Types of Dental Implants: Procedure, Materials, and How They Work
Reader-supported. We may earn a commission from links on this page. Advertising disclosure.
In this article
What are Dental Implants?
A dental implant is an artificial tooth root surgically placed in your jawbone to support a replacement tooth.1 Implants are a long-term tooth replacement option after tooth loss or extraction.
More than 5 million dental implants are placed in the U.S. every year, and they have anchored successful dental restorations for more than 30 years.3
Quick Facts About Dental Implants
| Question | Answer |
|---|---|
| What are dental implants? | Artificial tooth roots — usually titanium — surgically placed in the jawbone to support replacement teeth.1,3 |
| What are the main types? | Single-tooth, implant-supported bridge, All-on-4, and 3-on-6 (by what they replace); endosteal, subperiosteal, and zygomatic (by how they are placed).2 |
| Which type is best? | Endosteal single-tooth implants are the most common. The right type for you depends on how many teeth are missing and how much jawbone you have.2,3 |
| How long do they last? | Implant bodies can last decades with proper care; the visible crown on top may need replacement sooner.8 |
Dental Implant Structure: How They Work
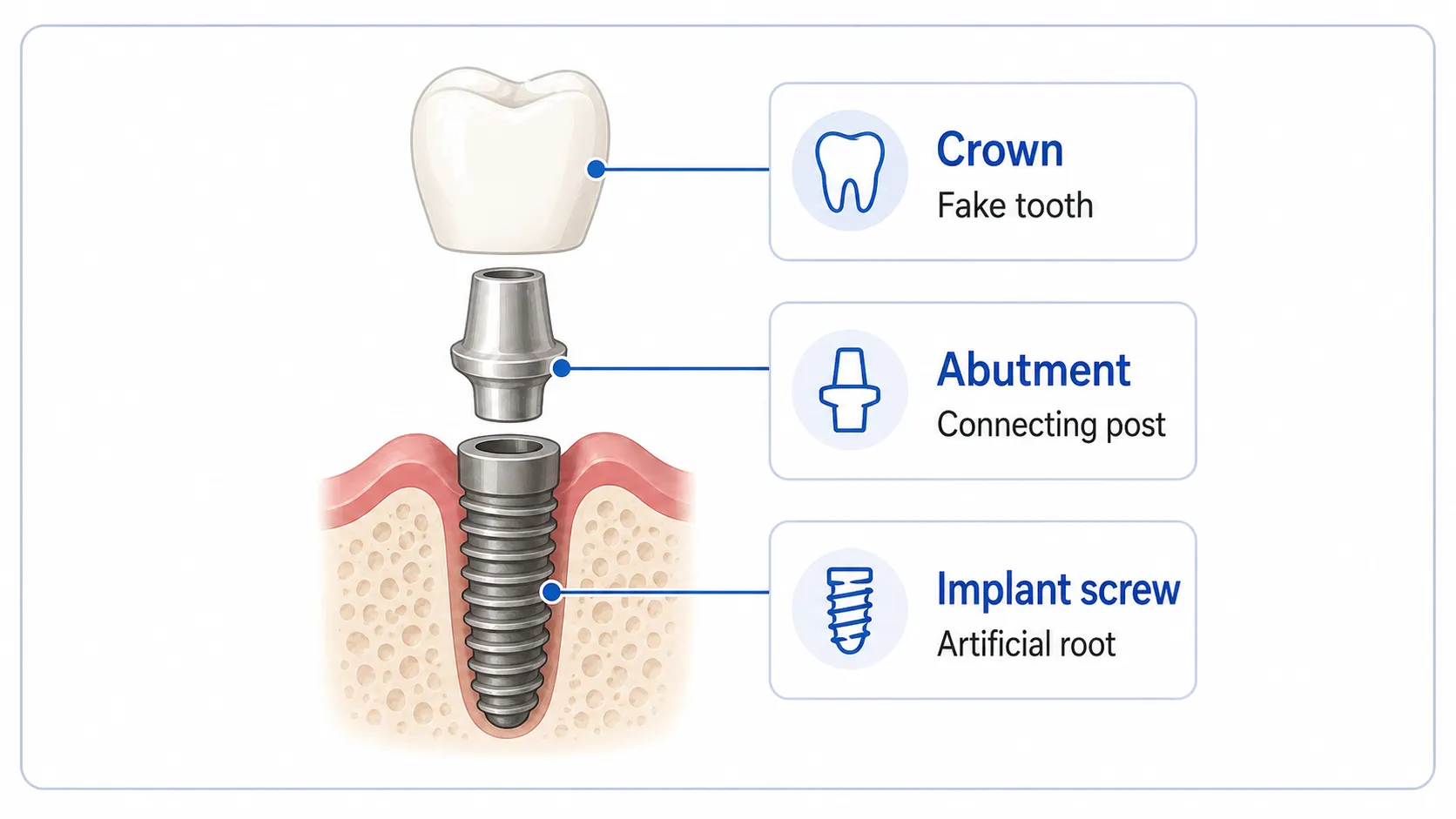
A dental implant has three parts that work together to replace the root and visible crown of a missing tooth:1,3
- The implant (or screw) serves as the tooth’s artificial root and integrates with your jawbone.
