What Are Common Oral Health Problems in Seniors?
Reader-supported. We may earn a commission from links on this page. Advertising disclosure.
In this article
Persistent oral health issues affect millions of older adults in the United States. From tooth loss and gum disease to dry mouth and oral cancer, these challenges are not just a matter of comfort; they’re closely tied to systemic health and quality of life.
This article offers a clear, data-backed look at the most common oral health problems affecting seniors and how these trends have evolved from 2019 through 2026.
2019–2026 Statistics
The following statistics offer a snapshot of oral health conditions among adults aged 65 and older in the United States.
-
In 2022, 63.7% of adults 65+ had a dental visit in the past year.
-
From 2017 to 2020, 13% of adults 65+ had untreated dental caries.
-
Root caries affected 16% of older adults, rising to 33% among those with low income.
-
The prevalence of periodontitis was 59.8% in adults aged 65+ (2017–2020).
-
Complete tooth loss affected 19.7% of adults aged 75+, compared to 11.4% of those aged 65–74.
-
Oral cancer incidence rates reached 44.8 per 100,000 for those aged 75+.
-
Only 56.4% of seniors without dental insurance saw a dentist in 2022.
-
ED visits for tooth disorders declined from 88.4 to 59.4 per 10,000 between 2014 and 2022.
-
States like Utah and Virginia expanded Medicaid adult dental benefits between 2019 and 2026.
What Changes With Age
Aging affects every part of the body, and your mouth is no exception. Several normal physiological changes raise the risk of oral health problems.
Saliva production tends to decrease with age, especially in people taking multiple medications. This condition, called dry mouth (or xerostomia), weakens the natural defenses that protect teeth from decay and the gums from infection.
At the same time, the gums naturally recede, exposing root surfaces that lack protective enamel. These shifts don’t guarantee problems, but they do make preventive care more important.
Key Conditions In Seniors
The most common oral health issues in older adults are distinct from those seen in younger people. The conditions below cause pain, interfere with eating, and increase the risk of other health complications.
Root Caries
Root caries refers to decay on the tooth root, which becomes exposed due to gum recession.
Unlike enamel, the root surface is covered by a softer material called cementum. This makes it more vulnerable to acid damage—especially when dry mouth limits the protective effects of saliva.
According to national data, root caries affects 16% of older adults and up to 33% of those with low incomes.
Periodontitis
Periodontitis is an advanced form of gum disease that leads to inflammation, infection, and loss of bone and tissue around the teeth.
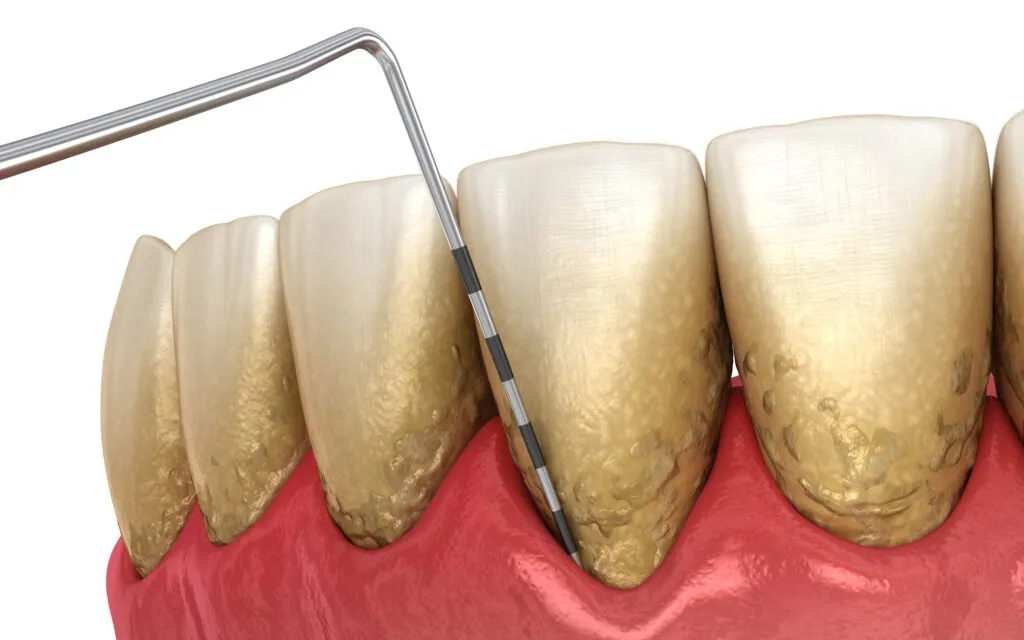
Periodontitis testing, gum recession process. Medically accurate 3D illustration
In the most recent CDC data, nearly 60% of seniors have some form of periodontitis. Rates increase with age: 71.5% of adults aged 65–74 and 81% of those 75 and older show signs of the disease.
