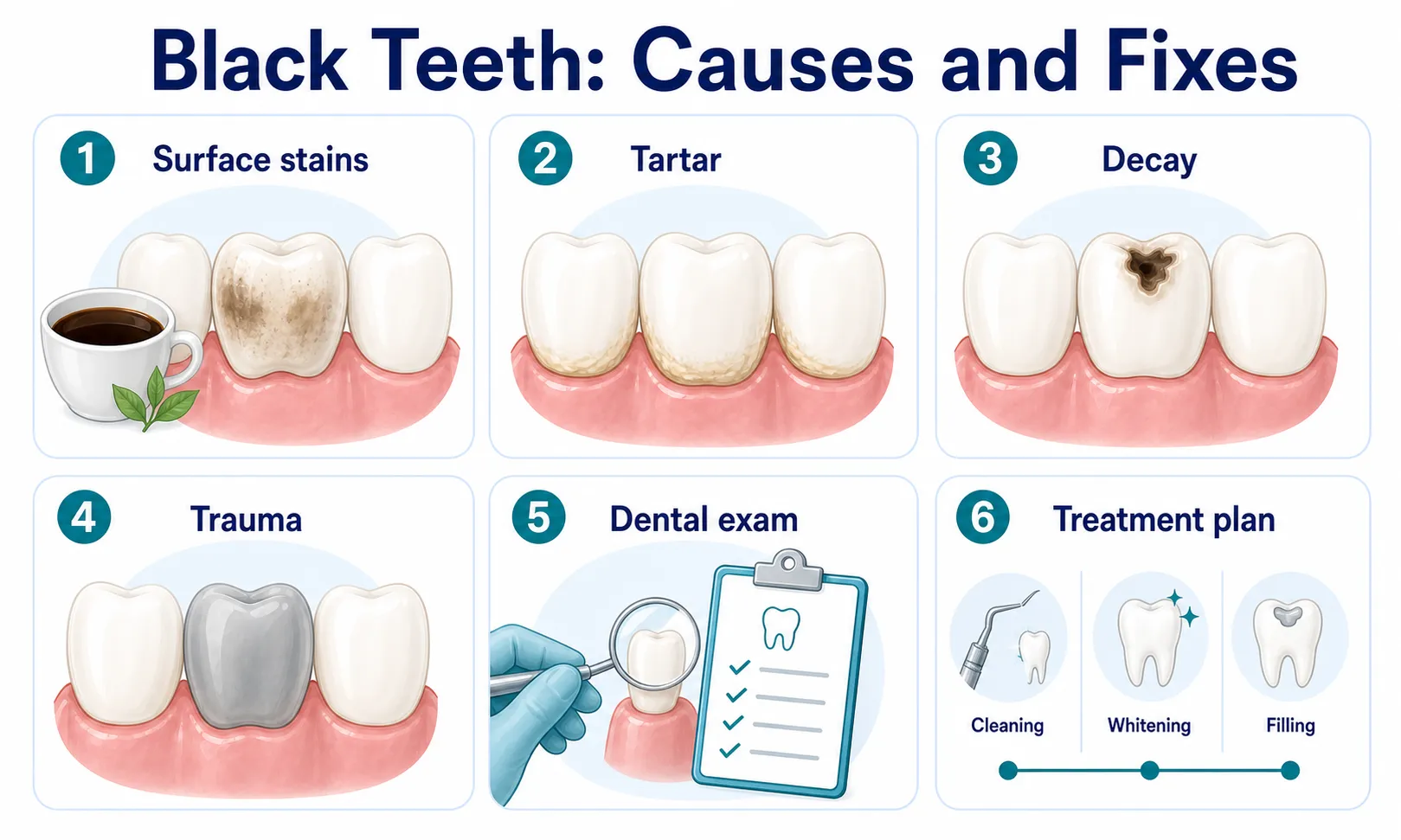 Black stains that form on the outside of the tooth come from surface deposits, foods, drinks, or certain products. These stains sit on the enamel rather than inside the tooth, making them easier to remove with professional care.
Black stains that form on the outside of the tooth come from surface deposits, foods, drinks, or certain products. These stains sit on the enamel rather than inside the tooth, making them easier to remove with professional care.
Surface deposits can look dramatic, but they do not weaken the tooth, and most can be removed with cleaning or polishing.
Dentists start with the least invasive option, then use more focused techniques if the stain is stubborn. Common fixes for extrinsic stains include:
- Professional scaling — To remove hard deposits along the gumline that normal brushing cannot reach.
- Polishing or microabrasion — When stains remain after cleaning and need gentle smoothing of the outer surface.
- Chemical whitening — For lingering surface discoloration that requires peroxide-based treatment under supervision.
- Avoiding charcoal products — Because abrasive powders can wear enamel and make sensitivity worse.
- Reviewing medications — Things like liquid iron supplements may darken specific teeth and need special hygiene support.
Once the stain is removed, a dentist can explain how often you may need maintenance cleanings, especially if the stain tends to return.> Get your brightest smile with NewMouth’s top teeth whitening picks for 2026.
Intrinsic Causes of Black Teeth
Black discoloration within the tooth usually signals decay, trauma, or changes in the pulp. These issues affect deeper layers of the tooth, so surface cleaning or whitening won’t fix the color.
- Cavities and decay — Decay creates soft, darkened spots that need to be removed before the tooth can be rebuilt.
- Pulp problems — A tooth that has turned gray or darker overall may have nerve damage, often from trauma or deep decay.
- Developmental stains — Some stains form when tooth enamel develops, such as fluorosis or tetracycline staining.
Treatment focuses on restoring the tooth’s health first, then improving its appearance if needed. This sequence matters because addressing infection or decay early prevents pain and protects the surrounding bone.
When discoloration is internal, dentists choose the least invasive option that keeps the tooth strong and comfortable. Treatment options for intrinsic discoloration include:
- Fillings — To remove decayed, soft areas and rebuild the tooth with a strong, tooth-colored material.
- Root canal treatment — When the pulp is dead or infected, and it needs to be cleaned and sealed from the inside.
- Internal bleaching — Once the tooth is healthy, using a safe, sealed technique to lighten discoloration after root canal therapy.
- Veneers or crowns — To mask deep stains or restore weakened teeth when a color change is severe.
- Extraction — When the tooth is too damaged to be restored safely or predictably.
Your dentist will help you choose the most conservative treatment that addresses both the tooth’s health and its final appearance.
After treatment, your dentist will explain how to keep the restored tooth healthy and what follow-up visits are needed.
When Should You See a Dentist?
Black discoloration should always be evaluated, and certain symptoms mean you should go sooner. Stains from foods, drinks, or surface deposits rarely cause other problems, while decay or infection often causes sensitivity or pain.
A quick exam helps separate harmless discoloration from issues that need care, and it prevents delays if the tooth has deeper damage.
Before the list, here’s the practical rule: get prompt care if pain, swelling, or fever develops because these symptoms can signal a spreading infection that needs professional treatment.
See a dentist soon if you notice:
- Tooth or facial pain that lingers or worsens after eating or brushing.
- Swelling of the gums or face that makes the area feel tight or warm.
- Bleeding gums that appear red, tender, or bleed easily during brushing.
- Sensitivity to hot, cold, or sweet foods that feels sharper than normal.
- Pus or pockets forming around the gumline near a dark spot.