- The abutment is the connecting post between the implant screw and the crown.
- The crown is the visible “tooth” that sits on top of the abutment and matches the shape and color of your natural teeth.
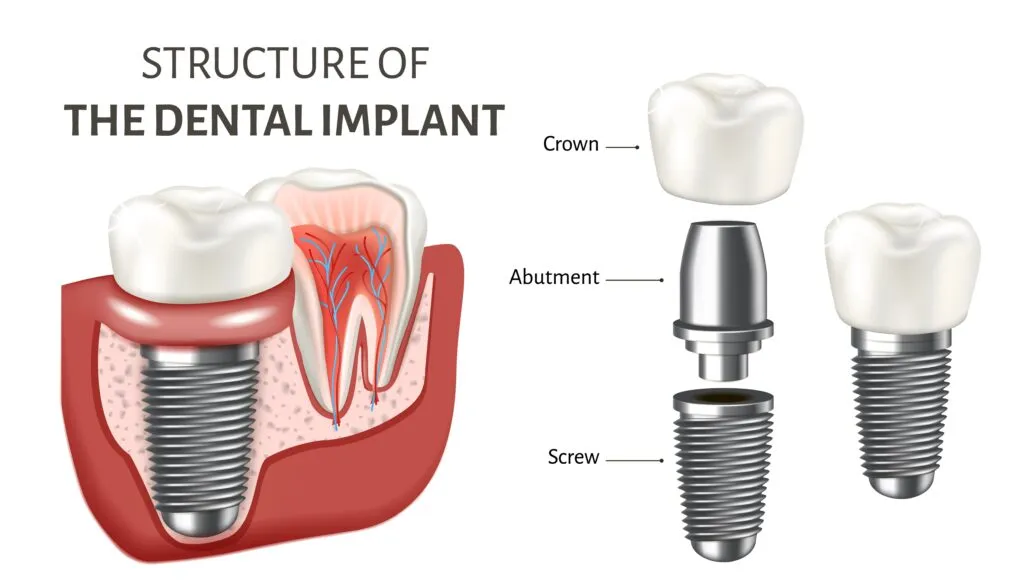
4 Types of Dental Implants
Implants are classified by what they replace (single tooth, bridge, full arch) and by how they are surgically placed (endosteal, subperiosteal, zygomatic).2 The four most common implant solutions, organized by what they replace, are:
1. Single Tooth Implant
A single dental implant replaces one missing tooth and is the right choice when neighboring teeth are healthy. It uses one implant screw, one abutment, and one crown.2,3
