Root Canal Infection Symptoms
Reader-supported. We may earn a commission from links on this page. Advertising disclosure.
In this article
If you’ve had a root canal and the same tooth starts bothering you again, you’re not alone, and you’re not imagining it. While root canal therapy is generally successful, it’s still possible for a treated tooth to become re-infected months or even years later.
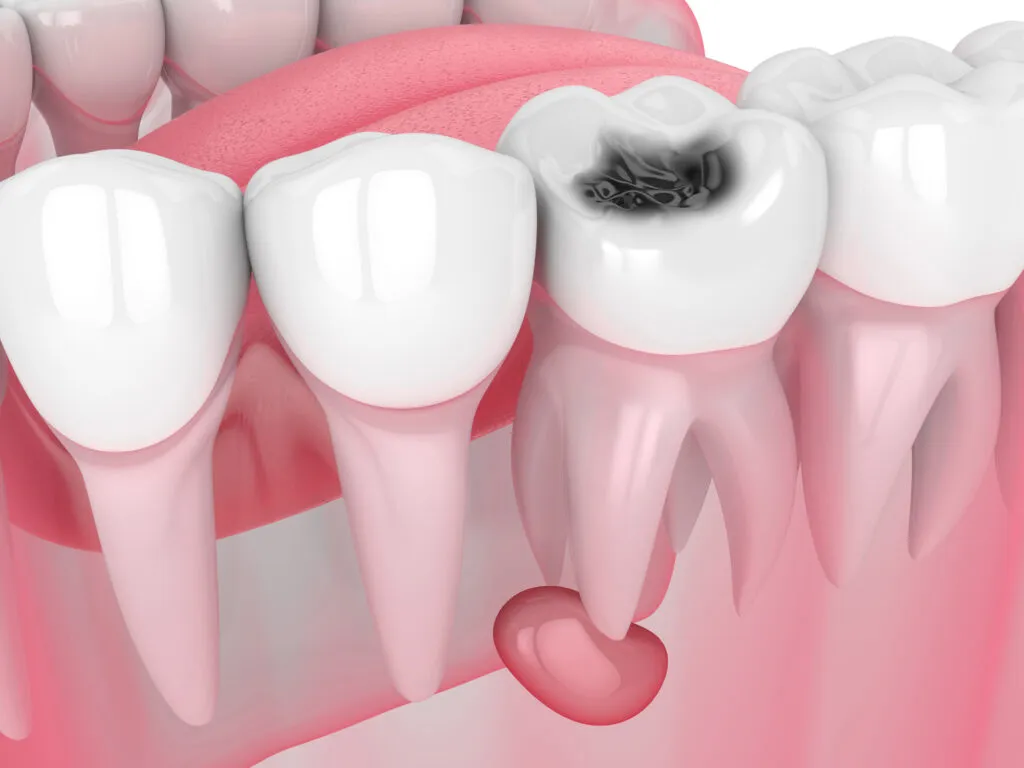
Recognizing the signs early and knowing what to do next can help you get relief and avoid further complications.
What Causes a Root Canal Infection?
A root canal infection happens when bacteria enter the inner chamber of a tooth, either because the initial treatment didn’t fully remove the infection or because bacteria found their way back in later. This is sometimes called a “failing root canal.”
Even though most root canal treatments work well, a small percentage fail over time. Cracks in the tooth, delays in getting a permanent crown, or new cavities near the treated area can create paths for bacteria. You may not notice a problem at first, but over time, symptoms can develop.
If you’ve had a root canal and your symptoms return or worsen, it’s worth having a dentist or endodontist evaluate the tooth.
Symptoms of a Root Canal Infection
Pain or pressure near a tooth that has had a root canal is a common warning sign, especially if it lingers or worsens over time. Other changes in the gums, taste, or tooth appearance can also signal a problem.
Watch for the following symptoms:
-
Persistent tooth pain or pressure — Pain may feel sharp, throbbing, or dull and achy. It can come and go or remain constant. Pain that feels different from normal sensitivity or steadily worsens should be evaluated.
-
Pain when biting or chewing — Discomfort is often more noticeable when biting down, especially on hard foods or when clenching your teeth.