A dentist can quickly confirm the cause and guide your next steps so you know whether cleaning, whitening, or restorative care is the right fit.
How Do Dentists Diagnose Black Teeth?
Dentists diagnose black discoloration by looking at the pattern, checking the texture, and using X-rays or simple tests to evaluate the tooth.
These steps distinguish stain from decay and confirm whether the pulp inside the tooth is healthy. This matters because surface stains can be cleaned, while deeper issues need different treatments.
Your dentist will walk you through these methods:
- Visual pattern — Dentists look at the color and location of the spot, which helps separate a harmless surface line from decay or graying due to pulp changes.
- Tactile check — A sticky or soft texture suggests active decay, while a hard, firmly attached deposit points to a surface stain or an arrested lesion.
- Tests — X-rays reveal hidden decay, and a cold or electric test checks whether the tooth’s pulp is still alive.
A professional exam works because each cause has a recognizable pattern or response, which helps quickly and safely narrow down the right treatment.
Your dentist will explain what they see and why it suggests a stain, a cavity, or a pulp problem.> See NewMouth’s top 10 teeth whitening products of 2026.
Costs and Insurance for Black Teeth Treatment
Costs vary based on where you live, the materials used, and whether the procedure is cosmetic or medically necessary.
Preventive cleanings are usually covered well, while cosmetic treatments often are not. Restorative procedures related to decay or pulp problems typically fall into partially covered categories.
Insurance coverage depends on how the treatment is documented, so asking your dental team for a benefits estimate can help you plan.
How to Prevent Teeth Stains and Decay
Prevention works best when it matches the cause of the discoloration. Good oral hygiene stops decay, while lifestyle changes reduce new stains.
Some forms of black line stain can persist even with good home care, making regular cleanings especially helpful.
Here are ways to help prevent black discoloration:
- Brush with fluoride toothpaste twice a day to strengthen enamel and prevent decay.
- Clean between teeth daily to remove plaque in places a brush cannot reach.
- Limit staining foods and drinks like coffee, tea, and red wine if you notice frequent surface stains.
- Avoid charcoal products because coarse abrasives can wear enamel and increase sensitivity.
- Stay consistent with checkups so stains or early decay are caught before they worsen.
Your dentist can tailor prevention steps based on whether your staining is surface-level or tied to decay.
A dental exam is the best way to confirm what’s causing the discoloration and choose the simplest, safest treatment. With a clear diagnosis, your dentist can help you restore your smile’s health and color with confidence.
Sources
- Cleveland Clinic. “Tooth Discoloration: Causes & Treatment – Cleveland Clinic.” Cleveland Clinic, 2025. (Cleveland Clinic)
- Medical News Today. “Black teeth: Stains, other causes, and treatment – MedicalNewsToday.” Medical News Today, 2023. (Medical News Today)
- National Institute of Dental and Craniofacial Research. “Tooth Decay | NIDCR.” NIDCR, 2025. (NIDCR)
- National Institute of Dental and Craniofacial Research. “Oral Hygiene – National Institute of Dental and Craniofacial Research.” NIDCR, 2024. (NIDCR)
- Slayton et al. “Evidence-Based Clinical Practice Guideline on Nonrestorative Treatments for Caries Lesions – ADA.” ADA.org, 2018. (PubMed)

Board-certified general dentist specializing in patient education and preventive dentistry.
Related Articles

5 Stages of Cold Sores and What to Do
Cold sores are a type of viral infection that can cause painful blisters on the lips, mouth, or throat. Learn about the...

Periodontitis Treatment: 6 Options & Oral Hygiene Tips
Periodontitis is a serious form of gum disease that can lead to tooth loss. Here we cover the primary treatment options...

Deciduous (Baby Teeth) vs. Permanent Teeth
What are Deciduous Teeth? Deciduous teeth are the first set of teeth to erupt in the mouth. They eventually fall out, an...

Pulpitis - Types, Causes, Symptoms & Treatment
Pulpitis is the inflammation of the pulp tissue inside your tooth. This guide explains how pulpitis affects oral health...
