Types of Underbites: Causes, Risk Factors & Treatment Options
Reader-supported. We may earn a commission from links on this page. Advertising disclosure.
In this article
Although underbites may not seem like a serious problem, they are something that requires treatment. Without proper treatment, an underbite can lead to several dental problems in the future.
Understanding an underbite and its implications is the first step toward a healthy, confident smile. Let’s explore what an underbite is, how to spot one, and the treatment options available.
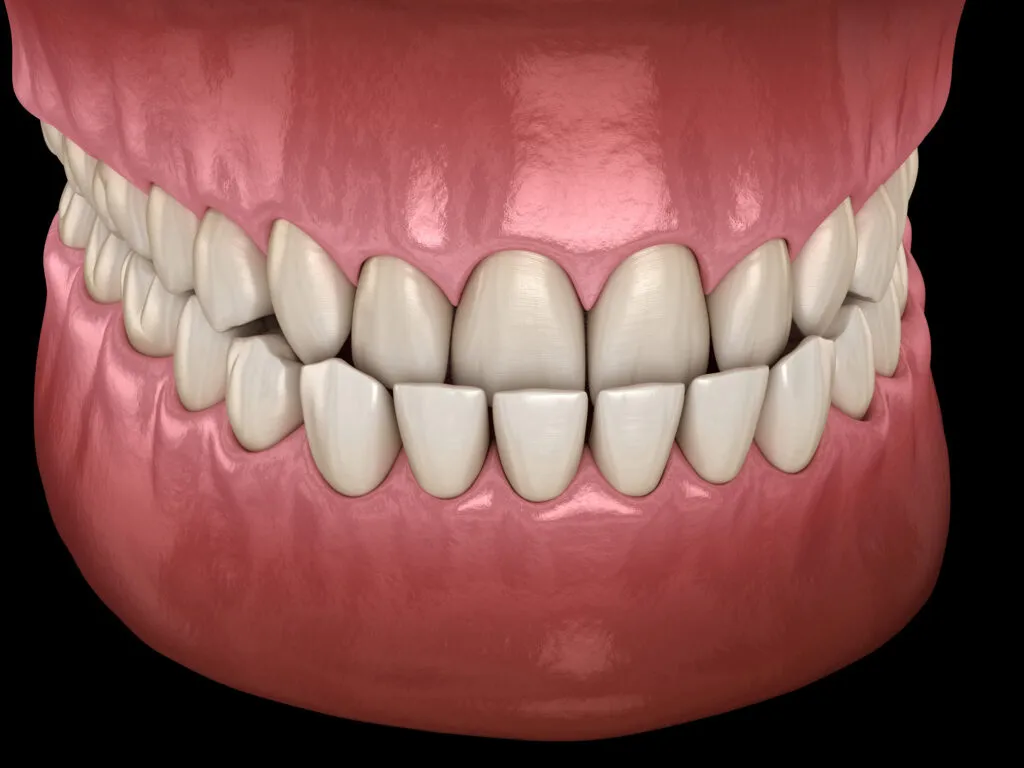
What is an Underbite?
An underbite is a class III orthodontic malocclusion where the lower jaw is pushed forward. In a normal bite, the front teeth should slightly overlap the lower teeth.
With an underbite, the lower front teeth and jaw are positioned in front of the upper front teeth and jaw. The condition can be mild or severe and requires orthodontic treatment.
What Are the Different Types of Underbites?
There are two types of underbites: a dental underbite and a skeletal underbite.
A dental underbite stems from teeth misalignment rather than the jawbone. That means the teeth are misaligned even if the jawbones are correctly positioned.
Meanwhile, a skeletal underbite is a genetic issue caused by jawbone deformity, such as an overdeveloped lower jaw or an underdeveloped upper jaw. This may require a more invasive form of treatment, such as jaw surgery.
Straighten your teeth at a fraction of the cost. Learn about clear aligners.
What Causes an Underbite?
The primary cause of underbites is genetics. If your parents or grandparents had an underbite, you’ll have a higher risk of getting it as well.
Additionally, some ethnic groups may have a higher tendency for jaw protrusion. Other causes include:
- Thumb sucking and pacifier use beyond 3 years old
- Drinking from a bottle long-term
- Jaw malformation
- Mouth breathing
- Injuries to the mouth
- Tumors
- Constant forward tongue pressure
- Crowding or abnormal tooth eruptions
- Tooth misalignment
Complications of Untreated Underbites
An underbite often leads to chewing difficulties, speech impediments, discomfort, and severe pain. Without proper treatment, it can increase your risk of dental problems, jaw problems, and even sleep apnea.
Other complications include:
- Increased risk of tooth decay
- Increased mouth breathing
- Temporomandibular joint disorders (TMD)
- Difficulties with swallowing
- Increased risk of gum disease
- Structural mouth and smile changes
- Irregular or crooked teeth
- Bad breath, even after brushing or rinsing with mouthwash
- Poor mental health and low self-esteem
- Increased need for invasive jaw surgery
- Headaches
- Earaches
- Cracked, damaged, or worn-down teeth
- Facial asymmetry
- Jaw joint inflammation or osteoarthritis
Find the best at-home clear aligners for mild misalignment. See our expert recommendations.
How are Underbites Treated?
If you’re concerned that your child may have a true underbite, consult a local orthodontist to discuss your options. Treatment for an underbite depends on the patient’s age and the severity of misalignment.
Underbite Treatment for Children
Some underbites form due to birth defects, such as a cleft lip and palate. The earlier you seek treatment for your child’s underbite, the less likely it is that surgery will be necessary later in life.