Beyond the mouth, chronic inflammation from periodontitis has been linked with diabetes complications and cardiovascular risk.
Tooth Loss
Tooth loss still affects many older adults, though less so than in previous generations. In 2017–2020, the average number of remaining teeth was 21.7 for adults 65–74 and 19.8 for those 75+.
Complete edentulism (having no natural teeth) was found in 11.4% of seniors aged 65–74 and 19.7% of those aged 75 and older.
Tooth loss impacts nutrition, speech, and quality of life, especially when replacement options like dental implants are unaffordable or inaccessible.
Oral Cancer
Oral and oropharyngeal cancers are increasingly common in the senior population. In 2025, an estimated 59,660 new cases and 12,770 deaths are projected nationwide.
The incidence rate for adults 75 and older reaches 44.8 per 100,000 people. Survival is highly variable: 55% of white adults survive five years after diagnosis, compared to just 33% of Black adults.
By Region
Oral health disparities vary across the country. Access to preventive care, insurance coverage, and state policy shape these outcomes.
Table 1. Selected
Oral Health Metrics by Region, 2019–2026**
| Region | Metric | Year | Value |
|---|---|---|---|
| National | Untreated Caries (65+) | 2017–2020 | 13% |
| National | Periodontitis (65+) | 2017–2020 | 59.8% |
| National | Edentulism (75+) | 2017–2020 | 19.7% |
| New Hampshire | Medicaid Dental Benefit | 2019 | Emergency only |
| New York | Medicaid Dental Benefit | 2019 | Extensive |
| Utah | Medicaid Dental Benefit | 2025 | Extensive |
Top/Bottom Patterns:
-
Highest benefits: States like New York and Utah offer extensive Medicaid adult dental coverage.
-
Lowest access: Several Southern states still offer emergency-only coverage.
-
Geographic clustering: States with strong benefits tend to cluster in the Northeast and West.
These patterns reflect how state-level decisions affect care access.
Trends Since 2019
While many older adults retain more natural teeth than in the past, trends show ongoing challenges.
Between 2014 and 2022, the average annual rate of emergency department visits for tooth disorders decreased from 88.4 to 59.4 per 10,000 people.
This reflects better preventive access in some areas, but also suggests that seniors may delay care until problems are severe.
Tooth retention has improved, but disparities persist. From 2017 to 2020, complete tooth loss was nearly twice as common in those aged 75+ (19.7%) compared to those aged 65–74 (11.4%).
Who Faces the Highest Risk
Some seniors are more vulnerable to oral health problems due to long-standing disparities in income, education, race, and physical ability.
In 2022, only 35.3% of older adults living below the federal poverty level visited a dentist, compared to 80.5% of those with incomes over 400% of the poverty line. Education shows similar effects: dental visit rates ranged from 33.3% for those without a high school diploma to 82% for college graduates.
Racial disparities persist as well. More than half (52%) of Black adults have lost at least one tooth due to decay or gum disease, compared to 43% of all adults. Five-year survival rates for oral cancer are markedly lower for Black seniors (33%) than white seniors (55%), suggesting inequities in early detection and treatment.
Geography also matters. Older adults in rural communities often face “dental care deserts” with few nearby providers, limited transportation, and inconsistent Medicaid coverage.
Long-term care facilities face their own barriers. Only 16% of nursing home residents reportedly receive daily oral care—a problem often linked to staffing shortages and a lack of caregiver training.
These disparities are not just about teeth. They reflect broader inequities in health care access, resources, and outcomes.
Care Access and Coverage
Access to oral health care in older adults is closely tied to insurance status. In 2022, 69.6% of seniors with dental insurance had seen a dentist in the past year, compared to just 56.4% of those without coverage.
Unfortunately, traditional Medicare does not cover routine dental care. Coverage is limited to “medically necessary” procedures, such as dental exams before organ transplants or treatment of infections prior to heart surgery. Medicare Advantage plans may offer expanded benefits, but access remains inconsistent.
Medicaid is different. Each state decides whether to cover adult dental services. Some, like New York and Utah, provide extensive benefits. Others offer only emergency services—or none at all. Between 2019 and 2026, several states (e.g., Utah, Virginia) expanded their Medicaid dental offerings, setting examples for others to follow.
Community health centers (FQHCs) also play a vital role. They provide dental services on a sliding fee scale, and many offer care tailored to older adults. However, appointment availability and service scope can vary.
Definitions and Measurement
Understanding oral health data requires clarity on how conditions and metrics are defined.