-
A feeling that the tooth hits first when you bite — The treated tooth may feel slightly raised or tender, making your bite feel uneven.
-
Soreness in nearby teeth — Inflammation or subtle bite changes can cause discomfort in surrounding teeth, even if they weren’t treated.
-
Gum swelling near the treated tooth — Swelling that lasts more than a few days, returns repeatedly, or feels tender when pressed can point to infection.
-
A pimple-like bump on the gums — This bump may drain pus or clear fluid and often signals an abscess beneath the surface.
-
A persistent bad taste or odor — A foul taste or smell that keeps coming back—even after brushing—can result from fluid draining from an infected area.
-
Pus or discharge from the gums — Any visible drainage near the tooth is a sign that the infection may still be active.
-
Bad breath that doesn’t improve — Ongoing infection can cause halitosis that regular oral hygiene doesn’t resolve.
-
Tooth discoloration — A tooth that turns gray, bluish, or noticeably darker than surrounding teeth may indicate internal damage or reduced blood flow. While not always urgent, it should be mentioned to your dentist.
If several of these symptoms appear together—especially pain with swelling—it’s a strong signal that the tooth needs to be re-evaluated.
Why Do Root Canals Fail?
Root canals can fail when bacteria re-enter the tooth or were never fully removed the first time. This isn’t always due to error—sometimes anatomy or timing plays a role.
The most common causes include:
Cracks
Tiny cracks can form in the tooth, especially after trauma or heavy grinding. These cracks may allow bacteria to reach deep areas that are hard to clean.
- Vertical root fractures are especially hard to detect.
- Nighttime clenching or grinding increases the risk over time.
- Undetected cracks may have been present before the original root canal.
If your dentist suspects a crack, they may recommend imaging or a referral to a specialist.
Restoration Leaks
After a root canal, the tooth requires a permanent filling or crown to seal it. If this restoration is delayed, damaged, or doesn’t fit well, bacteria can sneak in.
- Delays in getting a crown increase the risk of reinfection.
- Loose fillings or crowns can break the seal.
- Decay near the edge of a crown may allow entry points for bacteria.
Keeping your restoration intact is key to protecting the work already done.
New Decay
A root-canaled tooth can still get a cavity. You may not notice it right away, since the tooth’s pulp (nerve tissue) was removed, but decay can still damage the seal and reintroduce infection.
Regular dental cleanings and plaque control help prevent this. Reinfection isn’t always avoidable, but many cases are preventable.
Can a Root Canal Infection Spread?
If untreated, a root canal infection can spread beyond the tooth. While serious complications are rare, they’re possible.
Watch for:
- Facial swelling, especially if it’s spreading.
- Fever, chills, or general illness alongside dental pain.
- Difficulty swallowing or breathing, which requires emergency care.
Most dental infections stay localized, but worsening symptoms always deserve prompt attention.
When Should You Call a Dentist?
Don’t wait if something feels off. Pain, swelling, or other new symptoms after a root canal are reasons to call.
Here’s when to reach out:
You should call your dental provider right away if:
- You have facial swelling, especially if it’s getting worse.
- You feel feverish or unwell, along with tooth pain.
- There’s drainage or pus near a previously treated tooth.
- The pain wakes you up at night or affects daily tasks.
These signs may indicate an active infection needing immediate care. Even if symptoms aren’t severe, call your provider this week if:
- Your bite feels off, or a treated tooth feels sore again.
- You notice a pimple or bump on your gum that comes and goes.
- Your tooth is turning dark or looks different from the others.
- It’s been a while since your last X-ray, and you have mild symptoms.
Most failing root canals can be treated, but earlier intervention often makes treatment easier.
How Dentists Diagnose a Root Canal Infection
A dentist doesn’t diagnose a failing root canal based on pain alone. The goal is to find out why the tooth hurts again so the treatment actually fixes the problem.
The evaluation usually starts with your symptom history and a focused exam, because timing, triggers, and changes since your original procedure matter.
Exam
During the exam, your dentist checks the tooth and surrounding tissues for signs of inflammation or infection. This may include tapping on the tooth, checking your bite, and gently pressing on nearby gums.
They also look for cracks, loose restorations, or decay around the treated tooth, which can explain why bacteria got back in.
