Alzheimer's and Oral Health
Reader-supported. We may earn a commission from links on this page. Advertising disclosure.
In this article
Recent studies uncovered evidence of a connection between oral health and Alzheimer’s disease. Researchers must conduct larger studies to confirm this relationship, but periodontal disease and Alzheimer’s appear linked.
In 2020, the National Institute on Aging found that the bacteria associated with gum disease may also be associated with the development of Alzheimer’s and other dementias.
Link Between Gum Disease and Alzheimer’s
Just as oral health is a known indicator of overall health, gum disease may indicate the likelihood of developing Alzheimer’s disease. Two recent studies point to this connection.
A 2021 study found that older adults with more harmful than healthy bacteria in their gums are likelier to have evidence for amyloid beta in their cerebrospinal fluid. Amyloid beta is a key biomarker for whether someone will develop Alzheimer’s.
However, the study did not find an association between harmful gum bacteria and tau, another key biomarker for Alzheimer’s.
Meanwhile, a 2019 study found that the bacteria that causes gum disease (Porphyromonas gingivalis) can move from the mouth to the brain. Once in the brain, the bacteria can release enzymes that destroy nerve cells, possibly leading to memory loss and Alzheimer’s.
These findings suggest that gum disease can contribute to the development of Alzheimer’s. While more research is necessary to confirm this link, it only strengthens the case for taking care of oral health at all ages.
What Is Alzheimer’s Disease?
Alzheimer’s disease is a progressive decline of the nervous system, mostly in the brain, that leads to reduced cognitive function. People with Alzheimer’s slowly lose their ability to perform regular social and behavioral tasks over time.
The symptoms of Alzheimer’s disease include:
- Memory loss
- Poor judgment
- Having trouble with routine tasks
- Getting lost or misplacing items
- Mood and personality changes
Due to the disease’s progressive nature, symptoms will worsen over time. People with advanced Alzheimer’s will need a caretaker to help them with daily life.
Causes and Treatment of Alzheimer’s
The cause of Alzheimer’s disease is not yet fully understood. Scientists suspect multiple factors may all play a role in developing Alzheimer’s.
These factors include:
- Changes in the brain
- Genetics
- Environmental factors
- Lifestyle factors
At this time, there is no cure for Alzheimer’s disease. However, doctors may prescribe certain medications to manage symptoms in the approximately 7.2 million Americans aged 65 and older who have Alzheimer’s disease.
What Is Gum Disease?
Gum disease is an infection of your gums or the tissues that hold your teeth in place. The dental plaque that accumulates on your teeth causes gum disease.
The bacteria living in plaque produce toxins that penetrate the gum tissue, triggering inflammation. Like Alzheimer’s, gum disease is progressive, and more advanced stages can affect different parts of your mouth.
Gingivitis
Gingivitis is mild gum disease. In its earliest stages, inflammation affects only the edge of the gum tissue where it meets the teeth.
Signs of early-stage gum disease include:
• Redness • Swelling • Tenderness • A tendency to bleed
Gingivitis is reversible when addressed early by dental care and good oral hygiene.
Periodontitis (Periodontal Disease)
Gum disease worsens to periodontitis when the inflammatory response destroys the ligaments and bones surrounding the teeth. Periodontal disease is often accompanied by a transition from acute to chronic inflammation.
The signs of chronic inflammation in your gums are easy to miss but might include:
- Red, swollen, or receding gums
- Bleeding gums
- New gaps between teeth or change in bite
- Loosening teeth
- Bad breath
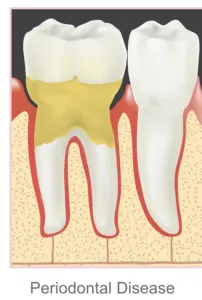
As untreated, periodontal disease destroys the attachment between the bone and teeth, and deep pockets or crevices form. These pockets are perfect places for oral bacteria to continue to collect. They may deepen and even lead to lost teeth.
How Do I Know If I Have Gingivitis or Periodontitis?