-
Untreated dental caries: Active cavities not filled or restored; measured via oral exams (NHANES).
-
Root caries: Decay affecting exposed root surfaces; more common with gum recession and dry mouth.
-
Periodontitis: Gum disease defined by clinical attachment loss and probing depth; CDC/AAP criteria.
-
Edentulism: Complete tooth loss; self-reported in BRFSS and clinically confirmed in NHANES.
-
Oral cancer: Includes oral cavity and oropharynx; measured as incidence per 100,000 people (SEER).
-
Dental visit rate: % of people reporting a visit in the past year (NHIS, BRFSS).
-
Medically necessary dental care: Services integral to other covered medical procedures (CMS definition).
Rates may be reported as:
-
Prevalence: % of population with the condition.
-
Incidence: New cases in a specific time frame.
-
Per-capita rate: Often per 10,000 or 100,000 people.
-
Age-standardized rate: Adjusted to account for population aging.
Methods And Data Notes
This article draws from national datasets covering the years 2017 through 2026:
-
NHANES (2017–Mar 2020, 2021–2022): Clinical exam data on caries, tooth loss, periodontitis.
-
NHIS & BRFSS (2019–2024): Self-reported data on dental visits, insurance status, health disparities.
-
SEER (2019–2023): Cancer incidence and survival by age, race, and site.
-
CMS & MACPAC: Medicare claims rules and Medicaid benefit status by state.
-
HRSA UDS (2019–2024): Dental service encounters at FQHCs.
-
WHO Global Oral Health Report (2022): International context on aging and oral disease.
-
CareQuest Institute (select briefs): Supplemental insights on access and equity.
Data handling:
-
Survey data weighted for national estimates.
-
Age-standardization used for comparisons across groups.
-
Cancer rates shown per 100,000; ED visits per 10,000.
-
Prevalence reported to one decimal point.
-
Missing/suppressed data flagged where n<30 or RSE>30%.
-
Where 2021–2022 NHANES data were incomplete, 2017–2020 figures were used with cycle note.
What Are Common Oral Health Problems In Seniors
NewMouth PodcastSources
- Centers for Disease Control and Prevention. “National Health and Nutrition Examination Survey, 2017–March 2020, 2021–2022 datasets and documentation.” CDC.gov, 2023.
- Centers for Disease Control and Prevention. “Behavioral Risk Factor Surveillance System (BRFSS) prevalence and trends data, 2019–2024.” CDC.gov, 2024.
- Centers for Disease Control and Prevention. “National Health Interview Survey: 2019–2022 survey tables and documentation.” CDC.gov, 2023.
- National Cancer Institute. “SEERExplorer: Oral cavity and pharynx cancer statistics, 2019–2023*.” NCI SEER, 2023.
- Centers for Medicare & Medicaid Services. “Calendar Year (CY) 2024 Medicare Physician Fee Schedule Final Rule: Dental services that are inextricably linked to covered medical services.” CMS.gov, 2023.
- Medicaid and CHIP Payment and Access Commission. “State Medicaid adult dental benefits: 2019–2025 tracker.” MACPAC.gov, 2025.
- Health Resources and Services Administration. “Uniform Data System (UDS): Federally Qualified Health Center dental service data, 2019–2024.” HRSA.gov, 2024.
- World Health Organization. “Global oral health status report: Towards universal health coverage for oral health by 2030.” WHO.int, 2022.
- CareQuest Institute for Oral Health. “State of Oral Health Equity in America 2023 report.” CareQuest Institute for Oral Health, 2023.
- U.S. Department of Health and Human Services. “Healthy People 2030 objectives: Oral conditions.” Health.gov, 2023.
- American Academy of Periodontology & CDC. “Case definitions for surveillance of periodontitis: CDC–AAP 2012 case definition.” Journal of Periodontology, 2012.
- Centers for Disease Control and Prevention. “United States Cancer Statistics (USCS): Oral and oropharyngeal cancer data.” CDC.gov, 2023.

Experienced general dentist and adjunct professor. Advocates for preventive dentistry and dental education.
Related Articles
Dental Care for Teens and Young Adults (Life Stages)
What are the dental care needs of teens and young adults? Learn common concerns, treatments, procedures, and how to choo...
Oral Health Basics for Adults
Adult dental care is essential for maintaining your quality of life. Here are eight ways to maintain good oral health pl...

6 Tips to Teach Your Child About Dental Health
Discover everything you need to know about children's dental health, from losing baby teeth to common dental conditions...

Oral Health for Babies and Toddlers
Dental care should start before your baby's first tooth appears. Here's how to maintain your baby's oral health from bir...