Imaging
Dental imaging helps confirm what’s happening beneath the surface. Standard X‑rays can show bone changes or infection around the root tip.
In certain cases, your dentist may recommend 3D imaging, which provides a clearer view of complex root anatomy, hidden cracks, or areas that are hard to see on regular X‑rays. This isn’t routine for every patient, but it can be useful when symptoms don’t match earlier findings.
Testing
Additional tests help narrow down the diagnosis. These may include hot or cold testing on nearby teeth, checking gum pocket depths, or using magnification to look for missed canals or tiny fractures.
Once the cause is clear, your dentist can explain which treatment option makes the most sense and why.
Bring a brief timeline of your symptoms to the appointment so the diagnosis is faster and more accurate.
Treatment Options to Save the Tooth
When a root canal treatment fails, management usually falls into one of three categories. The best option depends on the cause of the problem, the condition of the tooth, and your overall oral health.
In most cases, dentists focus on saving the tooth when possible. Your treatment options for a root canal infection include:
- Retreatment — Your dentist reopens the tooth, removes the old filling material, cleans the canals again, and reseals them. It allows the dentist or endodontist to address areas that were previously hard to reach.
- Apical surgery — The dentist accesses the root tip through the gum, removes infected tissue, and seals the end of the root. It’s typically recommended when canals are blocked or anatomy prevents full cleaning from the top.
- Extraction — If the tooth can’t be saved, removing the tooth removes the source of the infection, though you may still need additional treatment (for example, drainage and/or antibiotics) depending on how far the infection has spread.
Recovery and Follow-Up Visits After Treatment
What happens after treatment plays a big role in long‑term success. Some soreness is normal, but symptoms should steadily improve.
Treatment may require one or more visits, depending on the selected option. Follow‑up appointments allow your dentist to confirm healing and adjust the plan if needed.
During the first few days, it’s common to experience mild tenderness. Pain that worsens rather than improves, or swelling that spreads, should be reported promptly.
Permanent Restoration
After retreatment or surgery, the tooth usually needs a permanent restoration—often a crown—to protect the seal and prevent reinfection.
Delaying this step increases the risk of failure, even if the internal treatment was successful. Finishing the restoration helps preserve the tooth for the long term. If a crown is recommended, schedule it as soon as your dentist advises.
How to Lower Your Reinfection Risk
While not all failures are preventable, daily habits and follow‑through after treatment make a real difference.
Focus on consistent care and protection.
- Thorough brushing and cleaning — Remove plaque daily to reduce bacterial buildup.
- Regular dental checkups — Allow early detection of cracks, leaks, or decay.
- Protecting the tooth — Use a night guard if you grind or clench.
- Gentle rinsing when advised — Helps keep the area clean during healing.
If any signs of infection return, call your dentist rather than waiting.
Sources
- American Dental Association. “Antibiotics for Dental Pain and Swelling.” ADA.org, 2022.
- European Society of Endodontology. “Resources for Clinicians (includes “Quality guidelines for endodontic treatment” listing).” e-s-e.eu, 2020.
- American Association of Endodontists. “Guide to Clinical Endodontics.” AAE.org, 2021.
- National Institute of Dental and Craniofacial Research. “NIDCR homepage (federal oral health research institute; root-canal-related content is housed under News/Topics).” NIDCR.nih.gov, 2023.
- Centers for Disease Control and Prevention. “Oral Health (dental health basics, including oral disease and infection-related resources).” CDC.gov, 2022.

Licensed dental specialist focusing on personalized dental content writing and blogging.
Related Articles

When to Eat Solid Food After Tooth Extraction
When can you eat solid food after a tooth extraction? Read on for a complete guide on the healing timeline, plus what to...

What's the Difference Between a Dentist and a Periodontist?
Dentists have many specializations, including periodontists. This article talks about the difference between the differe...

Is Dental Insurance Worth It?
Dental insurance can be worth it, depending on your needs, the plan you purchase, and your financial situation. Research...
Laser Teeth Whitening: Pros, Cons, & Costs
Laser teeth whitening uses light energy to break down stains on tooth enamel. Learn more about the cost and how it works...