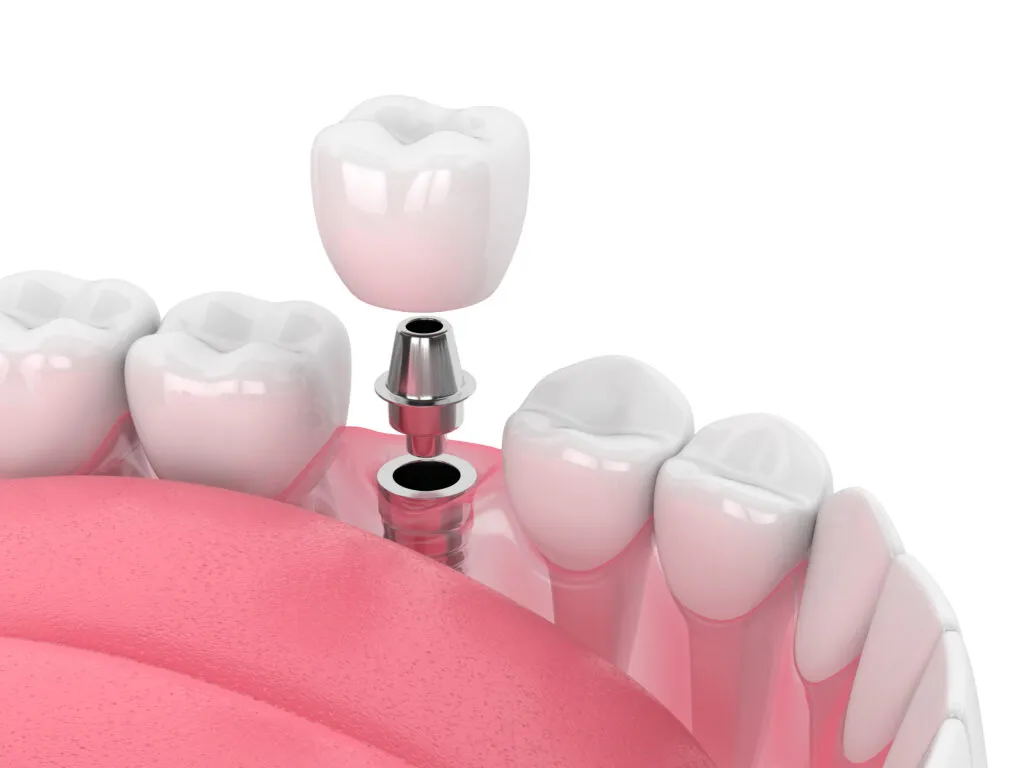
Single-tooth implants typically start in the low thousands per tooth. See the single-tooth implant cost breakdown for current ranges and what affects price.
2. Implant-Supported Bridge
Implant-supported bridges replace several adjacent missing teeth by anchoring a bridge to two or more implants instead of to natural teeth.2 Compare options with our bridge vs. implant guide.
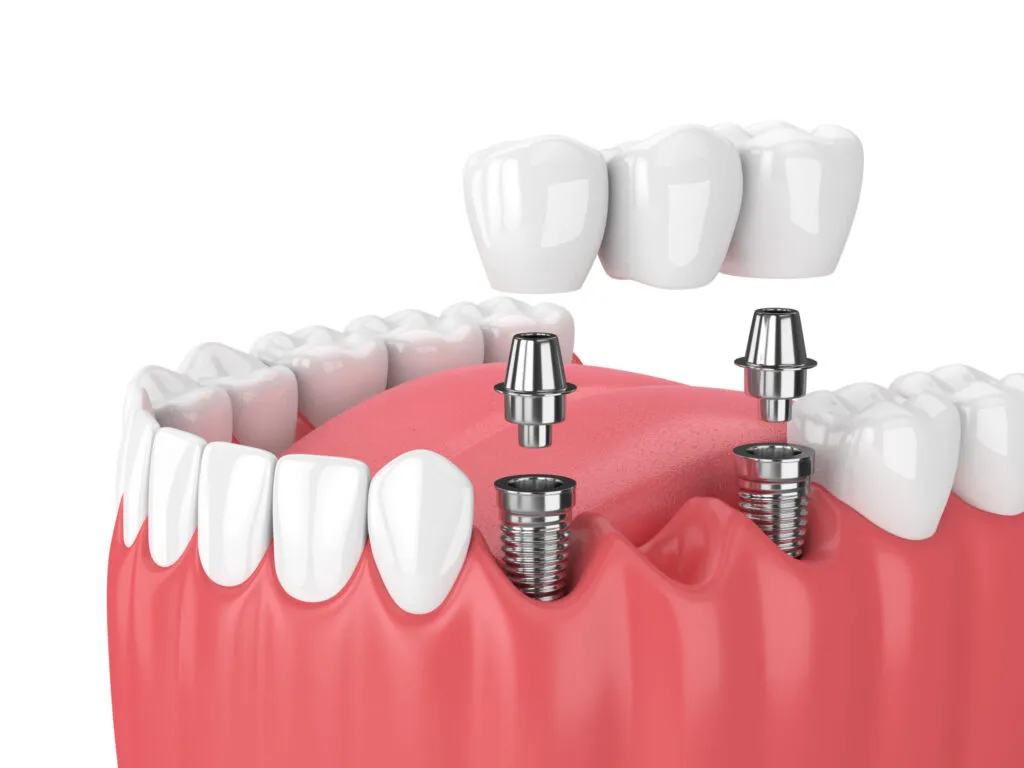
A fixed implant-supported bridge restores chewing and speech and keeps remaining teeth from drifting into the gap.