If a severe underbite isn’t noticeable or present at birth, orthodontists recommend waiting to start treatment until your child starts developing permanent teeth around 7 years old.
According to Dr. Nandita Lilly, one of NewMouth’s in-house dentists, “the correction methods used to treat an underbite are based on factors such as the extent of the underbite and the child’s age, so it is imperative to see your dental professional as early as possible so the child’s bones and palate can be more easily manipulated.”
Common underbite treatments for children include:
Underbite Treatment for Adults
If an underbite is not corrected in early childhood, it is more likely that other dental conditions and jaw issues will develop into adulthood.
Treatment is still possible for adults, but choices are limited since the jaw and teeth have fully developed. Depending on the patient, surgery is usually necessary at this stage of life.
Other treatment options for adults include:
- Dental braces
- Invisalign (clear aligners)
- Jaw surgery
How is the Severity of An Underbite Determined?
Orthodontic professionals often categorize underbites by severity:
- Mild — A subtle overlap that might not disrupt daily functions but could pose minor cosmetic worries.
- Moderate — The jaw misalignment is apparent, affecting chewing, speech, or comfort.
- Severe — Marked jaw protrusion, leading to significant challenges like chronic jaw pain or breathing difficulties.
Clinicians use visual exams, X-rays, and 3D imaging to determine how far the lower jaw is forward and whether the problem is caused by jaw structure, tooth alignment, or both.
When Should You See a Dentist?
If you start noticing symptoms like jaw pain, difficulty chewing, or speech problems, consider visiting an orthodontist or an oral and maxillofacial surgeon.
However, you should regularly visit the dentist to spot the early signs of underbites and other potential dental problems. This is especially true for kids around 7 years old or older.
Sources
- Cobourne, M., and DiBiase, A. “Handbook of Orthodontics.” Elsevier, 2016.
- “Orthodontic Treatment Options.” American Association of Orthodontists.
- Proffit et al. “Contemporary Orthodontics.” Elsevier/Mosby, 2019.
- Ghodasra, R. and Brizuela, M. “Orthodontics, Malocclusion.” Treasure Island (FL): StatPearls Publishing, 2023.
- Sterling, E. “Your Childs Teeth: a Complete Guide for Parents.” Johns Hopkins University Press, 2013.
- Zere et al. “Developing Class III malocclusions: challenges and solutions.” Clinical, Cosmetic and Investigational Dentistry, 2018.
- Lathrop-Marshall et al. “Orthognathic speech pathology: impacts of Class III malocclusion on speech.” European Journal of Orthodontics, 2022.

Board-certified general dentist specializing in patient education and preventive dentistry.
Related Articles

Underbite Correction for Children, Teens & Adults
Here's your complete guide on how to correct underbites for children, late teens, and adults. Learn about the various op...
Crowded Teeth: Causes, Treatment & Risks
Crowded teeth can cause a number of problems. Learn about the causes, treatment, and risks of untreated dental crowding.

Types of Diastema, Causes, and Treatment Options
A diastema is also known as gapped teeth. This article discusses the common type of diastema, its causes, treatment opti...

What Is a Deep Bite (Deep Overbite)?
A deep overbite occurs when there is an overlap between the upper and lower teeth. Here are its causes, treatment option...