The early stages of gum disease are difficult to notice at first. Some people may not feel any pain from gingivitis. Others may notice:
- Swollen, red, or tender gums
- Bleeding from the gums
- Bad breath
Advanced gum disease (periodontitis) includes those same symptoms as well as:
- Inflammation around the teeth that may extend under the gums
- Loose teeth
- Tooth sensitivity when consuming hot or cold substances
- Gum recession (when the gums pull away from the teeth)
- Pus between the gums and teeth
- Sudden tooth misalignment
- Partial dentures that do not fit properly anymore
Gum Disease and Overall Health
A chronically unhealthy mouth affects the rest of the body. Scientists are actively researching the role of chronic inflammation in diseases besides Alzheimer’s, including:
- Diabetes
- Heart disease
- Cancer
So far, research shows that chronic gum disease can have a disastrous effect on the body.
Bacteria from gum disease can spread throughout the body, potentially worsening major health problems. To keep your whole body healthy, see your dentist regularly and practice good oral hygiene at home.
Read more about gum disease and its causes.
Summary
Gum disease is an inflammation of the gums that, if untreated, can lead to oral health problems and tooth loss. Early research suggests that it may also play a role in developing or indicating the possibility of Alzheimer’s disease.
One study shows that harmful bacteria in the gums may be associated with a biomarker for Alzheimer’s found in the cerebrospinal fluid. Another indicates that bacteria can travel from the mouth to the brain and destroy nerve cells, potentially leading to Alzheimer’s.
More evidence is needed to determine the correlation between gum disease and Alzheimer’s, but we know that oral health is connected to overall health. Practice good oral hygiene at home and visit your dentist every six months to prevent gum disease.
Sources
- Beydoun et al. “Clinical and Bacterial Markers of Periodontitis and Their Association with Incident All-Cause and Alzheimer's Disease Dementia in a Large National Survey.” Journal of Alzheimer’s Disease, National Library of Medicine, 2020.
- “What Are the Signs of Alzheimer’s Disease?” National Institute on Aging, National Institutes of Health, 2022.
- “What is Alzheimer’s Disease?” Alzheimers.gov, National Institutes of Health, 2023.
- “Alzheimer’s Disease Facts and Figures.” Alzheimer’s Association, 2023.
- “Imbalance in Gum Bacteria Linked to Alzheimer’s Disease Biomarker.” New York University, 2021.
- Dominy et al. “Porphyromonas gingivalis in Alzheimer's disease brains: Evidence for disease causation and treatment with small-molecule inhibitors.” Science Advances, National Library of Medicine, 2019.
- “Periodontal (Gum) Disease: Causes, Symptoms, and Treatments.” NIH Publication, National Institutes of Health, 2013.
- “Periodontal Disease in Adults (Age 20 to 64).” National Institute of Dental and Craniofacial Research, U.S. Department of Health and Human Services, 2021.
- Shoemark, D., and Allen, S. “The Microbiome and Disease: Reviewing the Links Between the Oral Microbiome, Aging, and Alzheimer’s Disease.” IOS Press Content Library, 2015.
- Watts et al. “Inflammation as a Potential Mediator for the Association between Periodontal Disease and Alzheimer's Disease.” Neuropsychiatric Disease and Treatment, Dove Medical Press, 2008.

Experienced general dentist and adjunct professor. Advocates for preventive dentistry and dental education.
Related Articles

8 Tips to Keep Your Teeth Healthy While Traveling
If you want to know how to keep your teeth healthy while traveling, here are eight tips you can do before and during you...
Black Triangles Between Your Teeth
When you look in the mirror, you may notice small black triangles between your teeth. These are gaps that your gum tissu...

Are Tonsil Stones Contagious?
Are Tonsil Stones Contagious? No, tonsil stones are not contagious, nor are they serious health problems. While tonsil s...

The Benefits of Dental Probiotics
Your body is home to a unique set of microbes, and about 700 species live in your mouth. 5, 7 These include microscopic...