Implant-supported bridges sit in the mid range of implant pricing. See the bridge cost breakdown for current ranges and what is included.
3. All-on-4 Dental Implants
All-on-4 implants restore an entire upper or lower arch using four strategically placed implants to support a full set of teeth.2
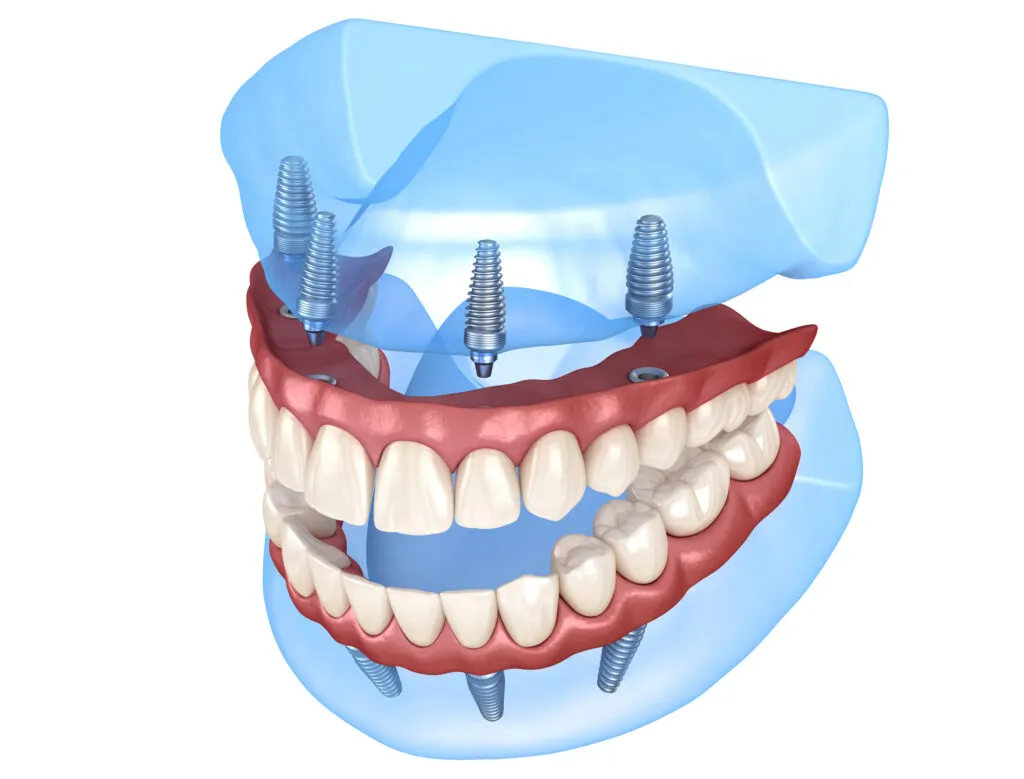
All-on-4 is a fixed full-arch restoration — your dentist screws it in, and only your dentist removes it for maintenance. Patient-removable implant-retained overdentures are a separate full-arch option that snaps on and off at home for cleaning.9 ClearChoice is one brand center that places All-on-4 implants.
All-on-4 is a higher-investment full-arch solution. See the All-on-4 cost breakdown for per-arch pricing and what affects it.
4. 3-on-6 Dental Implants
A 3-on-6 implant replaces a full arch using three individual bridges anchored to six implants. It is an alternative to an implant-retained denture for patients who want a fixed full-arch restoration.
3-on-6 implants are priced per arch. See the 3-on-6 cost breakdown for current ranges.
Dental Implant Techniques and Materials
Most modern implants are placed using one of three surgical approaches: endosteal (in the jawbone), subperiosteal (on the jawbone), or zygomatic (anchored in the cheekbone).2 Almost all implants are made from titanium because it bonds reliably with bone, though zirconia is sometimes used as a metal-free alternative.7
Endosteal Implant
Endosteal implants are the most common type used today. The titanium post is placed directly into the jawbone, where it bonds with surrounding bone over several months.1,2
Subperiosteal Implant
Subperiosteal implants rest on top of the jawbone, under the gum tissue, rather than inside the bone.2 They are uncommon today but remain an option for patients who do not have enough healthy jawbone for endosteal placement and prefer to avoid bone grafting.
Zygomatic Implant
Zygomatic implants anchor into the cheekbone (zygoma) instead of the upper jawbone. They are used for patients with severe upper-jaw bone loss who cannot support standard implants and want to avoid extensive grafting.2
Benefits of Dental Implants
Implants restore chewing and speech to near-natural function, preserve jawbone, and can keep working for decades with proper care.3,8
Here are the benefits of dental implants:
- Restore chewing and speech function
- Look like your natural teeth and improve self-esteem
- Reduce stress on remaining natural teeth by offering independent support
- Preserve jawbone and prevent loss of jaw height
- Straightforward to clean at home — though some implant bridges and full-arch restorations need floss threaders, interdental brushes, or a water flosser to clean underneath, plus routine professional cleanings
- Implant bodies can last decades; the visible crown may need replacement sooner8
Here are the disadvantages of getting dental implants:
- Will not whiten like your natural teeth
- Require invasive surgery for placement
- They are expensive, though the long-term benefits often justify the investment
- Bone grafting may be necessary before placement if you do not have enough natural jawbone remaining6
Dental Implant Procedure: Step-By-Step
Dental implant placement is outpatient surgery — you go home the same day.4 The full process takes several months because the implant must bond with your jawbone before the crown is attached.
Professionals who can perform dental implant surgery include:
The procedure breaks down into the following steps, depending on the number of implants you need:
1. Remove the Tooth
If the damaged tooth is still in your mouth, your dentist will extract it first. This step is skipped if the tooth is already missing.
2. Grafting and Jawbone Preparation
If your jawbone is too thin or soft to hold an implant, your surgeon will perform a bone graft to build up the site.6 Patients with upper-back-tooth bone loss may need a sinus lift — a type of bone graft that adds bone beneath the sinus floor. Grafts take a few months to heal before implant placement.
3. Implant Placement
During placement, the surgeon opens the gum, drills a precise channel into the bone, and positions the titanium implant where the tooth root used to sit.4
If a front tooth is being restored, your dentist fills the space with a temporary tooth while the implant heals beneath the gum. Back-tooth sites are usually left covered without a temporary.
4. Healing and Growth
Osseointegration begins as soon as the implant is in place — your jawbone grows around the titanium post and locks it in.1 This process takes several months and creates the stable foundation needed to support a permanent crown.
5. Abutment Placement (Crown Preparation)
Once the implant has integrated, your dentist attaches an abutment to the top of the implant post. The abutment extends just above the gum line so the crown has something to anchor to.
6. Crown Placement (Artificial Tooth)
After the abutment is placed, your dentist takes new impressions of your mouth. A dental lab creates a custom crown shaped and shaded to match your natural teeth, and your dentist cements or screws it onto the abutment.
7. Aftercare
Your surgeon will recommend over-the-counter or prescription pain medicine for the first few days. Antibiotics may be prescribed when clinically indicated, such as for higher infection risk or some grafting procedures.5 Stick to soft foods for the first week, keep the site clean, and avoid alcohol, caffeine, and tobacco during initial healing. Plan on regular follow-ups during the first few months and continue routine dental exams long term.
Side Effects and Complications of Dental Implant Surgery
Dental implant survival rates are high — most studies report 10-year survival above 90% — but complications can still occur. Careful planning, good oral hygiene, and follow-up lower risk, though some complications stem from surgical or health factors outside patient control.8
To reduce your risk, maintain good oral health care at home, including proper nutrition, brushing, and flossing.
As with any dental surgery, minor discomfort is normal. Common short-term side effects include:5
- Gum and face swelling
- Bruising on the skin or gums
- Minor bleeding
- Pain at the implant site
More serious complications, which are less common but possible, include:3,7
- Damage to surrounding teeth, gums, or blood vessels
- Infection at the implant site
- Prolonged bleeding
- Sinus issues and pressure (if the implant is placed in your upper jaw)
- Fractured jaw and jaw pain
- Nerve damage, which can cause tingling in the mouth or lips
For details about what the patient experience involves, see our dedicated guide.
How Much Do Dental Implants Cost?
Dental implant cost depends on the type, how many you need, your location, and the complexity of your case. A single-tooth implant typically runs in the low thousands; full-arch solutions like All-on-4 or full-mouth implants run into the tens of thousands per arch. For a complete cost breakdown by implant type, factors that drive price, and how insurance and financing work, see our dental implant cost guide and the dedicated dental implant insurance page.
When to See a Dentist About Dental Implants
See a dentist promptly if any of the following happen after implant surgery, or if you want to find out whether implants are right for you:
- Pain, swelling, or bleeding that worsens, does not improve with your prescribed medication, or comes with pus, fever, spreading redness, or warmth — possible signs of infection.5
- The implant feels loose or moves when you bite — a sign of implant failure or osseointegration problems.
- Numbness or tingling in your lip, chin, or tongue that does not resolve — possible nerve involvement.
- Prolonged sinus pressure or congestion — relevant if your implant was placed in the upper jaw.
- You are considering implants and want to know if you are a good candidate based on jawbone volume, gum health, oral hygiene, smoking status, healing ability, and conditions like uncontrolled diabetes. Start with our implant candidacy assessment.
A dentist or oral surgeon can examine the site, image the implant, and recommend treatment. Most post-op complications are easier to resolve when they are caught early.
Sources
- Gupta R, Gupta N, Weber KK. “Dental Implants.”StatPearls. StatPearls Publishing; last updated August 8, 2023. Accessed May 18, 2026.
- American Academy of Implant Dentistry. “Types of Implants and Techniques.” AAID.
- U.S. Food and Drug Administration. “Dental Implants: What You Should Know.” FDA, 2021.
- American Association of Oral and Maxillofacial Surgeons. “Dental Implant Surgery.” myOMS, last updated May 2021. Accessed May 18, 2026.
- American Association of Oral and Maxillofacial Surgeons. “Healing Process for Dental Implants.” myOMS, last updated July 2024. Accessed May 18, 2026.
- American Association of Oral and Maxillofacial Surgeons. “Bone Grafting and Membranes.” myOMS, last updated March 2020. Accessed May 18, 2026.
- National Institute of Dental and Craniofacial Research. “Dental Materials.” NIDCR, last reviewed January 2026. Accessed May 18, 2026.
- Kupka JR, König J, Al-Nawas B, Sagheb K, Schiegnitz E. “How far can we go? A 20-year meta-analysis of dental implant survival rates.”Clinical Oral Investigations. 2024;28:541. doi:10.1007/s00784-024-05929-3.
- American Association of Oral and Maxillofacial Surgeons. “Advantages of Implant-retained Dentures.” myOMS, last updated July 2024. Accessed May 18, 2026.

Experienced general dentist and adjunct professor. Advocates for preventive dentistry and dental education.
Related Articles
Types of Dental Implants and How Much Each One Costs
Wondering how much dental implants cost? We break down factors that affect implant pricing and explore different ways to...
What is a Single Tooth Implant?
Learn the benefits of a single tooth implant, how they work, the different types, and why you should consider getting on...
3 on 6 Dental Implants
3 on 6 dental implants are recommended for people who are missing most of their teeth. Learn more about 3 on 6 implants,...

Should I Get All-on-4 Dental Implants?
If you have missing teeth and want full functionality of your mouth back, All-on-4 dental implants may be right for you....
